 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube
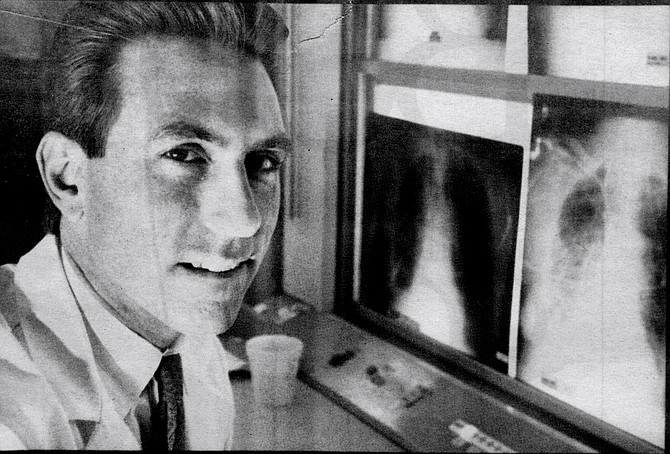
Doctor Michael Koumjian looks younger than his 37 years. If you were making a movie about him, you might cast Kevin Costner; he has that sensitive, pleasant, and boyish handsomeness. In fact, he looks more like an actor or an athlete than a cardiac and thoracic surgeon. At a dinner party in November of 1989, Koumjian spoke quietly about his work to a table of fashion designers, sports car dealers, models, novelists, and scientists. Of all the people in the room, none of whom might be described as having boring jobs, the source of interest was Koumjian. What do you do? What is it like? How do you feel when you're... doing it?
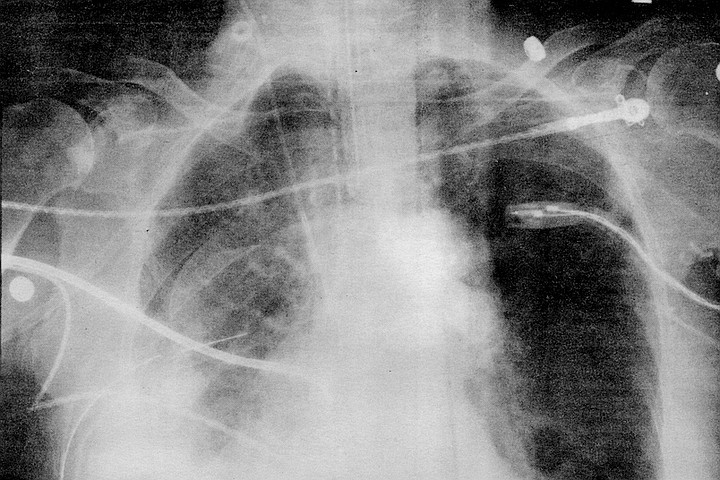
Koumjian is not talkative. His words are measured and thoughtful. The stereotype of the swaggering physician playing God with brassy confidence is immediately conspicuous by its absence in this retiring figure with the slightly mischievous smile. "If it's a new procedure. I'm thinking pretty much about the procedure. If it's routine, I might think about...." But what he might think about is left to speculation as his beeper sounds and he excuses himself for the third time during the meal. He speaks in hushed tones into the telephone, and the partygoers try to be inconspicuous about their eavesdropping as they make dinner conversation. Something about the raw drama of heart surgery has captured the group. The fine points of importing Maseratis, Donna Karan's spring line, the death or rebirth of the novel, even AIDS research all pale in interest, usurped by the image of this thoughtful man sewing and stitching a human heart like a garment.
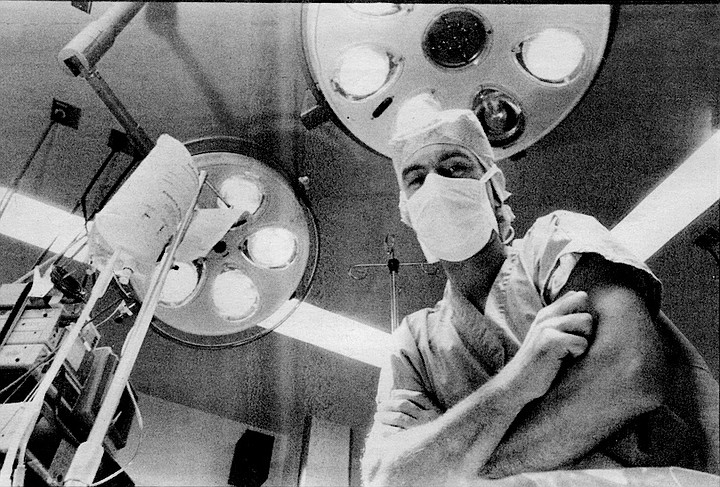
"Sorry, sorry." He returns to the table and slices his cooling pizza, pours himself a glass of red wine. "You wanted to know about the HIV-positive patient. Well, he was brought in for aortic valve endocarditis but was routinely tested, and it turns out he was positive. No one was eager to perform surgery. I said I'd do it. I used a new kind of glove, like chain mail sort of. It's impervious to needles, supposedly, and scalpels, but there's no guarantee." He smiles, chewing his pizza, washing it down with Chianti. "Trouble is, it's more difficult to manipulate instruments." He plays his fork in the air, describing tiny arcs over the mozzarella, black olives, and tomato sauce.
"Oh God, Michael!" His cousin makes a face and laughs, but her interest is piqued. She does, really, want him to go on. Someone lights a cigarette and says, "Okay. I know, I know. You're going to tell me why I shouldn't smoke. In great detail."
"I probably should." Michael grins, forking salad between his even, white teeth. He describes what-the lung looks like while exposed in surgery. He goes on smiling and presents the facts. He talks about the coloration of the lung, the function and texture of cilia. The smoker draws with less relish on his Merit and puts it out on his pizza crust.
"Oh, Bob," his wife admonishes. "You've got to quit."
Michael smiles away, eating heartily. It is not what Koumjian says, but his presence, what he does, that informs the room with reverence, fear, a kind of fascination/repulsion: a healer who might save us when it's pulse to the wall.
"I'm sick of the Chargers," someone says.
Michael laughs. "Tell me about it."
The subject is changed. Everyone thinks, I would like to know what he does. The drama in the minutiae of this man's life promises much. The wine flows.
Koumjian is a busy man. When he makes rounds it is sometimes to five patients in five different hospitals around the county. Another factor was Koumjian's reluctance to be portrayed as a Porsche-driving, life-in-the-fast-lane surgeon, a playboy with a neo-deco bachelor pad at Windansea. Worse yet, a saint. He was momentarily amused but finally resistant to any media attention whatsoever. In July of the following year, I received a phone call from a man named Raylan Evans. He was calling from a trailer park in San Ysidro.
"I have read your articles." He spoke with a trace of Southern accent. "And you should know that God has worked a miracle through the skill and compassion of a doctor here in San Diego. You should write about this man, who is a very powerful tool in the hands of the Lord."
The circumstances involved a 43-year-old man, the son of Raylan and Beverly Evans, who is congenitally afflicted with several handicaps including cerebral palsy. Charles has the mental agility of a two-year-old and the social capacity of a first grader. He is legally blind. He is also deaf. He had a stroke at 19. "Charles is physically deformed to some extent as well. He's a chromosome case. We'd like very much for you to see him," Raylan said.
A retired real estate man from Colorado Springs, Evans came to San Diego as a cancer patient in remission seeking Laetrile and enzyme treatments in Tijuana in 1983. He and his wife Beverly returned for the climate and moved to Coronado. "Another of Wayne's [Charles's nickname] congenital weaknesses is his esophagus. Fifteen or sixteen times in his life we've had to have food removed. A physician had stretched his esophagus, and Wayne was able to swallow normally for a time, but shortly thereafter, while he was eating supper one night — this was June of 1989 — he showed great distress and he ruptured his esophagus. He was in great pain. He almost went into shock. Of course, he was unable to tell us anything, but we're accustomed to him so we were able to tell what it was. The lower portion of his esophagus is abnormally small and it just ruptured. For years we pureed his food like baby food. Anyway, we took him to Coronado hospital and he was diagnosed quickly, but they were unable to do anything there.
"We needed a surgeon, so the doctor called Mercy. The emergency room physician said he would call Dr. Koumjian...."
"Did you say Koumjian?"
"Yes, Michael Koumjian. This was about seven o'clock on a Saturday night...."
Asking Evans for directions to his trailer park, I told him I would like to see his son and hear about the case. Evans complied, and within the hour I was sitting on a director's chair beneath an awning that extended from their RV. Evans appeared to be in his 60s, his wife somewhat younger. He is a slow-speaking man with a kindly manner. His wife is quiet but energetic and attentive. She contributed readily.
"We had been told from the word go, at Coronado, just how dangerous it was. The contamination, going into such a sterile area ... we were told there was a 95 to 99 percent chance of death. He was put on oxygen, an IV, and heart monitor in the ambulance. He was given barium for the X-rays, but we waited at Mercy for 2 1/2 hours in the emergency room. The diagnostic tests appeared normal. But he was in such obvious distress that the nurse immediately called Dr. Koumjian, who was in surgery at the time. Koumjian called in another surgeon to close for him so that he could leave and come see Wayne.
"By that time, it had been 12 hours and Dr. Koumjian ordered another barium swallow and sent him down to surgery. Mike worked on him for 8 1/2 hours."
Beverly interjected, "The thing that makes it all the more a miracle is that mediastinitis had set in, an infection under the sternum, the very worst place. He had seven different kinds of bacteria in there. Ten doctors told us he would not live, that no one could live with what he had. Not Dr. Koumjian."
"We wanted to tell somebody," Raylan picked up, "how he differs from the other doctors. He seems to be under such a shadow of other, older physicians. He seems to get the dregs of cases, but that's all right with him. He just serves mankind. His skill is such that.... Well, the nurses recognize it."
Beverly added, "Wayne survived that surgery, and nine weeks later he had to undergo another 12-hour surgery, which Mike did. In those nine weeks, scar tissue had grown horribly, plus, where they gave him the barium, it had solidified in the lung. Dr. Koumjian could not have removed it the first time. So this second time around, Koumjian had to deal with this wall of cement. Dr. Koumjian took as much of that off as he could, just scraping it away. It required the removal of part of a lung, some ribs, just to get to it. Mike disengaged Wayne's stomach and reattached it to the stub of the esophagus where he had taken out the deformed part. He reattached his stomach up here." Beverly reached around her right armpit and indicated a spot just beneath her right shoulder blade. "Twelve and a half hours."
"Wayne's lifestyle now is far less than it was prior to this," Raylan said. "But that he is alive at all is a miracle."
"Something has come about with him,” Beverly continued. "He's becoming more sociable, he's gaining strength."
At this point I was taken into the RV and introduced to Wayne. He was lying in bed and blinking sleepily from beneath an abnormally large brow. Uneager to be roused from his bed, though it was past noon, Wayne made noises of protestation from deep in his throat. Beverly sat him up and began lifting his T-shirt to expose the scars from surgery.
The scar behind Wayne's right shoulder blade was something like a trench. Deeply concave, running laterally about eight inches and three or four inches wide, it was a new deformity that Wayne would have to live with. Wayne, who looked like a child's grotesque rendering of a man, furrowed his brow and began to strike himself in the face with his hand. This appeared to be a well-rehearsed ploy to annoy his mother, who hurriedly lowered his arm and shushed him.
He continued to frown and wrinkle his nose in annoyance. It was impossible to imagine what Wayne's life might have been like, what it will continue to be. Thinking of Koumjian's massive efforts to save this man, the question why? presented itself, and on the heels of that thought came a wave of disappointment in myself that the answer was not, somehow, obvious.
Koumjian, in tennis clothes, sat in his home in La Jolla overlooking the beach, leaned forward, and drank from a can of Coors Light. His apartment is dominated by black furniture, stereo, and a wide-screen television. Above the black leather couches is a colorful abstract painting shot with bright red and gold leaf paint. "Boerhaaves Syndrome. Ruptured esophagus," he said. "It's named after some Dutch surgeon who had some old general for a patient who was eating duck. The guy tried to swallow the whole duck or something, and he ruptured his esophagus. It's a well-documented syndrome."
Koumjian grew up in Freehold, New Jersey, and finished medical school in 1977 when he was 23. He did a year of internship at Balboa Hospital and then a year on board ship with the Navy. This was followed by five years of general surgery and two years of cardiac training at UCSD and Sharp Hospital. He was a cardiac surgeon with the Navy from 1985 to 1988. He remains in the Naval Reserve and is on call, as of this writing, for the Middle East.
"In a war, they need a lot of chest surgeons," he explained. "In modern warfare, something like 40 percent of all injuries are in the chest. The high-velocity weapons they use nowadays...." He drank his beer. "In 1987, the Navy sent me to Portland, Oregon, to train under Dr. Starr, who did the first heart valves ever in 1960. It was a six-month scholarship in complex valve surgery and heart transplants. Then I went to Italy for three more months of transplant surgery."
"Did you always want to be a surgeon?"
"My dad kind of programmed me, like a robot. My dad is Armenian and he was born in Turkey. When he came here he decided he wanted all of his kids to be professionals. He bought me a stethoscope when I was like four years old. He pushed it. When I was in high school and college, it really seemed like an interesting thing to do. I had a brother who was in preventive medicine, a doctor. He went into public health service in the most medically indigent population of the country, which was in northwestern Mississippi. One night after being awake for a long time, having delivered a baby, he was driving home, came around a curve, and this tractor hit him. He was killed at 29 years of age. It affected me a lot. He came in brain dead, but his heart was still alive. He was in a trauma center in Memphis. I could see that his intracranial pressure was higher than his blood pressure. No blood flowing through his brain. They were reluctant to say that he was brain dead, because I was a doctor."
"Is there a gray area between being alive and dead?"
"No," he answered quickly. "Sometimes to the patient's family, because they'll look up and see he's got a blood pressure of 120, which is totally normal. They might touch him and see a peripheral reflex of his leg and think, 'Geez. he's still moving.' But there's no blood flowing to his brain, so the chance of his being a viable human being is zero.”
Koumjian excused himself to answer his beeper and returned with another beer for himself and his guest. Out the window, surfers caught waves in the sunset. On the beach, a group of teenagers on the seawall laughed at a homeless man shambling along the sand without his pants on.
"You don't really fit the image of a typical heart surgeon," I pointed out. "You know, the obnoxious, egotistical guy with a loud voice barking at people."
He nodded and grinned as if he'd heard this before. "It's true. The guys that are like that don't really have insight into what they're doing. They end up yelling at all the nurses and making everybody upset. I've just taken a tack that tries to avoid that. The reason it happens to cardiac surgeons is because when things occasionally go bad, and there's always problems in surgery — you're dealing with life and death every day — you're the one who is ultimately responsible. You've got an anesthesiologist, a handful of techs and nurses running around, someone running the bypass machine; you're like the captain of the ship.
If something goes wrong, it ends up being your fault. Rather than let those pressures become externalized and making everybody nervous, I get better results internalizing them, using calm words, staying cool and trying to maintain."
"Why the heart? Why not brain surgery or oncology?"
"Because it is the most technically demanding. Every case has the potential of becoming a very difficult case of life and death. I thought it would be challenging and never become routine or mundane."
"And is it ever routine?"
"No. Even when everything goes well, you still have to maintain a level of proficiency that is technically demanding, and you're always on edge because you know things could change very rapidly. It's kind of like flying an F14 or something. Most of the flying is routine, but you know that if the slightest thing happens to your jet, things could change rapidly."
"It’s a very good, quote unquote, natural high," Koumjian continued. "For example, when things go well in a case where a patient has a very low chance of surviving. That's unusual in that most cases have a high rate of predictability. Most cardiac cases have a 98 percent chance of doing well nowadays.
"But I just had a case, a 29-year-old Hispanic male that has four kids, he's an IV heroin user. From the IV use he infected his aortic valve, and he got what is called endocarditis. It got so bad the infection actually burrowed a hole through his heart. He came in in very bad congestive failure, and because of that the blood backed up, and his liver wasn't working very well. He had no insurance, of course, so it became an ethical thing. It's a very expensive procedure, to put a valve in. We had the resources to do it, and it would involve a long hospital stay, which is costly. Now, if he shoots up again he's going to immediately infect that valve, which is metal and carries an even higher risk of infection. But Mercy decided to go ahead and do it, and they asked me if I'd accept the case and I said fine, but the anesthesiologist who was put on the case called me that night and said, 'Look, this guy's got a 90 percent chance of dying. Why are you willing to take this case? Even if he gets over the initial surgery, he's gonna bleed out. He's an addict and he'll just do it again. There's no chance for this guy.'
"I said, the guy has four kids and he's seeing a psychiatrist. It seemed he was a good candidate for rehab. As it turned out, the hole in his heart went right through the conducting nerves that stimulate the heartbeat, so we had to put in a pacemaker. Now he's still in the hospital, he needs six weeks of antibiotics. He'll be discharged on Thanksgiving. He says his life has changed, that he won't shoot up anymore. I don't know.” Koumjian shrugs. "You can ask him yourself."
Koumjian invited me to sit in on two surgeries and to join him on rounds the next day. The Hispanic patient he described looked emaciated. He had long hair and a wispy black beard. His arms and torso were decorated with amateur tattoos. The man, who spoke little English, displayed his scars to me and invited me to touch the hard patch of healing skin that concealed the pacemaker.
As Dr. Koumjian asked him how he felt, the man replied "feeling stronger," as he looked at the surgeon with what can only be described as an expression of enormous gratitude, almost adoration.
"You know that if you shoot drugs again you will probably die?" Koumjian asked him.
The patient nodded. He understood. “No mas,” he said. “No mas.”
Koumjian entered a dark, closet-like room and beckoned for me to follow. "Let me show you something," he said. He held a spool of film in his hand and then placed it in a cradle on a screening device that looked something like an editing machine. "This morning I'll be doing a triple bypass on a 72-year-old male. Maybe a quadruple bypass, I don't know yet. This is film of his heart." He switched on the screen, and a black-and-white film of dye moving through arteries and vessels writhed like smoke in a strobe light. He pointed out "blockages," which looked similar to the other patches of grey and white on the screen. In the darkened room, he silently studied the film, moving it back and forth in its cradle to replay the same sequence of dye being pumped through the chambers and tangles of vessels and ventricles. "Okay," he said after a time. "Let's go."
In the doctor's locker room we stripped and changed into hospital greens, shoe coverings, paper hats that tied beneath the chin, and masks. Koumjian scrubbed but told me I didn't need to unless I'd be operating. I wasn't to bring in a tape recorder, so I assumed this meant no notebook either. I followed him into O.R. #8, a brightly lit room the size of my apartment bedroom. Green-suited figures moved neither slowly nor hurriedly among the monitors, instruments, racks of sponges, and the heart and lung machine. It was impossible to tell who was a doctor, a tech, a nurse, the anesthesiologist. The coldness of the room struck me immediately. The temperature had been lowered for reasons having to do with protecting the heart. I was offered a shawl by one of the nurses but declined.
The patient's bald head was visible beneath a tangle of tubing monitored by Dr. John Ahlering, the anesthesiologist. He would be answering most of my questions in a quiet voice during the procedure. I was told to stand a few inches from the top of the patient's head. I did so and looked down at the jaundice-colored, Betadine-washed skin exposed in a square between navel and collarbone. Clinging to the skin was a plastic adhesive.
Another surgeon was already working on the patient's left leg. Dr. Gomez-Engler was introduced to me. He was busy opening the calf to remove the saphenous vein, which in turn would be grafted to replace the obstructed veins on the surface of the man's heart.
Without ceremony or fanfare, Koumjian used an electrical scalpel to make the incision in the center of the sternum. A radio in the O.R. was playing Wes Montgomery-style jazz guitar. The scalpel cauterized the tissue it cut, exposing yellow fat globules and quickly clotted blood. The smell of burnt meat and ozone in the room made me momentarily nauseated. Turning away, I asked John Ahlering what the patient would be feeling, if anything.
He told me that the man was given something like curare to paralyze him, something like morphine or heroin to deaden the pain, and a third drug in the Diazepam family to induce amnesia. "We want him absolutely still and not experiencing pain, but we don't want him to remember the experience either."
With the sternum exposed, Koumjian leaned over the patient with a fiber-optical loop fixed around his head. A small beam of concentrated light was attached to the headgear, like a penlight. A pair of Coke-bottle magnifying lenses distorted Koumjian's eyes into those of some subaquatic creature. The saw he wielded to open the bone joining the ribs looked like a butcher's saw.
"What is that thing?" I asked the anesthesiologist.
"It's a meat saw, basically."
The smell of burnt, cleaved calcium permeated the room, and again I turned to monitors and machinery to ask questions.
"This is the part that gets to people," said Ahlering. "Here, this is a pulse oximeter. It measures the oxygen in the blood. Have you met Ramey Stewart?"
I turned to meet the "perfusionist," a masked woman with large blue eyes behind wire-rimmed glasses. She would be in charge of the heart and lung machine. The patient's life would, in effect, be entrusted to her and several yards of tubing and pumps and thermometers and gauges while Koumjian cut and threaded veins in the man's heart.
"You okay?" she asked. The Moody Blues were on the radio, and they kept using the word heart in the song. "Fine. Fine. Thank you."
Ahlering started drawing me a diagram of the atrium, the ventricle, the aorta, and the lungs, pointing out the location of the mammary artery, which they would need access to in order to take a piece of it and graft it elsewhere. Stewart talked about the measurement of anti-coagulation, the necessity for the coldness of the room. "Activated clotting time...." she was saying. Ahlering was pointing out a monitor, "...wave form of exhaled CO2... tidal volume ... arterial pulse ... mixed venous oxygen ... pulmonary artery catheter...."
They were trying to distract me from the fact that Koumjian had now installed a rack of metal onto the patient's chest and was separating his rib cage with the thing by cranking a lever. The left side of the sternum was now elevated in a manner not unlike jacking up a car chassis.
"Sternum retractor," John said. "You okay?" I nodded. I had seen the inside of a human torso on cable TV, but this was very different. I was inches from the egg-like white tissue, the pericardium surrounding the heart that writhed and subsided rhythmically. As the rib cage was lifted, cranked, pulled farther away, I thought about the pain this man would feel in his back for days. Reading my mind, Koumjian turned to me and said, "What he'll feel afterward is a discomfort along his spine because of the retractor."
What I was feeling was a sudden lightheadedness, and Dr. Gomez-Engler suggested I sit down and place my head between my knees. I did this while Ramey Stewart distracted me with a running commentary on the intricacies of the perfusion device.
The next day, I made rounds with Koumjian and met the patient. He was sitting in a chair, not in bed, and seemed in good spirits. He was in no obvious pain, though catheters and IV tubing trailed from his body. Koumjian told him how well it had gone, and the man nodded, pleased. Twenty-four hours ago he had been all but technically dead — his heart still, his blood routed through yards of cool tubing, his chest open — with Michael Koumjian holding the 800 grams of heart in his hand like a trembling animal.


Doctor Michael Koumjian looks younger than his 37 years. If you were making a movie about him, you might cast Kevin Costner; he has that sensitive, pleasant, and boyish handsomeness. In fact, he looks more like an actor or an athlete than a cardiac and thoracic surgeon. At a dinner party in November of 1989, Koumjian spoke quietly about his work to a table of fashion designers, sports car dealers, models, novelists, and scientists. Of all the people in the room, none of whom might be described as having boring jobs, the source of interest was Koumjian. What do you do? What is it like? How do you feel when you're... doing it?

Koumjian is not talkative. His words are measured and thoughtful. The stereotype of the swaggering physician playing God with brassy confidence is immediately conspicuous by its absence in this retiring figure with the slightly mischievous smile. "If it's a new procedure. I'm thinking pretty much about the procedure. If it's routine, I might think about...." But what he might think about is left to speculation as his beeper sounds and he excuses himself for the third time during the meal. He speaks in hushed tones into the telephone, and the partygoers try to be inconspicuous about their eavesdropping as they make dinner conversation. Something about the raw drama of heart surgery has captured the group. The fine points of importing Maseratis, Donna Karan's spring line, the death or rebirth of the novel, even AIDS research all pale in interest, usurped by the image of this thoughtful man sewing and stitching a human heart like a garment.

"Sorry, sorry." He returns to the table and slices his cooling pizza, pours himself a glass of red wine. "You wanted to know about the HIV-positive patient. Well, he was brought in for aortic valve endocarditis but was routinely tested, and it turns out he was positive. No one was eager to perform surgery. I said I'd do it. I used a new kind of glove, like chain mail sort of. It's impervious to needles, supposedly, and scalpels, but there's no guarantee." He smiles, chewing his pizza, washing it down with Chianti. "Trouble is, it's more difficult to manipulate instruments." He plays his fork in the air, describing tiny arcs over the mozzarella, black olives, and tomato sauce.
"Oh God, Michael!" His cousin makes a face and laughs, but her interest is piqued. She does, really, want him to go on. Someone lights a cigarette and says, "Okay. I know, I know. You're going to tell me why I shouldn't smoke. In great detail."
"I probably should." Michael grins, forking salad between his even, white teeth. He describes what-the lung looks like while exposed in surgery. He goes on smiling and presents the facts. He talks about the coloration of the lung, the function and texture of cilia. The smoker draws with less relish on his Merit and puts it out on his pizza crust.
"Oh, Bob," his wife admonishes. "You've got to quit."
Michael smiles away, eating heartily. It is not what Koumjian says, but his presence, what he does, that informs the room with reverence, fear, a kind of fascination/repulsion: a healer who might save us when it's pulse to the wall.
"I'm sick of the Chargers," someone says.
Michael laughs. "Tell me about it."
The subject is changed. Everyone thinks, I would like to know what he does. The drama in the minutiae of this man's life promises much. The wine flows.
Koumjian is a busy man. When he makes rounds it is sometimes to five patients in five different hospitals around the county. Another factor was Koumjian's reluctance to be portrayed as a Porsche-driving, life-in-the-fast-lane surgeon, a playboy with a neo-deco bachelor pad at Windansea. Worse yet, a saint. He was momentarily amused but finally resistant to any media attention whatsoever. In July of the following year, I received a phone call from a man named Raylan Evans. He was calling from a trailer park in San Ysidro.
"I have read your articles." He spoke with a trace of Southern accent. "And you should know that God has worked a miracle through the skill and compassion of a doctor here in San Diego. You should write about this man, who is a very powerful tool in the hands of the Lord."
The circumstances involved a 43-year-old man, the son of Raylan and Beverly Evans, who is congenitally afflicted with several handicaps including cerebral palsy. Charles has the mental agility of a two-year-old and the social capacity of a first grader. He is legally blind. He is also deaf. He had a stroke at 19. "Charles is physically deformed to some extent as well. He's a chromosome case. We'd like very much for you to see him," Raylan said.
A retired real estate man from Colorado Springs, Evans came to San Diego as a cancer patient in remission seeking Laetrile and enzyme treatments in Tijuana in 1983. He and his wife Beverly returned for the climate and moved to Coronado. "Another of Wayne's [Charles's nickname] congenital weaknesses is his esophagus. Fifteen or sixteen times in his life we've had to have food removed. A physician had stretched his esophagus, and Wayne was able to swallow normally for a time, but shortly thereafter, while he was eating supper one night — this was June of 1989 — he showed great distress and he ruptured his esophagus. He was in great pain. He almost went into shock. Of course, he was unable to tell us anything, but we're accustomed to him so we were able to tell what it was. The lower portion of his esophagus is abnormally small and it just ruptured. For years we pureed his food like baby food. Anyway, we took him to Coronado hospital and he was diagnosed quickly, but they were unable to do anything there.
"We needed a surgeon, so the doctor called Mercy. The emergency room physician said he would call Dr. Koumjian...."
"Did you say Koumjian?"
"Yes, Michael Koumjian. This was about seven o'clock on a Saturday night...."
Asking Evans for directions to his trailer park, I told him I would like to see his son and hear about the case. Evans complied, and within the hour I was sitting on a director's chair beneath an awning that extended from their RV. Evans appeared to be in his 60s, his wife somewhat younger. He is a slow-speaking man with a kindly manner. His wife is quiet but energetic and attentive. She contributed readily.
"We had been told from the word go, at Coronado, just how dangerous it was. The contamination, going into such a sterile area ... we were told there was a 95 to 99 percent chance of death. He was put on oxygen, an IV, and heart monitor in the ambulance. He was given barium for the X-rays, but we waited at Mercy for 2 1/2 hours in the emergency room. The diagnostic tests appeared normal. But he was in such obvious distress that the nurse immediately called Dr. Koumjian, who was in surgery at the time. Koumjian called in another surgeon to close for him so that he could leave and come see Wayne.
"By that time, it had been 12 hours and Dr. Koumjian ordered another barium swallow and sent him down to surgery. Mike worked on him for 8 1/2 hours."
Beverly interjected, "The thing that makes it all the more a miracle is that mediastinitis had set in, an infection under the sternum, the very worst place. He had seven different kinds of bacteria in there. Ten doctors told us he would not live, that no one could live with what he had. Not Dr. Koumjian."
"We wanted to tell somebody," Raylan picked up, "how he differs from the other doctors. He seems to be under such a shadow of other, older physicians. He seems to get the dregs of cases, but that's all right with him. He just serves mankind. His skill is such that.... Well, the nurses recognize it."
Beverly added, "Wayne survived that surgery, and nine weeks later he had to undergo another 12-hour surgery, which Mike did. In those nine weeks, scar tissue had grown horribly, plus, where they gave him the barium, it had solidified in the lung. Dr. Koumjian could not have removed it the first time. So this second time around, Koumjian had to deal with this wall of cement. Dr. Koumjian took as much of that off as he could, just scraping it away. It required the removal of part of a lung, some ribs, just to get to it. Mike disengaged Wayne's stomach and reattached it to the stub of the esophagus where he had taken out the deformed part. He reattached his stomach up here." Beverly reached around her right armpit and indicated a spot just beneath her right shoulder blade. "Twelve and a half hours."
"Wayne's lifestyle now is far less than it was prior to this," Raylan said. "But that he is alive at all is a miracle."
"Something has come about with him,” Beverly continued. "He's becoming more sociable, he's gaining strength."
At this point I was taken into the RV and introduced to Wayne. He was lying in bed and blinking sleepily from beneath an abnormally large brow. Uneager to be roused from his bed, though it was past noon, Wayne made noises of protestation from deep in his throat. Beverly sat him up and began lifting his T-shirt to expose the scars from surgery.
The scar behind Wayne's right shoulder blade was something like a trench. Deeply concave, running laterally about eight inches and three or four inches wide, it was a new deformity that Wayne would have to live with. Wayne, who looked like a child's grotesque rendering of a man, furrowed his brow and began to strike himself in the face with his hand. This appeared to be a well-rehearsed ploy to annoy his mother, who hurriedly lowered his arm and shushed him.
He continued to frown and wrinkle his nose in annoyance. It was impossible to imagine what Wayne's life might have been like, what it will continue to be. Thinking of Koumjian's massive efforts to save this man, the question why? presented itself, and on the heels of that thought came a wave of disappointment in myself that the answer was not, somehow, obvious.
Koumjian, in tennis clothes, sat in his home in La Jolla overlooking the beach, leaned forward, and drank from a can of Coors Light. His apartment is dominated by black furniture, stereo, and a wide-screen television. Above the black leather couches is a colorful abstract painting shot with bright red and gold leaf paint. "Boerhaaves Syndrome. Ruptured esophagus," he said. "It's named after some Dutch surgeon who had some old general for a patient who was eating duck. The guy tried to swallow the whole duck or something, and he ruptured his esophagus. It's a well-documented syndrome."
Koumjian grew up in Freehold, New Jersey, and finished medical school in 1977 when he was 23. He did a year of internship at Balboa Hospital and then a year on board ship with the Navy. This was followed by five years of general surgery and two years of cardiac training at UCSD and Sharp Hospital. He was a cardiac surgeon with the Navy from 1985 to 1988. He remains in the Naval Reserve and is on call, as of this writing, for the Middle East.
"In a war, they need a lot of chest surgeons," he explained. "In modern warfare, something like 40 percent of all injuries are in the chest. The high-velocity weapons they use nowadays...." He drank his beer. "In 1987, the Navy sent me to Portland, Oregon, to train under Dr. Starr, who did the first heart valves ever in 1960. It was a six-month scholarship in complex valve surgery and heart transplants. Then I went to Italy for three more months of transplant surgery."
"Did you always want to be a surgeon?"
"My dad kind of programmed me, like a robot. My dad is Armenian and he was born in Turkey. When he came here he decided he wanted all of his kids to be professionals. He bought me a stethoscope when I was like four years old. He pushed it. When I was in high school and college, it really seemed like an interesting thing to do. I had a brother who was in preventive medicine, a doctor. He went into public health service in the most medically indigent population of the country, which was in northwestern Mississippi. One night after being awake for a long time, having delivered a baby, he was driving home, came around a curve, and this tractor hit him. He was killed at 29 years of age. It affected me a lot. He came in brain dead, but his heart was still alive. He was in a trauma center in Memphis. I could see that his intracranial pressure was higher than his blood pressure. No blood flowing through his brain. They were reluctant to say that he was brain dead, because I was a doctor."
"Is there a gray area between being alive and dead?"
"No," he answered quickly. "Sometimes to the patient's family, because they'll look up and see he's got a blood pressure of 120, which is totally normal. They might touch him and see a peripheral reflex of his leg and think, 'Geez. he's still moving.' But there's no blood flowing to his brain, so the chance of his being a viable human being is zero.”
Koumjian excused himself to answer his beeper and returned with another beer for himself and his guest. Out the window, surfers caught waves in the sunset. On the beach, a group of teenagers on the seawall laughed at a homeless man shambling along the sand without his pants on.
"You don't really fit the image of a typical heart surgeon," I pointed out. "You know, the obnoxious, egotistical guy with a loud voice barking at people."
He nodded and grinned as if he'd heard this before. "It's true. The guys that are like that don't really have insight into what they're doing. They end up yelling at all the nurses and making everybody upset. I've just taken a tack that tries to avoid that. The reason it happens to cardiac surgeons is because when things occasionally go bad, and there's always problems in surgery — you're dealing with life and death every day — you're the one who is ultimately responsible. You've got an anesthesiologist, a handful of techs and nurses running around, someone running the bypass machine; you're like the captain of the ship.
If something goes wrong, it ends up being your fault. Rather than let those pressures become externalized and making everybody nervous, I get better results internalizing them, using calm words, staying cool and trying to maintain."
"Why the heart? Why not brain surgery or oncology?"
"Because it is the most technically demanding. Every case has the potential of becoming a very difficult case of life and death. I thought it would be challenging and never become routine or mundane."
"And is it ever routine?"
"No. Even when everything goes well, you still have to maintain a level of proficiency that is technically demanding, and you're always on edge because you know things could change very rapidly. It's kind of like flying an F14 or something. Most of the flying is routine, but you know that if the slightest thing happens to your jet, things could change rapidly."
"It’s a very good, quote unquote, natural high," Koumjian continued. "For example, when things go well in a case where a patient has a very low chance of surviving. That's unusual in that most cases have a high rate of predictability. Most cardiac cases have a 98 percent chance of doing well nowadays.
"But I just had a case, a 29-year-old Hispanic male that has four kids, he's an IV heroin user. From the IV use he infected his aortic valve, and he got what is called endocarditis. It got so bad the infection actually burrowed a hole through his heart. He came in in very bad congestive failure, and because of that the blood backed up, and his liver wasn't working very well. He had no insurance, of course, so it became an ethical thing. It's a very expensive procedure, to put a valve in. We had the resources to do it, and it would involve a long hospital stay, which is costly. Now, if he shoots up again he's going to immediately infect that valve, which is metal and carries an even higher risk of infection. But Mercy decided to go ahead and do it, and they asked me if I'd accept the case and I said fine, but the anesthesiologist who was put on the case called me that night and said, 'Look, this guy's got a 90 percent chance of dying. Why are you willing to take this case? Even if he gets over the initial surgery, he's gonna bleed out. He's an addict and he'll just do it again. There's no chance for this guy.'
"I said, the guy has four kids and he's seeing a psychiatrist. It seemed he was a good candidate for rehab. As it turned out, the hole in his heart went right through the conducting nerves that stimulate the heartbeat, so we had to put in a pacemaker. Now he's still in the hospital, he needs six weeks of antibiotics. He'll be discharged on Thanksgiving. He says his life has changed, that he won't shoot up anymore. I don't know.” Koumjian shrugs. "You can ask him yourself."
Koumjian invited me to sit in on two surgeries and to join him on rounds the next day. The Hispanic patient he described looked emaciated. He had long hair and a wispy black beard. His arms and torso were decorated with amateur tattoos. The man, who spoke little English, displayed his scars to me and invited me to touch the hard patch of healing skin that concealed the pacemaker.
As Dr. Koumjian asked him how he felt, the man replied "feeling stronger," as he looked at the surgeon with what can only be described as an expression of enormous gratitude, almost adoration.
"You know that if you shoot drugs again you will probably die?" Koumjian asked him.
The patient nodded. He understood. “No mas,” he said. “No mas.”
Koumjian entered a dark, closet-like room and beckoned for me to follow. "Let me show you something," he said. He held a spool of film in his hand and then placed it in a cradle on a screening device that looked something like an editing machine. "This morning I'll be doing a triple bypass on a 72-year-old male. Maybe a quadruple bypass, I don't know yet. This is film of his heart." He switched on the screen, and a black-and-white film of dye moving through arteries and vessels writhed like smoke in a strobe light. He pointed out "blockages," which looked similar to the other patches of grey and white on the screen. In the darkened room, he silently studied the film, moving it back and forth in its cradle to replay the same sequence of dye being pumped through the chambers and tangles of vessels and ventricles. "Okay," he said after a time. "Let's go."
In the doctor's locker room we stripped and changed into hospital greens, shoe coverings, paper hats that tied beneath the chin, and masks. Koumjian scrubbed but told me I didn't need to unless I'd be operating. I wasn't to bring in a tape recorder, so I assumed this meant no notebook either. I followed him into O.R. #8, a brightly lit room the size of my apartment bedroom. Green-suited figures moved neither slowly nor hurriedly among the monitors, instruments, racks of sponges, and the heart and lung machine. It was impossible to tell who was a doctor, a tech, a nurse, the anesthesiologist. The coldness of the room struck me immediately. The temperature had been lowered for reasons having to do with protecting the heart. I was offered a shawl by one of the nurses but declined.
The patient's bald head was visible beneath a tangle of tubing monitored by Dr. John Ahlering, the anesthesiologist. He would be answering most of my questions in a quiet voice during the procedure. I was told to stand a few inches from the top of the patient's head. I did so and looked down at the jaundice-colored, Betadine-washed skin exposed in a square between navel and collarbone. Clinging to the skin was a plastic adhesive.
Another surgeon was already working on the patient's left leg. Dr. Gomez-Engler was introduced to me. He was busy opening the calf to remove the saphenous vein, which in turn would be grafted to replace the obstructed veins on the surface of the man's heart.
Without ceremony or fanfare, Koumjian used an electrical scalpel to make the incision in the center of the sternum. A radio in the O.R. was playing Wes Montgomery-style jazz guitar. The scalpel cauterized the tissue it cut, exposing yellow fat globules and quickly clotted blood. The smell of burnt meat and ozone in the room made me momentarily nauseated. Turning away, I asked John Ahlering what the patient would be feeling, if anything.
He told me that the man was given something like curare to paralyze him, something like morphine or heroin to deaden the pain, and a third drug in the Diazepam family to induce amnesia. "We want him absolutely still and not experiencing pain, but we don't want him to remember the experience either."
With the sternum exposed, Koumjian leaned over the patient with a fiber-optical loop fixed around his head. A small beam of concentrated light was attached to the headgear, like a penlight. A pair of Coke-bottle magnifying lenses distorted Koumjian's eyes into those of some subaquatic creature. The saw he wielded to open the bone joining the ribs looked like a butcher's saw.
"What is that thing?" I asked the anesthesiologist.
"It's a meat saw, basically."
The smell of burnt, cleaved calcium permeated the room, and again I turned to monitors and machinery to ask questions.
"This is the part that gets to people," said Ahlering. "Here, this is a pulse oximeter. It measures the oxygen in the blood. Have you met Ramey Stewart?"
I turned to meet the "perfusionist," a masked woman with large blue eyes behind wire-rimmed glasses. She would be in charge of the heart and lung machine. The patient's life would, in effect, be entrusted to her and several yards of tubing and pumps and thermometers and gauges while Koumjian cut and threaded veins in the man's heart.
"You okay?" she asked. The Moody Blues were on the radio, and they kept using the word heart in the song. "Fine. Fine. Thank you."
Ahlering started drawing me a diagram of the atrium, the ventricle, the aorta, and the lungs, pointing out the location of the mammary artery, which they would need access to in order to take a piece of it and graft it elsewhere. Stewart talked about the measurement of anti-coagulation, the necessity for the coldness of the room. "Activated clotting time...." she was saying. Ahlering was pointing out a monitor, "...wave form of exhaled CO2... tidal volume ... arterial pulse ... mixed venous oxygen ... pulmonary artery catheter...."
They were trying to distract me from the fact that Koumjian had now installed a rack of metal onto the patient's chest and was separating his rib cage with the thing by cranking a lever. The left side of the sternum was now elevated in a manner not unlike jacking up a car chassis.
"Sternum retractor," John said. "You okay?" I nodded. I had seen the inside of a human torso on cable TV, but this was very different. I was inches from the egg-like white tissue, the pericardium surrounding the heart that writhed and subsided rhythmically. As the rib cage was lifted, cranked, pulled farther away, I thought about the pain this man would feel in his back for days. Reading my mind, Koumjian turned to me and said, "What he'll feel afterward is a discomfort along his spine because of the retractor."
What I was feeling was a sudden lightheadedness, and Dr. Gomez-Engler suggested I sit down and place my head between my knees. I did this while Ramey Stewart distracted me with a running commentary on the intricacies of the perfusion device.
The next day, I made rounds with Koumjian and met the patient. He was sitting in a chair, not in bed, and seemed in good spirits. He was in no obvious pain, though catheters and IV tubing trailed from his body. Koumjian told him how well it had gone, and the man nodded, pleased. Twenty-four hours ago he had been all but technically dead — his heart still, his blood routed through yards of cool tubing, his chest open — with Michael Koumjian holding the 800 grams of heart in his hand like a trembling animal.
Comments