 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube

A report by state auditor Elaine Howle released December 20 blames both city and county for the severity of last year's deadly Hepatitis A breakout in downtown San Diego, with lack of accountability by local officials responsible for the mounting death toll.
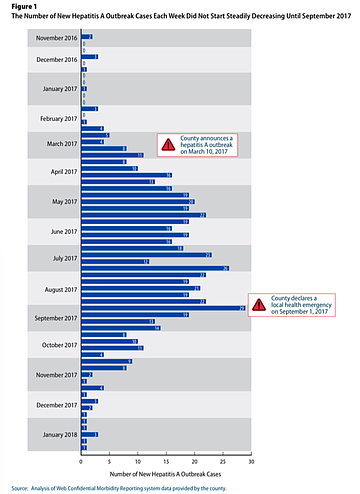
"Despite discussions in June and August 2017, the county and city did not fully implement the measures related to hand‐washing stations, restroom access, and street sanitizing until September 2017—after the county’s local health officer issued a directive telling the city it had to take action on the sanitation measures," says the audit.
"The county health officer did not issue a directive sooner because she wanted to collaborate with the city instead of mandating its compliance. However, by exercising her legal authority before August 31, 2017, the county health officer likely would have prompted the city to implement the important sanitation measures sooner.
"Additionally, the county did not share location data to inform the city about the concentration of the cases within its jurisdiction until November 2017. If the city had had more information, it might have more quickly understood the need for the sanitation measures."
During the early stages of the epidemic, chaos reigned as city officials pointed the finger of blame at the county. "We expected the city to have taken some additional steps to understand the actions needed related to sanitation to protect the public health of the at‐risk populations, such as requesting updates from the county regarding the response and coordinating any of its own sanitation efforts with the county.
"However, according to the assistant chief operating officer, the city expected the county to manage the outbreak and provide the city direction on what was required or necessary. Based on discussions it had with the county, the city believed that it was adequately responding to the county’s requests; thus, it did not see a need at the time to take additional action."
The state audit notes that a post-crisis internal analysis by San Diego city officials omitted relevant details of the bureaucratic runup to the meltdown. "The report stated that its purpose was to analyze the city’s response to an incident and that it identified 12 issues or areas for improvement. However, because the report covered only the time during which the local health emergency was in effect—September 2017 to January 2018—it did not identify any areas for improvement related to the implementation of sanitation measures before the declaration."
"By not also assessing its actions before the local health emergency declaration, the city missed an opportunity to identify issues that may have contributed to delays in the implementation of sanitation measures and to develop steps to address these issues in the future."
The audit additionally questions the county's delayed response, criticizing its failure to boost vaccination rates during the crisis. "We believe the county did not accelerate its vaccination efforts to address the hepatitis A outbreak because it lacked a strong sense of urgency. Its failure to hire additional temporary nurses in a timely manner is symptomatic of this lack of urgency."
"Even though internal county meeting agendas from April 2017 through June 2017 indicate that the county discussed acquiring extra nurses to administer vaccinations, it did not initiate the procurement process to hire additional nurses until July 2017. Instead, the county responded to the early months of the outbreak by relying on its own nursing staff, soliciting vaccination assistance from certain community clinics and health care providers, and using its existing contract for temporary staff."
"As a result, the county did not accelerate vaccination efforts until September and October 2017. Had the county hastened its vaccination efforts, it may have more quickly reduced the risk of the disease’s spread, which grew to include 584 reported hepatitis A cases, 398 hospitalizations and 20 deaths by the end of January 2018."
The audit recommends improved documentation of the responsibilities of city and county officials during public health emergencies. "To ensure that it takes appropriate action to protect the public health of the residents of the city, the county should enter into an agreement—such as a memorandum of understanding—with the city or should negotiate revisions in its contract with the city by March 31, 2019, to clarify each entity’s roles and responsibilities over public health matters, and to include city leadership in coordinating response efforts when public health matters, such as disease outbreaks, affect the city’s residents."
In their respective responses, the city and county said they would adopt the audit's recommended remedies by the deadline.


A report by state auditor Elaine Howle released December 20 blames both city and county for the severity of last year's deadly Hepatitis A breakout in downtown San Diego, with lack of accountability by local officials responsible for the mounting death toll.

"Despite discussions in June and August 2017, the county and city did not fully implement the measures related to hand‐washing stations, restroom access, and street sanitizing until September 2017—after the county’s local health officer issued a directive telling the city it had to take action on the sanitation measures," says the audit.
"The county health officer did not issue a directive sooner because she wanted to collaborate with the city instead of mandating its compliance. However, by exercising her legal authority before August 31, 2017, the county health officer likely would have prompted the city to implement the important sanitation measures sooner.
"Additionally, the county did not share location data to inform the city about the concentration of the cases within its jurisdiction until November 2017. If the city had had more information, it might have more quickly understood the need for the sanitation measures."
During the early stages of the epidemic, chaos reigned as city officials pointed the finger of blame at the county. "We expected the city to have taken some additional steps to understand the actions needed related to sanitation to protect the public health of the at‐risk populations, such as requesting updates from the county regarding the response and coordinating any of its own sanitation efforts with the county.
"However, according to the assistant chief operating officer, the city expected the county to manage the outbreak and provide the city direction on what was required or necessary. Based on discussions it had with the county, the city believed that it was adequately responding to the county’s requests; thus, it did not see a need at the time to take additional action."
The state audit notes that a post-crisis internal analysis by San Diego city officials omitted relevant details of the bureaucratic runup to the meltdown. "The report stated that its purpose was to analyze the city’s response to an incident and that it identified 12 issues or areas for improvement. However, because the report covered only the time during which the local health emergency was in effect—September 2017 to January 2018—it did not identify any areas for improvement related to the implementation of sanitation measures before the declaration."
"By not also assessing its actions before the local health emergency declaration, the city missed an opportunity to identify issues that may have contributed to delays in the implementation of sanitation measures and to develop steps to address these issues in the future."
The audit additionally questions the county's delayed response, criticizing its failure to boost vaccination rates during the crisis. "We believe the county did not accelerate its vaccination efforts to address the hepatitis A outbreak because it lacked a strong sense of urgency. Its failure to hire additional temporary nurses in a timely manner is symptomatic of this lack of urgency."
"Even though internal county meeting agendas from April 2017 through June 2017 indicate that the county discussed acquiring extra nurses to administer vaccinations, it did not initiate the procurement process to hire additional nurses until July 2017. Instead, the county responded to the early months of the outbreak by relying on its own nursing staff, soliciting vaccination assistance from certain community clinics and health care providers, and using its existing contract for temporary staff."
"As a result, the county did not accelerate vaccination efforts until September and October 2017. Had the county hastened its vaccination efforts, it may have more quickly reduced the risk of the disease’s spread, which grew to include 584 reported hepatitis A cases, 398 hospitalizations and 20 deaths by the end of January 2018."
The audit recommends improved documentation of the responsibilities of city and county officials during public health emergencies. "To ensure that it takes appropriate action to protect the public health of the residents of the city, the county should enter into an agreement—such as a memorandum of understanding—with the city or should negotiate revisions in its contract with the city by March 31, 2019, to clarify each entity’s roles and responsibilities over public health matters, and to include city leadership in coordinating response efforts when public health matters, such as disease outbreaks, affect the city’s residents."
In their respective responses, the city and county said they would adopt the audit's recommended remedies by the deadline.
Comments