 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube
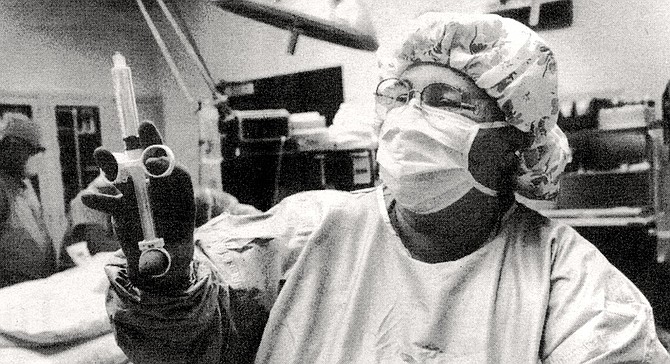
A sharp, schoolteacher’s voice barks, “You can change in there.”
I’m directed into a change room. The room has a high school P.E. quality to it. There are three rows of small, steel lockers, a wooden bench, one large vanity mirror over an oval sink, and showers in an adjoining room. I slip out of street duds, don blue pants, smock, shower cap, stretch blue booties over my loafers.
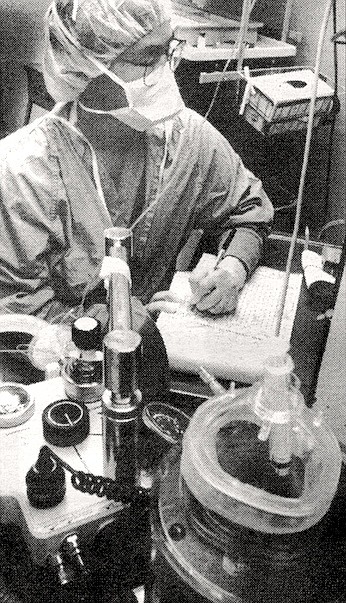
This is Sharp’s Chula Vista Medical Center, more precisely, the working end of Sharp Hospital, the operating room area. Sharp has seven operating rooms, 216 licensed acute beds, 325 physicians. It’s the most comprehensive medical center in the South Bay.
I finish changing, step through another door into a speckled linoleum hallway, and regard a dozen men and women dressed like me. I am introduced to the charge nurse for the day, Donna Fry. She is what used to be called a ‘handsome woman.’ She’s in her late 20s, has an oval, pale face, and long dark hair.
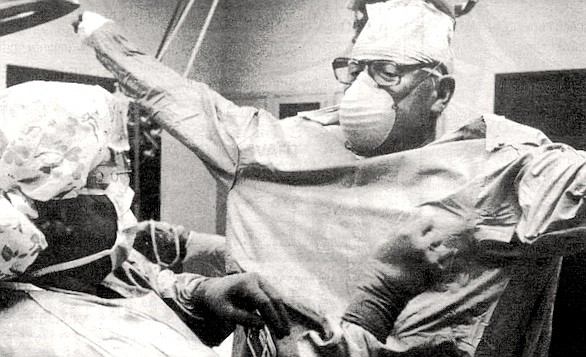
I look to my left. Down the hallway is a room Filled with five patients lying on hospital roll-away beds. Fry nods towards them, says, “We have a pre-op check list. We make sure that the consent form is signed correctly, see if the patient has any allergies, ask the last time he had anything to eat and drink, if he has any dentures, loose teeth, jewelry. Go over the lab work. It’s a double check.” Fry continues, “We have three general surgeries and a cath lab. A cath lab is where they thread a catheter through the arteries to see how the arteries around the heart are doing, see if they’re blocked. The heart program and cath lab are very strong here.”
We walk on, make a left through wide doors. “This is the inner core, just put on your mask.” The mask I’d been wearing loose is brought up snug over my nose and mouth. We enter a rectangular room filled with medical equipment. Four operating rooms feed into this inner core.
Fry explains, “This is where we keep our sutures. If we need to flash sterilize something, like if the surgeons need something they’ve already used we can sterilize it in here. And we have our warmers, they warm instruments; we like to use warm instruments when possible.”
Fry nods to her right, “In there is our ortho room. We do a lot of total hip replacements, and over there is our old heart room, we use it for general surgery now.”
We walk back to the main hallway. I am shown a large bulletin board hung on the wall. “This is the surgical board, it lists the cases for today.” Fry points to a row of carts parked along the wall, each one loaded with instruments. “We take all the supplies and put them on those carts. Surgeons have their own preference card listing everything he likes to use. And every surgeon is different. It’s the art of a good circulating nurse to know the surgeon and know what he wants. Before a case starts, the nurse takes everything from here into the O.R., opens everything up, scrub nurses scrub every item, then set up all the instruments that will be used.”
We continue along the main corridor. Fry introduces me to Linda Karmon, scrub nurse. Karmon is over 40, has hazel eyes, dark hair. She’s maybe five-foot five. I lean against the wall and ask, “You’re the scrub nurse, what do you do during an operation?”
“I pass the instruments. The doctor says something and I give it to him, or, best of all possible worlds, I have anticipated his needs and there doesn’t have to be any talking. You can do that once you’ve done enough of the same kinds of cases with the same doctor. Each doctor has their likes and dislikes.”
“How many instruments do you handle?”
“It depends on the procedure, this is just a basic setup,” a steady hand points towards the nearest surgical cart. “That one is called a Minor set and there are Kellys, and a couple of retractors. This stuff is for a pretty simple procedure. Of course, we have clamps; you use them in a lot of surgeries because of bleeders. And you always have suctions, a Bovie, and electric pump.”
We walk into an empty operating room. On a wall shelf is an ancient Sony AM-FM radio playing soft rock. For the first time the surroundings seem familiar, like the neighborhood auto mechanic shop. We pass through, I ask, “What are the shift hours here?”
“The day shift is 6:30 a.m. to 3 o’clock. The p.m. shift is 2:30 until 11 o’clock, and we do not have a night shift.”
Linda takes me into the Cysto room. “This table is set up so that they can do X-ray procedures without moving the patient. The table tilts and all kind of things, costs a $100,000, and...” Linda moves both hands to the joint where the table top and stainless steel column meet the frame, and shakes. We hear a rattle from within that sounds like a steel baby-rattle, “...it’s not even six months old.”
I look into clear, hazel eyes and think, “Where to start this?” I cough, ask, “I hear a New York accent. How did you get to California?”
“Oh, my god. Took a vacation, liked it, stayed. Came to visit some friends, went to L.A. for a little while, but San Diego is much quieter.”
“Where did you get your degree?”
“I went to a tech school in Mississippi.”
I roll both eyes, laugh. “It was either Mississippi or Paris?”
“Yeah, they’re about the same. I got accepted in Mississippi.”
“Did you always want to be a nurse?”
“When I lived in Washington, I got a chance to see surgery and that was it. Once I saw it, I said, ‘Yes, this is for me.’ It’s very exciting, different every day.”
“What was it like the first time you saw a surgeon rip open a chest?”
“It was amazing. It didn’t bother me, because the patient is usually draped out, so you’re not seeing a face, you’re not seeing any body parts except that little section left uncovered. Contrary to popular belief, you do not bleed. An operation is not a bloody thing. They don’t want you to bleed. When you open up somebody, the blood isn’t there, it’s in veins and arteries. Doctors try very hard not to cut a vein or artery.”
“Is there a sound to it, when you cut open flesh?”
“The sound that you get in the O.R. is from an electric cautery machine. There’s definitely a smell. When I first started surgery it was clamp, clamp, cut, which means clamp, clamp both sides of a vein or an artery, cut it and tie. Now it’s this little pencil attached to a cautery machine that cuts and coagulates at the same time. It creates smoke, burning flesh is what it is.
“I did this in Manhattan ten years ago and it’s very different now. Nowadays it’s all lasers. Everything is video, which means it’s not only what your eyes can see, but if you’re working through a camera one drop of blood looks like, well, it looks big.”
“How long have you been a scrub nurse?”
“I took a five-year hiatus to run a motel,” she laughs. “Many lives. Altogether, I’ve been in nursing 14 years.”
“What is the difference between a real operation and what you see on TV?”
“If I look at a show I can see that maybe the tube isn’t placed right, or the bleeding isn’t right, it’s more dramatic on television, but not that much more. In real life it’s very controlled, there’s no wasted steps. Hardly anybody ever dies in the operating room. They get you out of here and you die somewhere else.”
“How has the operating room changed since AIDS?”
“There’s a thing called 'universal precaution’ now. They did not have that before AIDS. Now, every case we have is considered a contaminated case, which requires a different procedure. I have dealt with a lot of friends who have died of AIDS; I know how it can be frightening to some people. It’s not frightening to me. If the sharp instruments are dealt with in the proper manner, you won’t get hurt. I’m not going to catch AIDS by touching somebody.”
“What’s the most dangerous moment in surgery?”
“I think intubation for anesthesia. Intubation is when a patient’s going under anesthesia and the tube has to go in. That’s not my part of it.”
“What’s your day like?”
“Well, we have to be here at 6:30 a.m., and start surgery at 7:30. When we walk into work, there’s a board on the wall that lists the surgeries, and then you know where you are going to be. You’re usually in that room for the whole day unless everything is changed around, or something is canceled. We get off at 3 o’clock. Today is a very mellow day; some days, it’s just one operation after the other.
“Anyway, they roll the patients in. Whoever’s scrubbing the case is already in the operating room, making a sterile field, setting up the instruments. A nurse is helping with the patient and helping the anesthesiologist. The doctors are inside scrubbing their hands; I’ve already done that a long time ago. The doctors come in, we gown them so they become sterile. Then they drape out the patient with sterile towels and a sterile sheet, so the only thing that’s open is this little spot on the body that’s going to be operated on, which has already been prepped by the nurse. Then the case starts.”
“How many instruments do you have to remember?”
“There’s a huge amount, but a lot of instruments are the same, just different sizes. They’re little ones because it’s the beginning of the operation, or they’re longer because the doctors are going in deeper, but it’s the same type of instrument, just a little longer. OB-GYN has their own instruments, as does Ortho, General, Neural, and so on.”
“Do you scrub all the surgeries?”
“I don’t do hearts, they have a heart team. I haven’t done total joints because there’s a team there, too.”
“Are those the glamour positions?”
“Heart is a glamour position. Orthopedic, yeah, I guess that is too. Ortho’s a lot of work, a lot of heavy instruments — they are heavy, heavy.”
“What’s it like when you put your hand inside an opened body?”
“It’s warm and wet, there is a wetness. We’re 90 percent seawater, or something like that, so inside, everything is smooth next to each other, there’s nothing rough.”
We walk out into the corridor, meander into the instrument cleaning room. Karmon stands over a tray of worn but immaculately clean operating instruments. “Now this is a weighted specula that goes into the vagina.”
I look at a gigantic stainless steel thing; it looks like a mutated shoe horn. “Good God.”
“Yeah, it looks like ancient stuff. These are more modern looking.” Linda picks up a delicate instrument. “This is a forcep, like a jeweler would have forceps.”
“This stuff must cost a fortune.”
“I think each one of these costs $25. Now this,” quick hands pick up a large, ugly, steel object, “is called Connor-O’Sullivan, which is a retractor you put in a stomach, and then you open up the stomach, and then the doctor works in there. You can be opened up this far...” Karmon opens the retractor; the thing becomes an enormous gaping hole like the jaws of a white shark.
“Auuuugh.”
She laughs. “Actually, it goes very easy. For a layperson it’s weird. This is a small retractor, they have much bigger ones.”
I turn away, mumble. “Being a nurse for 14 years, is it like going to work now?”
“Yes, yes. It is going to work. Interesting though. Yesterday they took out a kidney. I hadn’t touched a kidney in years, you get taken aback when they hand you a kidney. Same thing with an amputation. A leg has a very different feeling when it’s not connected to you, when they just hand it over to you. It’s a very weird feeling.” “What do you do with it?” “It’s covered, first of all. It’s handed to me, then I hand it to the nurse, or put it in another bag, and it’s tagged. Any body part or piece that comes out of the patient goes to the lab. And for a leg or things like that, there might be a religious reason, it might have to be buried, depends on what the person decides.”
“Do they have a storage facility for legs and arms?”
“No.”
“What was the first body part you saw?”
“When I first started as an aide, as a kid, I got to go through OB. And they used to save placentas. And they put them in an icebox — placentas — because they made an antibiotic from them. So, I was a kid, I saw my first delivery, and I couldn’t stop crying, it was just amazing, and then I started fooling around, looking around, opened a freezer — like an ice cream freezer in those days — and there was these placentas.”
“Auuugh!”


A sharp, schoolteacher’s voice barks, “You can change in there.”
I’m directed into a change room. The room has a high school P.E. quality to it. There are three rows of small, steel lockers, a wooden bench, one large vanity mirror over an oval sink, and showers in an adjoining room. I slip out of street duds, don blue pants, smock, shower cap, stretch blue booties over my loafers.

This is Sharp’s Chula Vista Medical Center, more precisely, the working end of Sharp Hospital, the operating room area. Sharp has seven operating rooms, 216 licensed acute beds, 325 physicians. It’s the most comprehensive medical center in the South Bay.
I finish changing, step through another door into a speckled linoleum hallway, and regard a dozen men and women dressed like me. I am introduced to the charge nurse for the day, Donna Fry. She is what used to be called a ‘handsome woman.’ She’s in her late 20s, has an oval, pale face, and long dark hair.

I look to my left. Down the hallway is a room Filled with five patients lying on hospital roll-away beds. Fry nods towards them, says, “We have a pre-op check list. We make sure that the consent form is signed correctly, see if the patient has any allergies, ask the last time he had anything to eat and drink, if he has any dentures, loose teeth, jewelry. Go over the lab work. It’s a double check.” Fry continues, “We have three general surgeries and a cath lab. A cath lab is where they thread a catheter through the arteries to see how the arteries around the heart are doing, see if they’re blocked. The heart program and cath lab are very strong here.”
We walk on, make a left through wide doors. “This is the inner core, just put on your mask.” The mask I’d been wearing loose is brought up snug over my nose and mouth. We enter a rectangular room filled with medical equipment. Four operating rooms feed into this inner core.
Fry explains, “This is where we keep our sutures. If we need to flash sterilize something, like if the surgeons need something they’ve already used we can sterilize it in here. And we have our warmers, they warm instruments; we like to use warm instruments when possible.”
Fry nods to her right, “In there is our ortho room. We do a lot of total hip replacements, and over there is our old heart room, we use it for general surgery now.”
We walk back to the main hallway. I am shown a large bulletin board hung on the wall. “This is the surgical board, it lists the cases for today.” Fry points to a row of carts parked along the wall, each one loaded with instruments. “We take all the supplies and put them on those carts. Surgeons have their own preference card listing everything he likes to use. And every surgeon is different. It’s the art of a good circulating nurse to know the surgeon and know what he wants. Before a case starts, the nurse takes everything from here into the O.R., opens everything up, scrub nurses scrub every item, then set up all the instruments that will be used.”
We continue along the main corridor. Fry introduces me to Linda Karmon, scrub nurse. Karmon is over 40, has hazel eyes, dark hair. She’s maybe five-foot five. I lean against the wall and ask, “You’re the scrub nurse, what do you do during an operation?”
“I pass the instruments. The doctor says something and I give it to him, or, best of all possible worlds, I have anticipated his needs and there doesn’t have to be any talking. You can do that once you’ve done enough of the same kinds of cases with the same doctor. Each doctor has their likes and dislikes.”
“How many instruments do you handle?”
“It depends on the procedure, this is just a basic setup,” a steady hand points towards the nearest surgical cart. “That one is called a Minor set and there are Kellys, and a couple of retractors. This stuff is for a pretty simple procedure. Of course, we have clamps; you use them in a lot of surgeries because of bleeders. And you always have suctions, a Bovie, and electric pump.”
We walk into an empty operating room. On a wall shelf is an ancient Sony AM-FM radio playing soft rock. For the first time the surroundings seem familiar, like the neighborhood auto mechanic shop. We pass through, I ask, “What are the shift hours here?”
“The day shift is 6:30 a.m. to 3 o’clock. The p.m. shift is 2:30 until 11 o’clock, and we do not have a night shift.”
Linda takes me into the Cysto room. “This table is set up so that they can do X-ray procedures without moving the patient. The table tilts and all kind of things, costs a $100,000, and...” Linda moves both hands to the joint where the table top and stainless steel column meet the frame, and shakes. We hear a rattle from within that sounds like a steel baby-rattle, “...it’s not even six months old.”
I look into clear, hazel eyes and think, “Where to start this?” I cough, ask, “I hear a New York accent. How did you get to California?”
“Oh, my god. Took a vacation, liked it, stayed. Came to visit some friends, went to L.A. for a little while, but San Diego is much quieter.”
“Where did you get your degree?”
“I went to a tech school in Mississippi.”
I roll both eyes, laugh. “It was either Mississippi or Paris?”
“Yeah, they’re about the same. I got accepted in Mississippi.”
“Did you always want to be a nurse?”
“When I lived in Washington, I got a chance to see surgery and that was it. Once I saw it, I said, ‘Yes, this is for me.’ It’s very exciting, different every day.”
“What was it like the first time you saw a surgeon rip open a chest?”
“It was amazing. It didn’t bother me, because the patient is usually draped out, so you’re not seeing a face, you’re not seeing any body parts except that little section left uncovered. Contrary to popular belief, you do not bleed. An operation is not a bloody thing. They don’t want you to bleed. When you open up somebody, the blood isn’t there, it’s in veins and arteries. Doctors try very hard not to cut a vein or artery.”
“Is there a sound to it, when you cut open flesh?”
“The sound that you get in the O.R. is from an electric cautery machine. There’s definitely a smell. When I first started surgery it was clamp, clamp, cut, which means clamp, clamp both sides of a vein or an artery, cut it and tie. Now it’s this little pencil attached to a cautery machine that cuts and coagulates at the same time. It creates smoke, burning flesh is what it is.
“I did this in Manhattan ten years ago and it’s very different now. Nowadays it’s all lasers. Everything is video, which means it’s not only what your eyes can see, but if you’re working through a camera one drop of blood looks like, well, it looks big.”
“How long have you been a scrub nurse?”
“I took a five-year hiatus to run a motel,” she laughs. “Many lives. Altogether, I’ve been in nursing 14 years.”
“What is the difference between a real operation and what you see on TV?”
“If I look at a show I can see that maybe the tube isn’t placed right, or the bleeding isn’t right, it’s more dramatic on television, but not that much more. In real life it’s very controlled, there’s no wasted steps. Hardly anybody ever dies in the operating room. They get you out of here and you die somewhere else.”
“How has the operating room changed since AIDS?”
“There’s a thing called 'universal precaution’ now. They did not have that before AIDS. Now, every case we have is considered a contaminated case, which requires a different procedure. I have dealt with a lot of friends who have died of AIDS; I know how it can be frightening to some people. It’s not frightening to me. If the sharp instruments are dealt with in the proper manner, you won’t get hurt. I’m not going to catch AIDS by touching somebody.”
“What’s the most dangerous moment in surgery?”
“I think intubation for anesthesia. Intubation is when a patient’s going under anesthesia and the tube has to go in. That’s not my part of it.”
“What’s your day like?”
“Well, we have to be here at 6:30 a.m., and start surgery at 7:30. When we walk into work, there’s a board on the wall that lists the surgeries, and then you know where you are going to be. You’re usually in that room for the whole day unless everything is changed around, or something is canceled. We get off at 3 o’clock. Today is a very mellow day; some days, it’s just one operation after the other.
“Anyway, they roll the patients in. Whoever’s scrubbing the case is already in the operating room, making a sterile field, setting up the instruments. A nurse is helping with the patient and helping the anesthesiologist. The doctors are inside scrubbing their hands; I’ve already done that a long time ago. The doctors come in, we gown them so they become sterile. Then they drape out the patient with sterile towels and a sterile sheet, so the only thing that’s open is this little spot on the body that’s going to be operated on, which has already been prepped by the nurse. Then the case starts.”
“How many instruments do you have to remember?”
“There’s a huge amount, but a lot of instruments are the same, just different sizes. They’re little ones because it’s the beginning of the operation, or they’re longer because the doctors are going in deeper, but it’s the same type of instrument, just a little longer. OB-GYN has their own instruments, as does Ortho, General, Neural, and so on.”
“Do you scrub all the surgeries?”
“I don’t do hearts, they have a heart team. I haven’t done total joints because there’s a team there, too.”
“Are those the glamour positions?”
“Heart is a glamour position. Orthopedic, yeah, I guess that is too. Ortho’s a lot of work, a lot of heavy instruments — they are heavy, heavy.”
“What’s it like when you put your hand inside an opened body?”
“It’s warm and wet, there is a wetness. We’re 90 percent seawater, or something like that, so inside, everything is smooth next to each other, there’s nothing rough.”
We walk out into the corridor, meander into the instrument cleaning room. Karmon stands over a tray of worn but immaculately clean operating instruments. “Now this is a weighted specula that goes into the vagina.”
I look at a gigantic stainless steel thing; it looks like a mutated shoe horn. “Good God.”
“Yeah, it looks like ancient stuff. These are more modern looking.” Linda picks up a delicate instrument. “This is a forcep, like a jeweler would have forceps.”
“This stuff must cost a fortune.”
“I think each one of these costs $25. Now this,” quick hands pick up a large, ugly, steel object, “is called Connor-O’Sullivan, which is a retractor you put in a stomach, and then you open up the stomach, and then the doctor works in there. You can be opened up this far...” Karmon opens the retractor; the thing becomes an enormous gaping hole like the jaws of a white shark.
“Auuuugh.”
She laughs. “Actually, it goes very easy. For a layperson it’s weird. This is a small retractor, they have much bigger ones.”
I turn away, mumble. “Being a nurse for 14 years, is it like going to work now?”
“Yes, yes. It is going to work. Interesting though. Yesterday they took out a kidney. I hadn’t touched a kidney in years, you get taken aback when they hand you a kidney. Same thing with an amputation. A leg has a very different feeling when it’s not connected to you, when they just hand it over to you. It’s a very weird feeling.” “What do you do with it?” “It’s covered, first of all. It’s handed to me, then I hand it to the nurse, or put it in another bag, and it’s tagged. Any body part or piece that comes out of the patient goes to the lab. And for a leg or things like that, there might be a religious reason, it might have to be buried, depends on what the person decides.”
“Do they have a storage facility for legs and arms?”
“No.”
“What was the first body part you saw?”
“When I first started as an aide, as a kid, I got to go through OB. And they used to save placentas. And they put them in an icebox — placentas — because they made an antibiotic from them. So, I was a kid, I saw my first delivery, and I couldn’t stop crying, it was just amazing, and then I started fooling around, looking around, opened a freezer — like an ice cream freezer in those days — and there was these placentas.”
“Auuugh!”
Comments