 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube
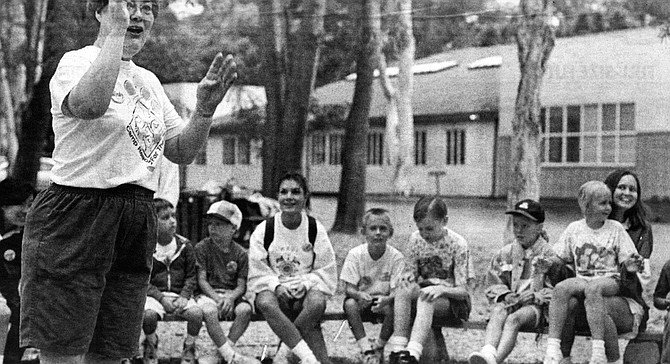
Six-year-old Michael Nava is as bald and brown as an almond. He is covered from head to foot in sunscreen lotion. A towel is draped around his shoulders, his swim trunks are comically baggy and his Sandals — day-glo rainbow — appear neon against smoothly tanned feet. The white catheter surgically implanted in his chest is covered with gauze and waterproof tape because Michael is going swimming with the rest of the kids in the Balboa Park pool.

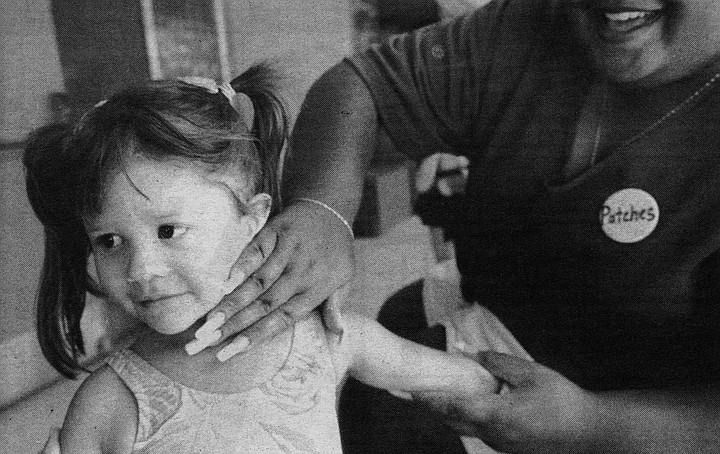
Accompanied by teenaged camp counselor volunteers with name tags like “Beetle Juice, ” “Puddles,” “Patches,” and “Tinkerbell,” Nava walks from the Girl Scout camp (headquarters for the week for Camp Reach for the Sky) to the pool area some 50 yards away. He passes two metal-dome recycling bins and pauses in his discussion of Sega CD video games. He points at the ovoid objects and says, “Hey, those things look just like me!”
The pretty teenaged girls holding his hands have dropped them. They put their fingers to their lips as they giggle, and Nava looks up at them with glee, his eyes wide, hairless eyebrows arched. The young cancer patient apparently delights in messing with the unspoken taboo about mentioning a kid’s hair, lack of it, catheter tubes, or unusual scars. Half an hour earlier, Nava had lifted his shirt, pointed to a long horizontal scar just above his navel with puncture scars above and below the incision line. “See? They stapled me, ” he said.
“They stapled you, huh?” I say.
“Yep. ” He nodded matter-of-factly. “Just like paper. ”
In February of 1986 I was working behind a bar in Ocean Beach wearing a gaudy blue Hawaiian shirt and a gauze patch with surgical tape over a biopsy incision on my neck. It was happy hour, about 4:30. The phone rang and I answered it with the name of the business. Someone asked for me.
“Speaking. ”
“This is Dr. Bassett. I have your biopsy results.”
“Oh. All right. What is it?”
I have no recollection of what he said other than he used a word ending in “oma” and a phrase I found fascinating but meaningless, like some sort of poetry in a dream. He said something about “the architecture of the node.”
“Oma?" I asked into the phone.
“Architecture of the node?” My happy-hour customers looked at me strangely, as if I were suddenly speaking in code, in tongues, or undergoing a seizure of some sort. I certainly must have looked angry or frightened. “Oma? Oma? When you say ‘something-oma,’ that means cancer, doesn’t it?”
“Yes, ifs a particular type of lymphoma. Hodgkin's disease. Sometimes they call it the young adult’s disease."
“But it’s cancer, right?"
“Yes, it is."
“All right. Thank you. I have to go now."
I hung up and refilled drinks, took cash and washed glasses. One of my regulars asked me, “What was all that about on the phone?"
I said, “Oh, just more crap I don’t need on top of this divorce shit and the girl I’ve been seeing with her old boyfriend in town and the car and taxes and everything else. ”
“Sounded like you were talking about cancer. ”
“Yeah, now I’ve got cancer."
“You seem to be taking it pretty good, man.”
“Well, what am I supposed to do?” I almost screamed at him.
I didn’t know how I was supposed to feel. I went home that night and wrote on a piece of paper, “February 23, 1986: I have cancer.” I stared at it for an hour and smoked cigarettes. I had no idea what it meant except that I was probably going to die.
I was 35 years old.
“Camp Reach for the Sky is a week of summer fun for cancer patients....” the press sheet from the American Cancer Society reads,
There’s watersports, campfires and laughter, games and more laughter...it’s time for a kid to be a kid.... It’s more than a camp for children with a history of cancer, it’s a chance for these kids to escape from a clinical environment and enter nature’s environment...an opportunity to enjoy a normal childhood experience. There are no awkward questions.... The camp has a medical staff of professionals who have taken time to volunteer...known more as counselors and friends than doctors and nurses. This year there are two camps, a day camp at Balboa Park for ages four to eight, which runs July 18th through July 22nd. The resident camp in Julian at the YMCA’s Camp Marston is for ages eight to eighteen and runs from August 15th through August 20th.
The day begins at the scout camp just west of Roosevelt Junior High on Upas Street. The children are seated on a circular bench some 30 feet in diameter. At the center is camp director Barbara “Windy” Wiggins, who leads the nearly 50 children in song: “Hi, my name is Joe and I work in a button factory.... I’ve got a wife and a dog and a family....”
“The wheels on the bus go round and round....”
“All the other frogs go frodyodyodyoh, frodyodyodyoh....”
And a song resonant with imagery under the circumstances:
“I stuck my head in a little skunk's hole.
The little skunk said, 'Upon my soul.
Take it out, take it out... remove it!’
Well, I didn’t take it out, and the little skunk said,
‘If you don’t take it out, you’ll wish you were dead!’ Take it out, take it out, take it out!
But I removed it too late.”
Wiggins introduces arm and leg movements to accompany the songs, and for the most part, the children follow with an approximate choreography.
One final chant led by Wiggins is “Rain, rain, go away, come again another day,” though it is not raining, merely an overcast July morning. The members of Camp Reach for the Sky do indeed raise up their arms to the cloud cover, and the invocation works perfectly as the sun emerges within the hour, scattering leafy shadows, warming the grass and wading pool, driving counselors to the sunscreen lotion, and inspiring the appearance of paper cups of soft drinks.
The oldest child at the camp today is 15-year-old Leo Coburn, and he is making a valiant attempt to follow along with the simplest of gestures but is clearly having difficulty. It is as if he cannot quite remember where he is from moment to moment or is trying to bridge some gap visible only to him between himself and the other children.
Coburn has had a brain tumor removed and will remain “challenged indefinitely.”
Cindy Fujii will accept those words warily. Fujii, formerly a resident at UCSD, is now a pediatrician at Kaiser Medical Center and volunteer camp physician.
“We have kids at basically all stages of their disease. We have some kids who have been newly diagnosed, kids right in the middle of their chemotherapy, some kids in their maintenance phase, and some kids who are on their second course of treatment because of a relapse. We have a lot of kids who are in remission.”
“That’s one of my favorite words,” I tell her.
Fujii, a 30ish, attractive Asian woman, smiles owlishly behind round, horn-rimmed glasses. “Yeah, that’s a nice word, isn’t it?”
Fujii’s name tag reads only “Acorn.” “There is a different group of physicians for the resident camp [Camp Marston], because the campers are a little bit older and they are staying overnight. It is primarily staffed by the hematology/oncology docs themselves. The day camp [Balboa Park] this year primarily staffed by community pediatricians, but the hematology/oncology docs drop in once in a while. Otherwise, it’s all volunteers.
What kind of medical problems does Fujii encounter in the camps?
“We do all the basic first aid and any stabilization they might need, but for the most part, since we're near all the major medical centers, it's more just temporizing until we get them to their primary hospitals or doctors. It’s mostly just a matter of cuts and scrapes. We check everybody, including the staff, for runny noses and signs of colds or flu, because some of the children may be immune-compromised because of treatment.”
Two girls dip Frisbees in the plastic wading pool. The girls are Dominique Bumpas and Jessica Plascha, both four years old. Dominique has long strawberry-blond hair and a fair complexion with freckles. Jessica has equally long but darker hair. As I approach, the girls seem to share some telepathic instinct to fill their Frisbees with water, pivot at exactly the same moment, and spray me, my beard, tape recorder, and new shirt with water.

Immediately, their faces drop in something like terror as I stand there sputtering, shaking my recorder and blinking water out of my eyes. It is as if, on the heels of that simultaneous impulse to douse a grownup, the thought followed, “Uh-oh, what did we just do?” and froze them in fear. My concern shifts from my clothes and cassette to the almost comic horror on the girls' faces.
“Hey, that’s okay. I’m fine. It's just water.”
Jessica is still not quite assured, “Are you gonna get in trouble with your mom now?” she asks in all seriousness.
“Oh, no,” I say. “That shouldn’t be a problem.”
David Sine is in his 20s, wears a USD sweatshirt, has unruly blond hair beneath a baseball cap turned backwards on his head, appears unshaven and more like a parks-department maintenance worker or homeless park resident than an M.D. His manner is casual, even serene. He does not speak much, but the children tend to flock around him and talk to him as if they are trying to bring him out of some shell.
Sine is from Canada and a second-year pediatric resident at Children’s Hospital and UCSD. Sine worked as a nurse at Camp Trillium for seven years, a similar cancer camp for children in Ontario, while he studied for his M.D. “I’m here strictly as a volunteer,” Sine says, a recurring refrain among all the adults. (The only exception is ACS liaison Kimberly Dark, a paid employee.) “I’m not here for medical reasons,” Sine continues. “That’s a separate part of my life than this. It’s just nice to see the kids in this environment. We do look for fatigue in the kids that are on therapy. We have to be careful of any exposure to anyone with viruses or colds. Kids on therapy are more susceptible to getting sick from that. Every day they screen both the campers, adults, kids with cancer, and kids that don’t have it.”
“Are there children being treated for leukemia here?”
“Yes, there are. But it’s not necessarily important to know who’s who. It’s really only the camp leaders who need to know who has cancer and who doesn’t. You can see that the kids that are bald or don’t have much hair are on therapy still, but otherwise there are kids here who are cured and been off therapy for years. Sometimes more than that. It’s a place for kids to be kids rather than to be kids with cancer.”
Are there patients of Sine’s among the group here today of (mostly) three- to nine-year-olds?
“Yes, there are a couple as far as in-house, in hospital.”
“How are they doing?”
“They’re doing real well. All the ones here pretty much have to be at a certain level to be able to actually come to camp. The kids that are still on aggressive therapy are in the hospital, and they can’t come to camp. Once they get to a point they call maintenance therapy, where you’ve pretty much treated the cancer in the body and you want to make sure none of it comes back. Those are the kids who would come here. The cancer, for the most part, is out of their body, and you’re keeping it out with chemotherapy.
“These are all outpatients. There are a few kids who have to go into the hospital for three or four days for treatment.”
“Any of them being treated for Hodgkin’s?” I ask.
“I don’t know. You’d have to ask some of the medical staff. Why?”
I mentioned that I had it and that it might be of some help to talk with a child who suffered from that lymphoma. But the medical staff and counselors are protective, and rightly so. Medical case histories are given out sparingly. No one I knew of that day was being treated for Hodgkin’s. I looked for the weight loss, paleness, sweating, nausea, but whatever I saw was just as likely due to the sun, any kind of chemotherapy, prolonged hospitalization, or too much fruit punch and cookies.
Looking around at the kids painting maple and oak leaves with bright tempera paints (later to be imprinted on T-shirts) or swinging plastic whiffle bats the size of small grain silos at plastic balls or listening attentively to the parks-department volunteer lecture on trees, acorns, pine cones, I ask Sine, “Are any of the kids here terminal?”
“I really wouldn’t know that,” he says, but looks as if he does.
My friend Rick in New York, a science-fiction writer with a multiple-book contract he had to deliver pronto, was also diagnosed around the same time as I was. Like me, he had another “good cancer,” “the kind you want to pick if you have to pick one.” These were phrases we had each heard doctors mention.
We compared other stock phrases like “Why did you wait so long?”; “Hope for the best but prepare for the worst”; and “A positive attitude can be of immeasurable value,” which we took to referring to as the “If you eat wheat grass and think good thoughts, who knows?” school of oncological shrugging.
Rick had colon cancer. Giddy with joints (him) and Scotch (me), our conversation went something like this:
“I’m sorry, Rick. That’s really shitty.”
“Bad choice of words. You should have node better.”
“Well, it will all be behind you soon.”
‘'Yes, it’s a bummer.”
“Can’t live forever.”
“June would be nice.”
And Rick used both his cancer and the tremendous pressure to produce an 80,000-word book in an ingenious manner. He wrote one of the strangest psychological urban fantasy novels I’ve ever read. It is called The Feral Cell, and it is brilliant and funny and poignant. It is about cancer.
Meanwhile, I used my time to write another novel that had as little to do with my illness as possible. While Rick used (to borrow Susan Sontag’s phrase) illness as metaphor, I used fiction to get the hell out of the Dodge City of my body and head. Rick saw his body as a canvas, a kind of landscape of conflict against good and evil. I saw mine as an ally turned enemy, pure and simple.
I actually ate wheat grass a few times, but for the first six months of my treatment, I rarely thought good thoughts.
I wept, I got pissed off at everything and everyone, I groveled and whined to a God I wasn’t sure was on the other end of that big white telephone into which I was hurling crackers, rice, potatoes, nitrogen mustard, and procarbazine. I prayed to God as if he were Monty Hall on Let’s Make a Deal.
I went to a curandera in Mexico who rubbed me down with coyote oil, brushed me with fresh-picked sage like a butler grooming the master before the opera. She spat into the base of my neck and wrapped me with a towel while two friends tugged either end as if I were a wishbone. I became blissful at my approach to the edge of this mortal coil and started making mystical pronouncements to my friends and family about meaning, desire, sin, and the mysteries of love. Most of this was a direct result of the Tylenol and codeine I was given to stop the feeling that my upper torso had become something of a sharp, white-hot yoke around my neck.
I did too little laughing, even when my oncologist recommended smoking grass for the nausea (I would merely become paranoid, thinking, Oh, man. I’m stoned and I’ve got cancer). I reacted every possible way a neurotic adult might.
And this is why, eight years after I heard the word “remission” from Doctor Death (as I came to think of him), it occurred to me that children are the teachers here. Adults with cancer should seek out Reach for the Sky and places like them. It’s well and good to rage against the dying of the light, but it might be a better use of one’s time to celebrate it, shadows and all, while it lasts.
Children don’t need to be taught this. They are better poised for the mortal realities of life-threatening illness if for no other reason than they instinctively know two things: It is better to be alive than dead and I’m not dead yet. It’s not dark yet, Mom...let me just finish painting this leaf, let me get from 3rd base to home. I’ll be in in a minute. One more minute...okay?
Justine Fry is eight and a half years old, an enthusiastic singer, conversationalist, and third baseman. Fry’s blond hair never quite fully restored itself after radiation treatments. She has been in remission for years but still looks as if she is undergoing treatment. Except, of course, that she has far more energy than anyone could possibly summon getting nuked with rads, hyped on prednisone, poisoned with nitrogen mustard, procarbazine, or vincristine — whatever.

Justine is dressed in pink shorts and T-shirt. She wears small earrings, and she braces one sneaker against the live oak that serves as third base. She is poised to move fast, retrieve a grounder, or tag out her brother J.J., who seems determined to steal all his bases. In this game the ball is a beach ball and players are just as likely to get thrown out by getting beaned or backsided with the thing as to be tagged.
Justine Fry chases down her runners, even if it means going around all the bases twice, pursuing them into the outfield or well into foul territory. Determination seems to exude from her focused gaze, body language, and steady, confident speaking voice. As the game winds down (evaporates, really, as players wander off for snacks, drinks, games of tag, contemplative nose-picking, the bathroom), Justine Fry has a moment for a post-game interview.
“I was sick for a long time,” she says.
“How long?”
“Um, a year or months or...I don’t know.”
“Do you still have to take medicine or go to the radiation machine?”
She shakes her head “No.”
“Well, good.”
“It was horrible in the hospital.”
“What was the most horrible thing?”
“It was when I went to bed and then they would wake me up in the middle of the night. But my dad was in the hospital in the next bed, and he slept with me every night.”
“Why did they wake you up?”
“Well, my dad would wake me up because I had to get a shot in the middle of the night.”
“Oh, yeah, I had to get those too. Did it make you throw up? That’s what I used to do.”
“No,” she seems to be trying to remember, as if this was something that had escaped her memory. “It was just horrible waking up when I was sleeping, and the needle hurt.”
Indeed, Sine had indicated that the incidence of nausea tended to be much less in child patients. “Children often tolerate chemotherapy better than adults,” he had said.
“See,” Justine explains, “my dad was in the Navy, and he worked in the hospital, so he was actually right next to me. And at home, when I first got sick and had to go to the hospital, they let him ride in the ambulance with me and hold me.”
“Do you know what they called it, what you had?”
“No.” She shakes her sparse corn-silk hair. “It was a long time ago. It started when I was two. And when it was all over, I couldn’t walk or anything. I had to be potty-trained all over again. It was hard.”
Justine Fry was diagnosed six years ago with something called rhabdomyosarcoma. “It was,” says her father, former E4 Naval Corpsman John Fry, “a tumor basically in her temple, behind her left eye and back in her nasal passages. I was in the military at the time. Her oncologist was a Dr. Thomas, now in Washington state. I have to tell you, I owe that guy everything. She’ll have been in remission five years as of this month [August]. We’re gonna throw her a little shindig.
“Yeah, she spent about the first three months after diagnosis in the [Balboa] hospital, and I was working the emergency room. They were nice enough to give me the first month off to be with her; and after that, my wife Laurie would stay with her during the day, and I would have the evenings because I was working anyway. Justine was in and out [of the hospital] for the next year and a half. She got to know everybody there pretty well.”
Laurie Fry remembers the symptoms that led to the ambulance ride her daughter just described. “She had lost a lot of weight over a short period of time, and she was always crabby. She slept 20 hours at a time, and her left pupil dilated abnormally.”
“She had,” recalls John Fry, “about a year and a half of chemo and about six weeks of full head radiation. That’s why the patchy hair; that’s pretty permanent.”
Any other lingering problems?
“Yeah, she lacks a little bit of manual dexterity from some of this stuff. You know, she’s blind in her left eye, so depth perception’s a little tough. The tumor pinched off her optic nerve on that side. She couldn’t see a Jeep; you could blindside her from that side. But she compensates pretty well. She still gets some drainage from her ears and her nose, and so sometimes balance things are a little bit tough for her.”
Justine Fry will be entering the third grade in Oceanside. “She’s a great artist,” says her father, whose critical artistic sensibilities may be exceeded by paternal myopia. “She can sit in her room for hours drawing, cutting stuff up and gluing it together. She’s great.”
Though Justine goes to school all year round, she has been given the week off for Camp Reach for the Sky. She has gone every year since she was three years old. “In fact,” says her father, “you probably shouldn’t tell the Cancer [ACS] people about this, but Dr. Thomas was nice enough to — even when she wasn’t old enough, kind of wrote her a little note and got her in. She gets to go to the resident camp next year.”
According to the American Cancer Society booklet “California Cancer Facts and Figures 1994”:
[Cancer] kills more children age 1 to 14 in the U.S. than any other disease. Among adults it occurs more frequently with advancing age. In the 1980s, it was estimated there were over 470,000 cancer deaths in California, almost 1 million new cancer cases and some 1.3 million people under medical care for cancer.
About 9 million Californians now living will eventually have cancer; about one in three according to present rates. Over the years, cancer will strike in approximately three of four families. Even if incidence rates remain constant, this number of new cases will continue to grow as the California population increases due to migration and the aging of the population.
There are over 776,000 Californians alive today who have a history of cancer, 331,000 can be considered cured, while others still have evidence of cancer. By “cured” it is meant that a patient has no evidence of disease and has the same life expectancy as a person who never had cancer.
The decision as to when a patient may be considered cured is made by the physician after examining the individual patient.
For most forms of cancer, five years without symptoms following treatment is the accepted time. Nevertheless, some patients can be considered cured after one year and others after three years, but some have to be observed much longer than five years.
The smell of damp carpeting to this day nauseates me, can blind me with headaches and panic. Doctor Death (or Dr. Vincristine I sometimes thought of him) had his office on the second floor of a building on Fourth Avenue near Mercy Hospital. I would take the stairs because I would always run into really sick-looking people in the elevators. The problem was, the carpeted stairway always smelled of mildew and disinfectant. Ascending the stairs on my way to intravenous chemo sessions, my stomach would churn with the anticipated hours of vomiting. The association between the smell of mildew and Pine-Sol and sickness and death remains with me still.
The first time I heard the word “remission” was within a week of my visit to the curandera. I am not suggesting there is any causality here, only synchronicity. And it is not the proximity of these two events that I found disconcerting or puzzling, it was, rather, Now what? I’ve spent a year rehearsing for the Big Sleep and it looks like I’m going to live after all. How do I do that? This is unfair. They've changed the rules on me. Doctor Death, now Doctor Get-a-Life, grinned toothily at me and extended his hand for me to shake. “Congratulations!” he said as I took his hand and smiled back as life-affirmingly as I could. “Welcome to maintenance therapy!” he said.

Fifteen-year-old Leo Coburn is making a flying saucer out of a plastic coffee-can lid and a Styrofoam dome decorated with paste-on stars and felt-tip pen markings. David Sine sits quietly at the corner of the long folding table, and Coburn demonstrates his construction to the mellow, almost sleepy-looking doctor and volunteer counselor. Briten and Kirsten Douglas, two seraphic blond sisters aged, respectively, seven and nine, are immersed in a crafts project with these same components. A half dozen other children are engaged in their own versions of similar activities, and though Sine elicits no explanation from the children as to just what it is they think they’re making, many of the campers give running progress reports to “Maple Leaf” (Sine’s button), elaborate descriptions of their creations (snowmen, igloos), comments on the difficulty and technique involved in getting the Styrofoam to take the felt-tip ink. Sine smiles, approves, and expresses an even interest: “Is that what that is?” His responses and attention, his slow smile seem to reassure the children that Sine doesn’t feel left out.
“It’s a flying saucer!” announces Coburn. He has to repeat himself a few times; his enunciation is sometimes unfocused.
“Hey, that turned out neat, didn’t it?” Sine looks pleased. “Try to throw it. See if it’ll fly.”
“Not inside,” Coburn corrects Sine. “Outside. In space.” Coburn tosses his saucer off the front porch of the scout lodge. It tumbles a few feet and lies in the grass at the foot of the steps. Coburn smiles up at Sine as if he had just demonstrated an interesting new example of Newtonian physics. Sine nods his head with appropriate approval.
“Briten was diagnosed with leukemia March 10 of ’91,” says Corinna Douglas, Briten’s mother. “She just finished her three-year protocol at the end of this last year. The day before Christmas she got her Hickman out.” The Hickman is the catheter implanted in the skin, usually the chest, to facilitate IV treatment. It precludes the necessity to constantly puncture the skin during treatment.
“The chemotherapy is completed,” says Douglas. “She is now in this surveillance phase, where the doctors don’t give you any real vote of confidence. We’re in that critical year to see how she does off chemo. The thing she has going for her is that she has responded to the chemotherapy and has stayed in remission for almost three years. Now to hold on to it is what we’re all hoping for.”
“So another 18 months or so and she’ll be out of the woods?”
I ask.
“Well, they never say that. They never say that you are out of the woods.” Douglas sounds tired, a little frustrated. “Only that she’s in remission and what her survival hopes are. But three years ago I could never have imagined being where I am now. It was just unforeseen that we could have possibly come out of this.”
At any point did Douglas resign herself to losing her daughter?
She answers carefully. “I was...resigned...in the sense of preparing for the worst, but hoping for the best.” That phrase again. I could never decide if it was a Zen koan or just double-talk.
“Briten was born with bladder atrophy, that is, she was born without a bladder and without a pelvis. When she was four hours old, she had seven and a half hours of reconstructive surgery. At that point in time, they told us there was a good chance she was not going to make it, but that if she does, she’s going to have a very compromised life. ‘She may never walk,’ they said. ‘And if she does walk, we don’t know the significant problems she will have.’ So we figured, this is the way her life is gonna go. At the time, I already had a 22-month-old baby at home.
“That preparation helped us to deal with the next phase,” Douglas continues, “which was her [Briten’s] diagnosis with cancer by the time she turned four. But if you recall what Briten looked like [the previous week at the camp], you wouldn’t know. I mean, the resilience of that kid!”
Indeed, Briten Douglas appears as healthy as any seven-year-old one might point to. Yet Douglas laughs, “She’s had us on an emotional roller coaster from the first day she was with us.”
How did Briten’s symptoms of leukemia announce themselves?

“She woke up in the middle of the night and came into our room and said she had a knife in her stomach, ‘Take me to the doctor to get the knife out.’ We were thinking it had something to do with her other problems. I couldn’t call a pediatrician up in the middle of the night and say, ‘My baby has a stomachache.’ I just told her to go to the bathroom. We were trying to treat things normally. But her earnest comment, ‘Take me to the doctor now’ prompted us to call. Our pediatrician happened to be on call at the time at our hospital here in Escondido. He took a blood, test, and since he was in the oncology field, he knew immediately that 69 percent of her was cancerous blast cells. Leukemia is basically an overproduction of white blood cells.”
The ACS “California Facts and Figures 1994,” under Major Cancer Sites, Leukemia, states, “There has been dramatic improvement in the outcome of acute childhood leukemia. The majority of children are cured and live into adulthood leading normal lives.” This, according to tables included in the booklet, is a 30 percent improvement in survival figures in as many years.
“We are just in that transition now,” says Corinna Douglas, “where we’re finally past the throwing up and the painful treatments and the dressing changes for the hip, and her hair has finally all grown back. She still has to have spinal taps every three months because, for some reason, the relapses they are seeing occur in the bone marrow even if it was not previously cancerous.”
What was Briten’s sister Kirsten’s reaction to the years of illness?
“The roller coaster on that was very, very tough. She had a very difficult time because we had to ship her to anyone we could at times. We don’t have that many family members that could support us here in California because most of our family is on the East Coast. It came down to my husband and myself — one of us being at the hospital and one of us trying to get Kirsten squared away. Dad needed to be in the hospital with Briten as much as I needed to be there. The message to Kirsten was, ‘You’re the well one. You have to stay strong.’
“It was hard on her because she would have to endure a lot of different households and uncertainties. She would go to kindergarten with a suitcase and a note telling her teacher so-and-so is going to pick her up. We had to rely on a lot of people coming out of the woodwork to help us out. She is now nine, and she still does not appreciate having to spend the night away anywhere. She has this phobia. It’s really hard to imagine that a kindergartner would want to kill herself, but Kirsten really, really did want to kill herself.”
How long did this go on?
“That lasted a good portion of the first year Briten was in the hospital. She was very, very worried about her sister, worried about us. She had grown up seeing her sister in this medical world. She had to wonder, ‘When will this stop? When will I get to be the focus?’
“I have now come to realize,” says Douglas, “that children that are presented these challenges in life are much brighter than you ever could imagine. They can handle it. Briten was very courageous; she knew she had to fight the fight. And in that battle, over the years she has witnessed friends — within the treatment room and the hospital — dying. And then attending their funerals.”
Waiting at poolside with lifeguard Paula “Boom-Boom” Ferraco, ACS liaison Kimberly Dark, assistant unit leader Susan “Beanie” Bean, and various other adults and children such as Shyloh Zurn and Leo Coburn’s nephew Chris Gray. Michael Nava dangles his feet in the water while Beanie plays drowning victim and “Boom-Boom” gives instructions on water safety.
In a demonstration involving a drowning victim (the dramatic Beanie — “Help! Help! Oh, my!”) being rescued by poolside buddy Leo Coburn (who lies prostrate at the edge of the pool to minimize danger of being pulled in along with the victim), rescuer Coburn points out the alternative lesson that it is possibly more fun to allow oneself to be pulled into the pool by a hammy actor than to go along with the fake lifesaving gag. Mike Nava warns several kids against a dive-bombing beetle and is wary when it is explained to him they cannot hurt you, “How do you know?” he asks suspiciously.
When fellow camper John Baxter (excellent batting stance but unenthusiastic interview subject) asks Nava what his Hickman catheter covered in waterproof tape is for, Nava answers, “For what they do to me, they poke hard. This is so I don’t get pokes on my arm.” He points out the scar on his stomach again and the staple marks. He announces proudly, “When they took ’em out, it didn’t hurt. I didn’t use the sleepy medicine, I didn’t use the not-feeling medicine or nothing. My brother Tony has a Walkman and a boom box and the Michael Jackson Thriller CD.”
Nava swims with the best of them and gives impromptu math tests to his companions, who are less than appreciative of Nava’s excellence in this area. He looks like a child as full of life and health, humor, and awe as could be asked for. He is merely bald and has plastic straws surgically implanted in his chest cavity and has a tumor in his liver.
Nava has gone through five types of chemo treatment in the past two years. He is currently undergoing a course of treatment known as I.C.E., which stands for the chemical names of the poisons he is given. I.C.E. is a particularly brutal chemical course and is something of a last resort for Nava’s parents, because Nava’s case is one in a hundred, and oncologists get few opportunities to study cancers like his. Nava’s mother’s attitude is “Whatever it takes.” Nava’s scar is a result of exploratory surgery that revealed the tumor to be inoperable. The six-year-old is on a “nonactive” waiting list for a liver donor. Last September, around Michael’s birthday, he relapsed, and so the course of chemotherapy had to be altered again. The Make-a-Wish Foundation rose to the occasion and raised $1900 for Michael and arranged a trip for him to Disneyworld, where Nava could cruise the gift shops and “pick out anything he wanted,” his mother says.

“He would just point to whatever and say, ‘I’ll have one of those and one of those.’ Now Michael thinks the Make-a-Wish Foundation is this kind of genie. This year for his birthday he wants the foundation to arrange for him to legally change his name from Michael Nava to Michael Jackson.”
What are the doctors saying about Nava’s prognosis, his chances, his future?
Mrs. Nava pauses, sighs. “No one really knows.”
In mid-September Gloria Nava called to say that Michael’s I.C.E. treatment was no longer working. “The doctors told me there was nothing more they could do. They told me it was a matter of weeks or a month.” One of Nava’s oncologists did suggest a last-ditch effort involving the experimental drug topotecan, a natural extract from tree bark. Nava is currently undergoing treatment involving this drug under the supervision of Dr. Alice Yu, professor of pediatrics at UCSD Medical School. Of the treatment, Yu said only, “We know very little about it. It is very experimental.”
When asked to comment by phone, the seven-year-old patient was playing a video game and said only, “Not now. I’ve got to concentrate.”

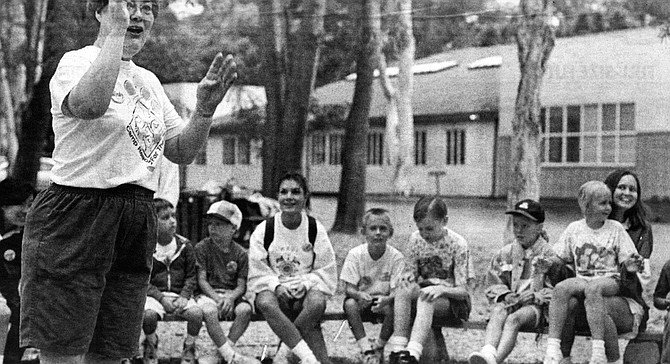
Six-year-old Michael Nava is as bald and brown as an almond. He is covered from head to foot in sunscreen lotion. A towel is draped around his shoulders, his swim trunks are comically baggy and his Sandals — day-glo rainbow — appear neon against smoothly tanned feet. The white catheter surgically implanted in his chest is covered with gauze and waterproof tape because Michael is going swimming with the rest of the kids in the Balboa Park pool.

Accompanied by teenaged camp counselor volunteers with name tags like “Beetle Juice, ” “Puddles,” “Patches,” and “Tinkerbell,” Nava walks from the Girl Scout camp (headquarters for the week for Camp Reach for the Sky) to the pool area some 50 yards away. He passes two metal-dome recycling bins and pauses in his discussion of Sega CD video games. He points at the ovoid objects and says, “Hey, those things look just like me!”
The pretty teenaged girls holding his hands have dropped them. They put their fingers to their lips as they giggle, and Nava looks up at them with glee, his eyes wide, hairless eyebrows arched. The young cancer patient apparently delights in messing with the unspoken taboo about mentioning a kid’s hair, lack of it, catheter tubes, or unusual scars. Half an hour earlier, Nava had lifted his shirt, pointed to a long horizontal scar just above his navel with puncture scars above and below the incision line. “See? They stapled me, ” he said.
“They stapled you, huh?” I say.
“Yep. ” He nodded matter-of-factly. “Just like paper. ”
In February of 1986 I was working behind a bar in Ocean Beach wearing a gaudy blue Hawaiian shirt and a gauze patch with surgical tape over a biopsy incision on my neck. It was happy hour, about 4:30. The phone rang and I answered it with the name of the business. Someone asked for me.
“Speaking. ”
“This is Dr. Bassett. I have your biopsy results.”
“Oh. All right. What is it?”
I have no recollection of what he said other than he used a word ending in “oma” and a phrase I found fascinating but meaningless, like some sort of poetry in a dream. He said something about “the architecture of the node.”
“Oma?" I asked into the phone.
“Architecture of the node?” My happy-hour customers looked at me strangely, as if I were suddenly speaking in code, in tongues, or undergoing a seizure of some sort. I certainly must have looked angry or frightened. “Oma? Oma? When you say ‘something-oma,’ that means cancer, doesn’t it?”
“Yes, ifs a particular type of lymphoma. Hodgkin's disease. Sometimes they call it the young adult’s disease."
“But it’s cancer, right?"
“Yes, it is."
“All right. Thank you. I have to go now."
I hung up and refilled drinks, took cash and washed glasses. One of my regulars asked me, “What was all that about on the phone?"
I said, “Oh, just more crap I don’t need on top of this divorce shit and the girl I’ve been seeing with her old boyfriend in town and the car and taxes and everything else. ”
“Sounded like you were talking about cancer. ”
“Yeah, now I’ve got cancer."
“You seem to be taking it pretty good, man.”
“Well, what am I supposed to do?” I almost screamed at him.
I didn’t know how I was supposed to feel. I went home that night and wrote on a piece of paper, “February 23, 1986: I have cancer.” I stared at it for an hour and smoked cigarettes. I had no idea what it meant except that I was probably going to die.
I was 35 years old.
“Camp Reach for the Sky is a week of summer fun for cancer patients....” the press sheet from the American Cancer Society reads,
There’s watersports, campfires and laughter, games and more laughter...it’s time for a kid to be a kid.... It’s more than a camp for children with a history of cancer, it’s a chance for these kids to escape from a clinical environment and enter nature’s environment...an opportunity to enjoy a normal childhood experience. There are no awkward questions.... The camp has a medical staff of professionals who have taken time to volunteer...known more as counselors and friends than doctors and nurses. This year there are two camps, a day camp at Balboa Park for ages four to eight, which runs July 18th through July 22nd. The resident camp in Julian at the YMCA’s Camp Marston is for ages eight to eighteen and runs from August 15th through August 20th.
The day begins at the scout camp just west of Roosevelt Junior High on Upas Street. The children are seated on a circular bench some 30 feet in diameter. At the center is camp director Barbara “Windy” Wiggins, who leads the nearly 50 children in song: “Hi, my name is Joe and I work in a button factory.... I’ve got a wife and a dog and a family....”
“The wheels on the bus go round and round....”
“All the other frogs go frodyodyodyoh, frodyodyodyoh....”
And a song resonant with imagery under the circumstances:
“I stuck my head in a little skunk's hole.
The little skunk said, 'Upon my soul.
Take it out, take it out... remove it!’
Well, I didn’t take it out, and the little skunk said,
‘If you don’t take it out, you’ll wish you were dead!’ Take it out, take it out, take it out!
But I removed it too late.”
Wiggins introduces arm and leg movements to accompany the songs, and for the most part, the children follow with an approximate choreography.
One final chant led by Wiggins is “Rain, rain, go away, come again another day,” though it is not raining, merely an overcast July morning. The members of Camp Reach for the Sky do indeed raise up their arms to the cloud cover, and the invocation works perfectly as the sun emerges within the hour, scattering leafy shadows, warming the grass and wading pool, driving counselors to the sunscreen lotion, and inspiring the appearance of paper cups of soft drinks.
The oldest child at the camp today is 15-year-old Leo Coburn, and he is making a valiant attempt to follow along with the simplest of gestures but is clearly having difficulty. It is as if he cannot quite remember where he is from moment to moment or is trying to bridge some gap visible only to him between himself and the other children.
Coburn has had a brain tumor removed and will remain “challenged indefinitely.”
Cindy Fujii will accept those words warily. Fujii, formerly a resident at UCSD, is now a pediatrician at Kaiser Medical Center and volunteer camp physician.
“We have kids at basically all stages of their disease. We have some kids who have been newly diagnosed, kids right in the middle of their chemotherapy, some kids in their maintenance phase, and some kids who are on their second course of treatment because of a relapse. We have a lot of kids who are in remission.”
“That’s one of my favorite words,” I tell her.
Fujii, a 30ish, attractive Asian woman, smiles owlishly behind round, horn-rimmed glasses. “Yeah, that’s a nice word, isn’t it?”
Fujii’s name tag reads only “Acorn.” “There is a different group of physicians for the resident camp [Camp Marston], because the campers are a little bit older and they are staying overnight. It is primarily staffed by the hematology/oncology docs themselves. The day camp [Balboa Park] this year primarily staffed by community pediatricians, but the hematology/oncology docs drop in once in a while. Otherwise, it’s all volunteers.
What kind of medical problems does Fujii encounter in the camps?
“We do all the basic first aid and any stabilization they might need, but for the most part, since we're near all the major medical centers, it's more just temporizing until we get them to their primary hospitals or doctors. It’s mostly just a matter of cuts and scrapes. We check everybody, including the staff, for runny noses and signs of colds or flu, because some of the children may be immune-compromised because of treatment.”
Two girls dip Frisbees in the plastic wading pool. The girls are Dominique Bumpas and Jessica Plascha, both four years old. Dominique has long strawberry-blond hair and a fair complexion with freckles. Jessica has equally long but darker hair. As I approach, the girls seem to share some telepathic instinct to fill their Frisbees with water, pivot at exactly the same moment, and spray me, my beard, tape recorder, and new shirt with water.

Immediately, their faces drop in something like terror as I stand there sputtering, shaking my recorder and blinking water out of my eyes. It is as if, on the heels of that simultaneous impulse to douse a grownup, the thought followed, “Uh-oh, what did we just do?” and froze them in fear. My concern shifts from my clothes and cassette to the almost comic horror on the girls' faces.
“Hey, that’s okay. I’m fine. It's just water.”
Jessica is still not quite assured, “Are you gonna get in trouble with your mom now?” she asks in all seriousness.
“Oh, no,” I say. “That shouldn’t be a problem.”
David Sine is in his 20s, wears a USD sweatshirt, has unruly blond hair beneath a baseball cap turned backwards on his head, appears unshaven and more like a parks-department maintenance worker or homeless park resident than an M.D. His manner is casual, even serene. He does not speak much, but the children tend to flock around him and talk to him as if they are trying to bring him out of some shell.
Sine is from Canada and a second-year pediatric resident at Children’s Hospital and UCSD. Sine worked as a nurse at Camp Trillium for seven years, a similar cancer camp for children in Ontario, while he studied for his M.D. “I’m here strictly as a volunteer,” Sine says, a recurring refrain among all the adults. (The only exception is ACS liaison Kimberly Dark, a paid employee.) “I’m not here for medical reasons,” Sine continues. “That’s a separate part of my life than this. It’s just nice to see the kids in this environment. We do look for fatigue in the kids that are on therapy. We have to be careful of any exposure to anyone with viruses or colds. Kids on therapy are more susceptible to getting sick from that. Every day they screen both the campers, adults, kids with cancer, and kids that don’t have it.”
“Are there children being treated for leukemia here?”
“Yes, there are. But it’s not necessarily important to know who’s who. It’s really only the camp leaders who need to know who has cancer and who doesn’t. You can see that the kids that are bald or don’t have much hair are on therapy still, but otherwise there are kids here who are cured and been off therapy for years. Sometimes more than that. It’s a place for kids to be kids rather than to be kids with cancer.”
Are there patients of Sine’s among the group here today of (mostly) three- to nine-year-olds?
“Yes, there are a couple as far as in-house, in hospital.”
“How are they doing?”
“They’re doing real well. All the ones here pretty much have to be at a certain level to be able to actually come to camp. The kids that are still on aggressive therapy are in the hospital, and they can’t come to camp. Once they get to a point they call maintenance therapy, where you’ve pretty much treated the cancer in the body and you want to make sure none of it comes back. Those are the kids who would come here. The cancer, for the most part, is out of their body, and you’re keeping it out with chemotherapy.
“These are all outpatients. There are a few kids who have to go into the hospital for three or four days for treatment.”
“Any of them being treated for Hodgkin’s?” I ask.
“I don’t know. You’d have to ask some of the medical staff. Why?”
I mentioned that I had it and that it might be of some help to talk with a child who suffered from that lymphoma. But the medical staff and counselors are protective, and rightly so. Medical case histories are given out sparingly. No one I knew of that day was being treated for Hodgkin’s. I looked for the weight loss, paleness, sweating, nausea, but whatever I saw was just as likely due to the sun, any kind of chemotherapy, prolonged hospitalization, or too much fruit punch and cookies.
Looking around at the kids painting maple and oak leaves with bright tempera paints (later to be imprinted on T-shirts) or swinging plastic whiffle bats the size of small grain silos at plastic balls or listening attentively to the parks-department volunteer lecture on trees, acorns, pine cones, I ask Sine, “Are any of the kids here terminal?”
“I really wouldn’t know that,” he says, but looks as if he does.
My friend Rick in New York, a science-fiction writer with a multiple-book contract he had to deliver pronto, was also diagnosed around the same time as I was. Like me, he had another “good cancer,” “the kind you want to pick if you have to pick one.” These were phrases we had each heard doctors mention.
We compared other stock phrases like “Why did you wait so long?”; “Hope for the best but prepare for the worst”; and “A positive attitude can be of immeasurable value,” which we took to referring to as the “If you eat wheat grass and think good thoughts, who knows?” school of oncological shrugging.
Rick had colon cancer. Giddy with joints (him) and Scotch (me), our conversation went something like this:
“I’m sorry, Rick. That’s really shitty.”
“Bad choice of words. You should have node better.”
“Well, it will all be behind you soon.”
‘'Yes, it’s a bummer.”
“Can’t live forever.”
“June would be nice.”
And Rick used both his cancer and the tremendous pressure to produce an 80,000-word book in an ingenious manner. He wrote one of the strangest psychological urban fantasy novels I’ve ever read. It is called The Feral Cell, and it is brilliant and funny and poignant. It is about cancer.
Meanwhile, I used my time to write another novel that had as little to do with my illness as possible. While Rick used (to borrow Susan Sontag’s phrase) illness as metaphor, I used fiction to get the hell out of the Dodge City of my body and head. Rick saw his body as a canvas, a kind of landscape of conflict against good and evil. I saw mine as an ally turned enemy, pure and simple.
I actually ate wheat grass a few times, but for the first six months of my treatment, I rarely thought good thoughts.
I wept, I got pissed off at everything and everyone, I groveled and whined to a God I wasn’t sure was on the other end of that big white telephone into which I was hurling crackers, rice, potatoes, nitrogen mustard, and procarbazine. I prayed to God as if he were Monty Hall on Let’s Make a Deal.
I went to a curandera in Mexico who rubbed me down with coyote oil, brushed me with fresh-picked sage like a butler grooming the master before the opera. She spat into the base of my neck and wrapped me with a towel while two friends tugged either end as if I were a wishbone. I became blissful at my approach to the edge of this mortal coil and started making mystical pronouncements to my friends and family about meaning, desire, sin, and the mysteries of love. Most of this was a direct result of the Tylenol and codeine I was given to stop the feeling that my upper torso had become something of a sharp, white-hot yoke around my neck.
I did too little laughing, even when my oncologist recommended smoking grass for the nausea (I would merely become paranoid, thinking, Oh, man. I’m stoned and I’ve got cancer). I reacted every possible way a neurotic adult might.
And this is why, eight years after I heard the word “remission” from Doctor Death (as I came to think of him), it occurred to me that children are the teachers here. Adults with cancer should seek out Reach for the Sky and places like them. It’s well and good to rage against the dying of the light, but it might be a better use of one’s time to celebrate it, shadows and all, while it lasts.
Children don’t need to be taught this. They are better poised for the mortal realities of life-threatening illness if for no other reason than they instinctively know two things: It is better to be alive than dead and I’m not dead yet. It’s not dark yet, Mom...let me just finish painting this leaf, let me get from 3rd base to home. I’ll be in in a minute. One more minute...okay?
Justine Fry is eight and a half years old, an enthusiastic singer, conversationalist, and third baseman. Fry’s blond hair never quite fully restored itself after radiation treatments. She has been in remission for years but still looks as if she is undergoing treatment. Except, of course, that she has far more energy than anyone could possibly summon getting nuked with rads, hyped on prednisone, poisoned with nitrogen mustard, procarbazine, or vincristine — whatever.

Justine is dressed in pink shorts and T-shirt. She wears small earrings, and she braces one sneaker against the live oak that serves as third base. She is poised to move fast, retrieve a grounder, or tag out her brother J.J., who seems determined to steal all his bases. In this game the ball is a beach ball and players are just as likely to get thrown out by getting beaned or backsided with the thing as to be tagged.
Justine Fry chases down her runners, even if it means going around all the bases twice, pursuing them into the outfield or well into foul territory. Determination seems to exude from her focused gaze, body language, and steady, confident speaking voice. As the game winds down (evaporates, really, as players wander off for snacks, drinks, games of tag, contemplative nose-picking, the bathroom), Justine Fry has a moment for a post-game interview.
“I was sick for a long time,” she says.
“How long?”
“Um, a year or months or...I don’t know.”
“Do you still have to take medicine or go to the radiation machine?”
She shakes her head “No.”
“Well, good.”
“It was horrible in the hospital.”
“What was the most horrible thing?”
“It was when I went to bed and then they would wake me up in the middle of the night. But my dad was in the hospital in the next bed, and he slept with me every night.”
“Why did they wake you up?”
“Well, my dad would wake me up because I had to get a shot in the middle of the night.”
“Oh, yeah, I had to get those too. Did it make you throw up? That’s what I used to do.”
“No,” she seems to be trying to remember, as if this was something that had escaped her memory. “It was just horrible waking up when I was sleeping, and the needle hurt.”
Indeed, Sine had indicated that the incidence of nausea tended to be much less in child patients. “Children often tolerate chemotherapy better than adults,” he had said.
“See,” Justine explains, “my dad was in the Navy, and he worked in the hospital, so he was actually right next to me. And at home, when I first got sick and had to go to the hospital, they let him ride in the ambulance with me and hold me.”
“Do you know what they called it, what you had?”
“No.” She shakes her sparse corn-silk hair. “It was a long time ago. It started when I was two. And when it was all over, I couldn’t walk or anything. I had to be potty-trained all over again. It was hard.”
Justine Fry was diagnosed six years ago with something called rhabdomyosarcoma. “It was,” says her father, former E4 Naval Corpsman John Fry, “a tumor basically in her temple, behind her left eye and back in her nasal passages. I was in the military at the time. Her oncologist was a Dr. Thomas, now in Washington state. I have to tell you, I owe that guy everything. She’ll have been in remission five years as of this month [August]. We’re gonna throw her a little shindig.

“Yeah, she spent about the first three months after diagnosis in the [Balboa] hospital, and I was working the emergency room. They were nice enough to give me the first month off to be with her; and after that, my wife Laurie would stay with her during the day, and I would have the evenings because I was working anyway. Justine was in and out [of the hospital] for the next year and a half. She got to know everybody there pretty well.”
Laurie Fry remembers the symptoms that led to the ambulance ride her daughter just described. “She had lost a lot of weight over a short period of time, and she was always crabby. She slept 20 hours at a time, and her left pupil dilated abnormally.”
“She had,” recalls John Fry, “about a year and a half of chemo and about six weeks of full head radiation. That’s why the patchy hair; that’s pretty permanent.”
Any other lingering problems?
“Yeah, she lacks a little bit of manual dexterity from some of this stuff. You know, she’s blind in her left eye, so depth perception’s a little tough. The tumor pinched off her optic nerve on that side. She couldn’t see a Jeep; you could blindside her from that side. But she compensates pretty well. She still gets some drainage from her ears and her nose, and so sometimes balance things are a little bit tough for her.”
Justine Fry will be entering the third grade in Oceanside. “She’s a great artist,” says her father, whose critical artistic sensibilities may be exceeded by paternal myopia. “She can sit in her room for hours drawing, cutting stuff up and gluing it together. She’s great.”
Though Justine goes to school all year round, she has been given the week off for Camp Reach for the Sky. She has gone every year since she was three years old. “In fact,” says her father, “you probably shouldn’t tell the Cancer [ACS] people about this, but Dr. Thomas was nice enough to — even when she wasn’t old enough, kind of wrote her a little note and got her in. She gets to go to the resident camp next year.”
According to the American Cancer Society booklet “California Cancer Facts and Figures 1994”:
[Cancer] kills more children age 1 to 14 in the U.S. than any other disease. Among adults it occurs more frequently with advancing age. In the 1980s, it was estimated there were over 470,000 cancer deaths in California, almost 1 million new cancer cases and some 1.3 million people under medical care for cancer.
About 9 million Californians now living will eventually have cancer; about one in three according to present rates. Over the years, cancer will strike in approximately three of four families. Even if incidence rates remain constant, this number of new cases will continue to grow as the California population increases due to migration and the aging of the population.
There are over 776,000 Californians alive today who have a history of cancer, 331,000 can be considered cured, while others still have evidence of cancer. By “cured” it is meant that a patient has no evidence of disease and has the same life expectancy as a person who never had cancer.
The decision as to when a patient may be considered cured is made by the physician after examining the individual patient.
For most forms of cancer, five years without symptoms following treatment is the accepted time. Nevertheless, some patients can be considered cured after one year and others after three years, but some have to be observed much longer than five years.
The smell of damp carpeting to this day nauseates me, can blind me with headaches and panic. Doctor Death (or Dr. Vincristine I sometimes thought of him) had his office on the second floor of a building on Fourth Avenue near Mercy Hospital. I would take the stairs because I would always run into really sick-looking people in the elevators. The problem was, the carpeted stairway always smelled of mildew and disinfectant. Ascending the stairs on my way to intravenous chemo sessions, my stomach would churn with the anticipated hours of vomiting. The association between the smell of mildew and Pine-Sol and sickness and death remains with me still.
The first time I heard the word “remission” was within a week of my visit to the curandera. I am not suggesting there is any causality here, only synchronicity. And it is not the proximity of these two events that I found disconcerting or puzzling, it was, rather, Now what? I’ve spent a year rehearsing for the Big Sleep and it looks like I’m going to live after all. How do I do that? This is unfair. They've changed the rules on me. Doctor Death, now Doctor Get-a-Life, grinned toothily at me and extended his hand for me to shake. “Congratulations!” he said as I took his hand and smiled back as life-affirmingly as I could. “Welcome to maintenance therapy!” he said.

Fifteen-year-old Leo Coburn is making a flying saucer out of a plastic coffee-can lid and a Styrofoam dome decorated with paste-on stars and felt-tip pen markings. David Sine sits quietly at the corner of the long folding table, and Coburn demonstrates his construction to the mellow, almost sleepy-looking doctor and volunteer counselor. Briten and Kirsten Douglas, two seraphic blond sisters aged, respectively, seven and nine, are immersed in a crafts project with these same components. A half dozen other children are engaged in their own versions of similar activities, and though Sine elicits no explanation from the children as to just what it is they think they’re making, many of the campers give running progress reports to “Maple Leaf” (Sine’s button), elaborate descriptions of their creations (snowmen, igloos), comments on the difficulty and technique involved in getting the Styrofoam to take the felt-tip ink. Sine smiles, approves, and expresses an even interest: “Is that what that is?” His responses and attention, his slow smile seem to reassure the children that Sine doesn’t feel left out.
“It’s a flying saucer!” announces Coburn. He has to repeat himself a few times; his enunciation is sometimes unfocused.
“Hey, that turned out neat, didn’t it?” Sine looks pleased. “Try to throw it. See if it’ll fly.”
“Not inside,” Coburn corrects Sine. “Outside. In space.” Coburn tosses his saucer off the front porch of the scout lodge. It tumbles a few feet and lies in the grass at the foot of the steps. Coburn smiles up at Sine as if he had just demonstrated an interesting new example of Newtonian physics. Sine nods his head with appropriate approval.
“Briten was diagnosed with leukemia March 10 of ’91,” says Corinna Douglas, Briten’s mother. “She just finished her three-year protocol at the end of this last year. The day before Christmas she got her Hickman out.” The Hickman is the catheter implanted in the skin, usually the chest, to facilitate IV treatment. It precludes the necessity to constantly puncture the skin during treatment.
“The chemotherapy is completed,” says Douglas. “She is now in this surveillance phase, where the doctors don’t give you any real vote of confidence. We’re in that critical year to see how she does off chemo. The thing she has going for her is that she has responded to the chemotherapy and has stayed in remission for almost three years. Now to hold on to it is what we’re all hoping for.”
“So another 18 months or so and she’ll be out of the woods?”
I ask.
“Well, they never say that. They never say that you are out of the woods.” Douglas sounds tired, a little frustrated. “Only that she’s in remission and what her survival hopes are. But three years ago I could never have imagined being where I am now. It was just unforeseen that we could have possibly come out of this.”
At any point did Douglas resign herself to losing her daughter?
She answers carefully. “I was...resigned...in the sense of preparing for the worst, but hoping for the best.” That phrase again. I could never decide if it was a Zen koan or just double-talk.
“Briten was born with bladder atrophy, that is, she was born without a bladder and without a pelvis. When she was four hours old, she had seven and a half hours of reconstructive surgery. At that point in time, they told us there was a good chance she was not going to make it, but that if she does, she’s going to have a very compromised life. ‘She may never walk,’ they said. ‘And if she does walk, we don’t know the significant problems she will have.’ So we figured, this is the way her life is gonna go. At the time, I already had a 22-month-old baby at home.
“That preparation helped us to deal with the next phase,” Douglas continues, “which was her [Briten’s] diagnosis with cancer by the time she turned four. But if you recall what Briten looked like [the previous week at the camp], you wouldn’t know. I mean, the resilience of that kid!”
Indeed, Briten Douglas appears as healthy as any seven-year-old one might point to. Yet Douglas laughs, “She’s had us on an emotional roller coaster from the first day she was with us.”
How did Briten’s symptoms of leukemia announce themselves?

“She woke up in the middle of the night and came into our room and said she had a knife in her stomach, ‘Take me to the doctor to get the knife out.’ We were thinking it had something to do with her other problems. I couldn’t call a pediatrician up in the middle of the night and say, ‘My baby has a stomachache.’ I just told her to go to the bathroom. We were trying to treat things normally. But her earnest comment, ‘Take me to the doctor now’ prompted us to call. Our pediatrician happened to be on call at the time at our hospital here in Escondido. He took a blood, test, and since he was in the oncology field, he knew immediately that 69 percent of her was cancerous blast cells. Leukemia is basically an overproduction of white blood cells.”
The ACS “California Facts and Figures 1994,” under Major Cancer Sites, Leukemia, states, “There has been dramatic improvement in the outcome of acute childhood leukemia. The majority of children are cured and live into adulthood leading normal lives.” This, according to tables included in the booklet, is a 30 percent improvement in survival figures in as many years.
“We are just in that transition now,” says Corinna Douglas, “where we’re finally past the throwing up and the painful treatments and the dressing changes for the hip, and her hair has finally all grown back. She still has to have spinal taps every three months because, for some reason, the relapses they are seeing occur in the bone marrow even if it was not previously cancerous.”
What was Briten’s sister Kirsten’s reaction to the years of illness?
“The roller coaster on that was very, very tough. She had a very difficult time because we had to ship her to anyone we could at times. We don’t have that many family members that could support us here in California because most of our family is on the East Coast. It came down to my husband and myself — one of us being at the hospital and one of us trying to get Kirsten squared away. Dad needed to be in the hospital with Briten as much as I needed to be there. The message to Kirsten was, ‘You’re the well one. You have to stay strong.’
“It was hard on her because she would have to endure a lot of different households and uncertainties. She would go to kindergarten with a suitcase and a note telling her teacher so-and-so is going to pick her up. We had to rely on a lot of people coming out of the woodwork to help us out. She is now nine, and she still does not appreciate having to spend the night away anywhere. She has this phobia. It’s really hard to imagine that a kindergartner would want to kill herself, but Kirsten really, really did want to kill herself.”
How long did this go on?
“That lasted a good portion of the first year Briten was in the hospital. She was very, very worried about her sister, worried about us. She had grown up seeing her sister in this medical world. She had to wonder, ‘When will this stop? When will I get to be the focus?’
“I have now come to realize,” says Douglas, “that children that are presented these challenges in life are much brighter than you ever could imagine. They can handle it. Briten was very courageous; she knew she had to fight the fight. And in that battle, over the years she has witnessed friends — within the treatment room and the hospital — dying. And then attending their funerals.”
Waiting at poolside with lifeguard Paula “Boom-Boom” Ferraco, ACS liaison Kimberly Dark, assistant unit leader Susan “Beanie” Bean, and various other adults and children such as Shyloh Zurn and Leo Coburn’s nephew Chris Gray. Michael Nava dangles his feet in the water while Beanie plays drowning victim and “Boom-Boom” gives instructions on water safety.
In a demonstration involving a drowning victim (the dramatic Beanie — “Help! Help! Oh, my!”) being rescued by poolside buddy Leo Coburn (who lies prostrate at the edge of the pool to minimize danger of being pulled in along with the victim), rescuer Coburn points out the alternative lesson that it is possibly more fun to allow oneself to be pulled into the pool by a hammy actor than to go along with the fake lifesaving gag. Mike Nava warns several kids against a dive-bombing beetle and is wary when it is explained to him they cannot hurt you, “How do you know?” he asks suspiciously.
When fellow camper John Baxter (excellent batting stance but unenthusiastic interview subject) asks Nava what his Hickman catheter covered in waterproof tape is for, Nava answers, “For what they do to me, they poke hard. This is so I don’t get pokes on my arm.” He points out the scar on his stomach again and the staple marks. He announces proudly, “When they took ’em out, it didn’t hurt. I didn’t use the sleepy medicine, I didn’t use the not-feeling medicine or nothing. My brother Tony has a Walkman and a boom box and the Michael Jackson Thriller CD.”
Nava swims with the best of them and gives impromptu math tests to his companions, who are less than appreciative of Nava’s excellence in this area. He looks like a child as full of life and health, humor, and awe as could be asked for. He is merely bald and has plastic straws surgically implanted in his chest cavity and has a tumor in his liver.
Nava has gone through five types of chemo treatment in the past two years. He is currently undergoing a course of treatment known as I.C.E., which stands for the chemical names of the poisons he is given. I.C.E. is a particularly brutal chemical course and is something of a last resort for Nava’s parents, because Nava’s case is one in a hundred, and oncologists get few opportunities to study cancers like his. Nava’s mother’s attitude is “Whatever it takes.” Nava’s scar is a result of exploratory surgery that revealed the tumor to be inoperable. The six-year-old is on a “nonactive” waiting list for a liver donor. Last September, around Michael’s birthday, he relapsed, and so the course of chemotherapy had to be altered again. The Make-a-Wish Foundation rose to the occasion and raised $1900 for Michael and arranged a trip for him to Disneyworld, where Nava could cruise the gift shops and “pick out anything he wanted,” his mother says.

“He would just point to whatever and say, ‘I’ll have one of those and one of those.’ Now Michael thinks the Make-a-Wish Foundation is this kind of genie. This year for his birthday he wants the foundation to arrange for him to legally change his name from Michael Nava to Michael Jackson.”
What are the doctors saying about Nava’s prognosis, his chances, his future?
Mrs. Nava pauses, sighs. “No one really knows.”
In mid-September Gloria Nava called to say that Michael’s I.C.E. treatment was no longer working. “The doctors told me there was nothing more they could do. They told me it was a matter of weeks or a month.” One of Nava’s oncologists did suggest a last-ditch effort involving the experimental drug topotecan, a natural extract from tree bark. Nava is currently undergoing treatment involving this drug under the supervision of Dr. Alice Yu, professor of pediatrics at UCSD Medical School. Of the treatment, Yu said only, “We know very little about it. It is very experimental.”
When asked to comment by phone, the seven-year-old patient was playing a video game and said only, “Not now. I’ve got to concentrate.”
Comments