 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube
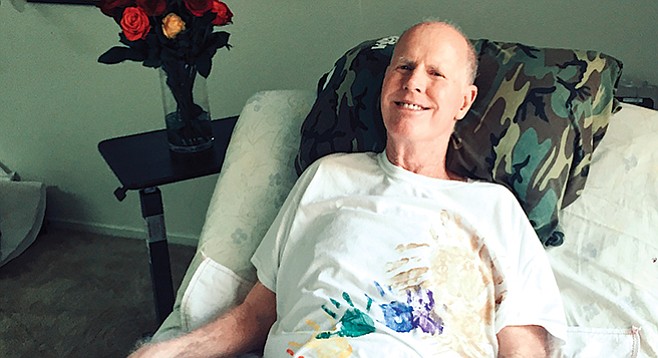
On the afternoon of October 23rd, in the presence of his family, trailblazing San Diego surfer Bill Andrews ingested medication prescribed to end his life. Within a few minutes the 73-year-old had fallen asleep, and over the next quarter hour his breathing slowed, gradually, until it stopped altogether.

Andrews is often credited as the first to surf the celebrated waves of La Jolla’s Black’s Beach, and a photograph of him doing so appeared on a 1965 cover of Surfer magazine. By all accounts, Bill Andrews enjoyed a vigorous life as an action sports enthusiast, entrepreneur, engineer, photographer, father, and grandfather.
However, in 2016 he was diagnosed with amyotrophic lateral sclerosis, more commonly known as ALS, or Lou Gehrig’s disease. The neurodegenerative disorder destroys nerve cells.

Those afflicted with the disease become progressively paralyzed to the point they can no longer walk, move their fingers, speak, swallow, or, eventually, breathe. While the disease advances at different rates for different people, there is no cure. Despite outlier cases such as Stephen Hawking — who recently passed at 76, after 55 years enduring a variant of ALS — it’s roundly considered a terminal diagnosis, with as little as two year life expectancy.

For Andrews, the symptoms progressed rapidly, his loss of motor function compounded by acute pain due to a lifetime of broken bones and other sporting injuries. Facing paralysis and suffering in the imminent future, Andrews chose instead to schedule the end of his own life, with the assistance of a physician.
After decades of controversy and public debate, the legal ability to do so has been available in California since mid-2016. Advocates have used several names to describe it: physician assisted suicide, medical aid in dying, death with dignity, the right to die.

Whatever the terms used, the California Department of Public Health reports 191 people acquired prescriptions to end their lives in the last seven months of 2016. At least 111 are confirmed to have taken the medication and perished.

But it’s still a new practice, and most of what we know about how the law is being put into practice is anecdotal. Just like the unsettled vocabulary involved in taking a prescription to take one’s life, the ways it’s being applied, both from a business perspective and a cultural standpoint, are starting to come into focus.

The End of Life Option Act became California law in June 2016 when it was passed by the state legislature and signed by Governor Jerry Brown. It states that a patient diagnosed with a terminal illness may request life ending medication from a licensed medical doctor. But due to the controversial nature of the law, it’s loaded with safeguards against patient abuses.

First of all, the patient must be deemed of sound mind, and not expected to survive a specified illness for more than six months. The patient must first make an oral request for life-ending care to his or her attending physician — alone; that is, without any loved ones or caregivers present to exert influence or duress. The physician must make the patient aware of all alternative treatment options, including hospice care. After a mandatory 15-day waiting period, a second oral request must be made under the same conditions, followed by a written request, signed in the presence of two witnesses.

The patient must also consult with a second physician to confirm the terminal diagnosis, and independently corroborate the patient’s mental state. Due to the soundness-of-mind requirement, Alzheimer’s patients or anyone affected by dementia are disqualified.
Once the medication is secured, a patient must ingest it him- or herself. The preferred prescription, used by Bill Andrews, is for a controlled overdose of the barbiturate seconal, a powerful sleeping agent. One hundred capsules are prepared into a liquid solution for the patient to drink.
A doctor cannot pour it down a patient’s throat, nor a family member. In some cases, the end of life option may boil down to whether a person can suck the medication down a straw and swallow it. At any time, even at the last moment, a patient may simply decide not to take the medication, choose to take it later, or simply keep the medication on hand while allowing a disease to take its course.
A few days prior to taking his fatal last drink, Bill Andrews frankly discussed his illness, and his decision to die on a podcast recorded by his doctor. “Just a year and a half ago I was in Peru surfing,” he said from inside his room at a San Marcos assisted living facility. By contrast, he characterized his present-day life as “horrible” and sedentary. “I get fed. I wear diapers. I’m kind of confined to my bed.”
With the support of his family, he planned how his death would go. “The thing that’s the most incredible thing to me,” Andrews said, “is being able to choose when you’re going to die… I’m choosing the time. I’m choosing the place. I’m choosing the environment. I’m choosing the company. And for me…” he added, “I can’t think of anything better.”
The avid surfer, motorcycle racer, and adventure traveler would find a gentle, painless end, surrounded by people he loved, having said his last goodbyes and tied up all his loose ends. “I’ve kind of been a pioneer in a lot of things,” he told his doctor on the podcast, explaining why he decided go public with his story. “I think this can do a lot of good.”
The doctor assisting Bill Andrews with his death was Bob Uslander, known to his patients as Dr. Bob.
Uslander established his practice, Integrated MD Care, in early 2016. Its primary purpose — then and now — is to provide in-home palliative care. Hospice. “The vast majority of what we do is take care of people in their homes,” he says. Some of his patients aren’t dying, rather they’re enduring prolonged recoveries from serious illness or injury. “A lot of our patients are older, they have dementia. Or they’re just frail, and they need someone to be there to take care of them.”
However, by the time Bill Andrews first approached him, Uslander had already been gaining a reputation as San Diego’s go-to primary physician for people seeking medical aid in dying. Uslander has helped dozens of patients gain access to life-ending medication — far more than any other local doctor. He’s traveled to assist patients in Orange County, Los Angeles, Riverside, Palm Springs, and Oakland. In the process, he has become one of the law’s most visible advocates.
He didn’t set out to be. Focused on starting his new practice when Jerry Brown signed the law, Uslander says he took note of it as an advancement of civil rights, but didn’t think of it as something that would impact him so significantly. “I thought it was a good move,” he says. “Progress. And that once the law went into effect, that doctors would be willing to help their patients.”
However, that has not been the case. Most medical professionals in San Diego have shied away from offering aid in dying to their patients, or referring patients to a doctor who will.
“It was really surprising to me when people started calling me,” recalls Uslander, “saying I can’t find anyone to help me. My own doctor won’t do it, my specialist won’t do it. And some of these people had called 10, 25 physicians, or more. And each time, they got denied.”
By law, health care providers are not required to offer medical aid in dying, and organizations such as hospitals or medical practices may prohibit doctors they employ from doing so. While statutes protect physicians from criminal, civil, and professional liability when they operate within the constraints of the law, a presumed risk to reputation proves enough to make many hesitate.
“It has a big impact, and we know it’s controversial,” confirms Uslander “It’s a service that I would be okay not providing if doctors would step up and take care of people adequately, but that’s not happening. I feel like, if I’m not doing it, there’s way too many people who are going to struggle, and have bad deaths.”
In November, Uslander launched the podcast, “A Life & Death Conversation.” It covers topics ranging from dealing with suicidal thoughts to coping with grief, and a lot of its episodes serve to bring the aid in dying topic into the public sphere, explaining the concept of a good death.
The doctor has found families have an easier time addressing end-of -life options when they can hear about how peaceful the process can be. Following Bill Andrews’s appearance, his three sons returned to record a follow up interview, describing the life-affirming experience his family shared on the day of his death, and the days leading up to it. According to one of his sons, Andrews described his last three to five days as “the most peaceful time of his life.”
Subsequent episodes have featured aid in dying advocates, a grief counselor, a hospice worker, and a doctor from the Netherlands speaking by phone to discuss his experience with euthanasia. The practice has been legal there since 2002, and today reportedly accounts for 4.5 percent of that nation’s deaths.
Uslander the podcast host is a stickler for the language we use to describe it. He avoids terms that carry negative connotations. For example, he points out that, in California, physician assisted suicide is not euthanasia. Officially, it’s not even suicide.
“Euthanasia is active,” he says, “It’s a physician actively ending a person’s life, at their request,” while the End of Life Option Act requires life-ending medication to be self-administered. Meanwhile, to ensure life insurance policies cannot deny benefits to patients who use the law, it clearly states that the patient’s death certificate should name the terminal diagnosis as cause of death. It may be cancer, ALS, heart disease, but never suicide.
A doctor is not required to be present, however most of Uslander’s patients have invited him to take part in their final moments, both for emotional support, and to ensure the medicine is administered properly. The moments he’s witnessed have reinforced to him the positive impact of the new law, and the value of a good death.
“Sometimes the last words they utter are directed at me,” he reveals, “It’s usually something like, ‘Thank you. Thank you for being there.’”
The patient’s family members often echo the sentiment. While he finds it gratifying to hear, Uslander tries to keep such praise in perspective. “It’s not fair,” he says, “I’m held in this light, as the person who stepped in to give them this final gift, when no one else would.”
While opponents of aid in dying have long argued that family members and care workers would coerce patients into physician assisted death for their own financial gain, Uslander’s experience has thus far shown otherwise. “There’s never been one incident that has smacked of that,” he says, “It’s kind of been the opposite.” Patients have been the ones convincing families to accept their decision to die.
Uslander tells the story of a woman in her late 90s who had a hard time getting her children and grandchildren to accept her plan. “There was a lot of misinformation and fear about what was going to happen,” he says, “But once they understood what the process is, and how peaceful it usually is, then they came around to supporting her.”
When the time came, the woman gathered her extended family around her for two days of remembrances and farewells. Then, with children, grandchildren, nieces, and nephews there to support her, she drank the medication, and fell asleep. “As soon as she stopped breathing and died,” Uslander recalls, “everybody stood up and gave her a standing ovation.”
In the August 2016 Voice of San Diego story “What I Learned Helping My Sister Use California’s New Law to End Her Life,” Kelly Davis documented the death of her sister, Betsy, who was in the advanced stages of ALS when, that July, she chose to be among the first in the state to legally ingest life-ending medication prescribed by her doctor.
The story, which received national attention, depicted an emotionally charged end-of-life celebration, wherein Betsy Davis invited friends and family to join her for a two-day gathering of drinks, music, and fashion that culminated with her falling asleep for the last time during an Ojai sunset.
Kelly ultimately helped Betsy realize her end of life vision, though she shares via email that her first instinct was to try to keep her sister alive. “Of course I didn’t want her to die, ever,” she writes. “I was constantly looking for some miracle cure, pestering her ALS doctor about clinical trials.”
However, during a visit several weeks prior to Betsy’s death, an ordinary moment brought a shift in Kelly’s perspective. “She wanted to take a nap, so I left the room,” Davis remembers. “A few minutes later, she called for me to come back to her room. She couldn’t sleep because she had an itch above her eyebrow that was driving her crazy and couldn’t reach it, so I scratched it for her. I left her room thinking about how, if I hadn’t been there, she would have been lying there, just in agony. Even though I’d seen how much she’d suffered in the three years since her diagnosis, there was something about that moment that really struck me and made me realize how much her quality of life had diminished and it was selfish of me to not be OK with her decision.”
Betsy Davis was not alone in wanting to be present for an end-of-life celebration to help herself and her loved ones to let go. On Uslander’s podcast, Bill Andrews’ sons tell how the surfer’s 95-year-old mother performed a hula song she had written for him, as the family gathered around him for the last time. Uslander tells of another patient who gathered friends so he could break out a bottle of scotch he’d been saving for a special occasion, to share one last drink before taking his medication.
Uslander says most of his patients don’t try to turn the moment into an event. Many are already suffering, and simply wish to get it over with. A number of his patients haven’t survived the 15-day waiting period required by the law.
However, others have created personal rituals, ranging from the reading of Bible verses, to the ringing of Buddhist bells. For the most part, they’ve been ad hoc rituals. While we have established norms for funerals, we don’t have practiced customs for commemorating a person’s death while it’s happening. In some cases, people embrace the opportunity to effectively be present at their own funerals.
Melissa Rainey operates a business called Eternally Loved, which offers memorial event planning. She started the work after a close friend died, and she saw the value it provided the family when she stepped in to make funeral arrangements as they grieved.
Recently, Rainey’s begun planning what she’s calling living memorials: arranging events for terminally ill patients. She tells that one of these clients had scheduled her fete ahead of her own physician-assisted death, opting for an elaborate send off.
The woman had a great sense of humor, and had Rainey book a stand-up comedian to emcee the party, introducing loved ones to deliver eulogies. “It broke the ice, and it also created an atmosphere of joy,” recalls Rainey, who also brought in therapy dogs, for people to pet in case someone was having a hard time.” And she had the party catered with the woman’s favorite foods, including Chinese food, donuts, Jewish deli, and In-N-Out Burger.
Historically, the Hemlock Society of San Diego has been the leading local advocate for this cause. The 31-year-old organization has advocated for terminal patients’ right to die, led by Harvard trained forensic psychologist, Faye Girsch, who founded the local chapter in 1987, and eventually served as president of its national, parent organization. After that group merged with another to form a new entity, Compassion & Choices, Girsch split off Hemlock Society of San Diego as an independent organization.
Girsch became involved in the right-to-die movement while working with the American Civil Liberties Union in 1983, on the nationally publicized case of onetime San Diego State student Elizabeth Bouvia, a quadriplegic who filed an injunction against a hospital for keeping her alive against her wishes.
“She wanted to die by refusing food and hydration, which you could not do at the time,” recalls Girsch, “So she admitted herself to Riverside Hospital, and they were force feeding her.” Girsch was tasked with evaluating Bouvia’s state of mind, and found her to be competent. Bouvia lost the case.
However, the circumstances inspired Girsch to lobby for changes to health policy, including working to help put Proposition 161, the “Aid in dying act” on the California ballot in 1992.
While the nonprofit Hemlock Society celebrated the passage of the End of Life Options Act, it continues to advocate expanding the law to include a wider range of patients. For example, while Girsch actually opposes capital punishment, she supports lethal injection being added to the end-of-life option, as Canada’s national health care policy allows. This would extend the right to die to someone unable to swallow medication.
Uslander tells of such a patient at his practice, who opted to have an endogastric tube inserted so he could push the lethal prescription into his stomach with a large syringe. With a progressive disease such as ALS, had that patient lost use of his hands before having a chance to take the medication, he would not be able to access the California law.
It’s one reason the Hemlock Society also finds the 15-day waiting period problematic. It’s included to give patients a chance to change their minds, and Uslander reports that a significant number of his patients do so — either during the waiting period, or after they’ve received the medication.
However, he’s also seen patients perish while waiting for a prescription. Some of these patients experienced what he calls “a bad death,” knowing how close they’d come to the peaceful one they’d been seeking. Some may have received the medication in time, if they’d found a doctor sooner.
So, the Hemlock Society has been working to compile a list of local doctors willing to support medical aid in dying. Thus far, it’s a short list, with Dr. Bob at the top of it. “We’ve being doing this now for a year,” says Girsch, “calling doctors and hospices, seeing whether they will participate or not. And generally, it’s not.”
“Nobody wants to be Dr. Kevorkian,” suggests Charese Brooker, the Hemlock Society’s executive director.
She’s referring to the controversial physician-assisted-suicide activist who made headlines in the 1990s for helping 130 terminal patients end their lives, then wound up in prison for eight years on a second degree murder conviction. While the California laws offers copious legal protections for practitioners, Kevorkian’s legacy includes the fear of reprisal for doctors helping patients die.
Brooker is a registered nurse who’s spent most of her nine year career working in hospice, and has seen the challenges terminal patients face in finding willing physicians. “Even though we now have the act in place,” Brooker says, “we’re seeing a lot of people having trouble accessing it… It’s hard to find a doctor. And then it’s hard to find a second one.” For a patient with terminal illness, she adds, “It’s very cumbersome and very draining.”
Compassionate Choices has been keeping track of whether local hospitals and hospices allow their doctors to serve as attending or consulting physicians, and post the information to a searchable web page. Organizations affiliated with the Catholic church and other religious organizations don’t allow doctors to participate. Neither does VA health care, which is subject to federal law. Even organizations that do offer aid in dying as a policy — such as Sharp HealthCare and Kaiser Permanente —don’t widely advertise the service. There’s little or no acknowledgement of the End of Life Option Act on their web sites, and phone inquiries receive limited or no response.
“What you’ll end up finding is people won’t talk to you,” Brooker says, “They’ll send you on this wild goose chase.”
Even when organization hierarchies aren’t an issue, individual doctors are free to opt out, and often do. Aid in dying advocates contend many, if not most, doctors do not bring up the medical aid in dying option with their terminal patients: particularly oncologists, neurologists, and other specialists who treat most of the patients who qualify. Even if they’re willing to assume the responsibility, they don’t advertise the fact.
“Unless they already have a relationship with the patient, they’re not going out and making it known that they’re doing this,” says Uslander. Publicly, he says, “I’m the only one who’s willing to take on patients.”
Uslander reports patients come to him saying their doctor refused to discuss it, or their hospice disallowed it. Others say their doctors agreed to do it, and even initiated the process, then changed their minds during the mandated 15-day waiting period, forcing the patient to start over. In some instances, the doctor agreed to serve as the consulting physician required by the EOLOA, but not as the attending.
“People are more willing to be the consulting physician, in my experience, than the primary physician,” says Brooker. “A lot of times, what we’re finding is they refer to Dr. Bob.”
According to California’s statistics, 84 percent of those seeking physician assisted death are enrolled in hospice care, which is no coincidence. The six-month terminal diagnosis required by the law is the same term established to receive hospice benefits.
Brooker proposes that hospices are unwilling to administer the option because some people still find a stigma attached to hospice itself. “People think, I’m going to go to hospice and you’re going to kill me.” In response, she says, “hospice has for a long time pushed that idea away.” Like hospitals, they’re reticent to market or discuss their aid in dying policies.
Hospices have at times been accused of rushing patients to death, and other times accused of keeping them alive longer to increase profits. Instances of fraud, such as the highly publicized case of San Diego Hospice allegedly misreporting patient information in 2012, have kept such suspicions alive. As a result, hospices have reaffirmed the credo that they “neither hasten nor postpone death,” which they can’t be seen to do if they publicly offer aid in dying.
However, a relatively noncontroversial practice that routinely takes place in hospices, and hospitals, is palliative sedation. Also known as terminal sedation, it’s what happens once a patient effectively experiences too much pain to remain awake. When the dose of morphine required to make them comfortable, also renders them unconscious.
Palliative sedation is often simply the inevitable end of palliative care; sometimes it’s a conscious decision, oftentimes it’s a circumstance that commences gradually, to the point that reviving a patient to the pain of consciousness would be objectively cruel. In these cases, a terminal patient may linger in this terminal morphine state for days or weeks.
But in Brooker’s experience working in hospices in the Midwest, where aid in dying is not legally available, patients would commonly ask for an end to life by this means, sometimes directly.
“I would have people all the time ask me,” she reports, “Would you kill me? Or, Would you give me that magic dose?”
To Brooker, medical aid in dying offers a more humane alternative. “Terminal sedation has always hit me the wrong way,” she says. “If we’re going to palliate someone so much that they’re in a coma… then what’s the point?”
There’s one point for patients of limited financial means: hospice is affordable. It’s been covered by Medicare since 1982. The end of life option is not.
Bob Uslander reports his aid in dying patients have ranged in age from early 40s to 106 years old, but are usually between 70 and 90. They tend to be college educated, with a high number of them professionals: doctors, lawyers, college professors. More than half have been men, though not by much. The overwhelming majority have been white.
While the sample sizes are too small to draw any concrete conclusions, these demographics roughly match the first set of data reported by the Department of Public Health.
In a nutshell, those who can access medical aid in dying must also be able to afford it. A prescription for seconal costs about $3500. An alternative mix of medications has shown to be effective for about $800 — Betsy Davis used it — but Uslander says it can take longer to work, hours potentially, and patients may gasp or twitch, which can be distressing to families.
Meanwhile, Integrated MD Care is a boutique palliative care provider employing specialists who provide treatments such as physical therapy, massage therapy, acupuncture, music therapy, and cannabis treatment, in addition to traditional nursing care. Uslander’s time does not come cheap.
“I’m not working with insurance, so [patients are] paying me a fee,” he says. He doesn’t share exact numbers — “My fee ranges from zero to something,” he says — but he has worked pro bono. “I have the ability to take care of people without charging them, which I do on occasion.”
However, free care is not sustainable for his business, so Uslander has taken steps to launch the Integrated Lifecare Foundation, a 501(c)(3) nonprofit that will raise funds to support providing patients with lower economic means access to the palliative services Integrated MD Care offers, including medical aid in dying.
“The one aspect that is uncomfortable for all of us at IMDC is that people without some financial means will not benefit from what we can offer,” explains Uslander.
In addition, he has been asked to offer training sessions to local hospices wishing to learn more about the aid in dying process, offering some hope more doctors will commit to participating.
In addition to the $3500 for seconal, Ray Walz paid Integrated MD Care out of pocket for his physician assisted death, which took place on February 4th of this year.
“Dr. Bob charged him $3000 for all of his care, which Ray didn’t think was expensive at all,” says Joy Jeffrey, Ray’s girlfriend of the past three years, who was with him when he died.
After Joy Jeffrey lost her husband of 40 years, she met Walz in a weekly grief therapy group — he’d lost his wife around the same time. The two grew close and began a relationship soon after.
“Ray was a horseman, a cowboy,” Joy remembers fondly, “We fell in love on horseback, actually.”
They enjoyed spending time with their dogs, and camping together on Mount Laguna, in the Sierras, and in the Anza Borrego desert. “There’s not a lot of people who love the desert,” Jeffrey says, “and can just sit there in a chair and watch the light change on the hills, and have it be a soul experience for them. But we found that intimacy with each other, and it was a miracle.”
When the End of Life Option Act became law, the couple read about it, and discussed it. It wasn’t long after that Walz was diagnosed with lymphoma.
It remained in remission for a while, and when tumors appeared around his throat, he received radiation treatment, which worked for a time. But after 12 weeks they returned, more aggressive, more painful. Left to run its course, the tumors would have eventually constricted Walz’s airways, choking him to death.
Mobile until the end, Walz remained active and strong for his 75 years, but in the last two weeks of his life he struggled to eat, and lost 20 pounds. He decided it was time. He reached out to family and friends, and invited them to come see him before he died. On Friday, his friends dropped by. On Saturday, his family, some visiting from the east coast.
“Then I came that Saturday at four,” recalls Jeffrey. “and we spent the night together.”
The following morning, Jeffrey, who had been a hospice volunteer for 20 years, helped Walz prepare his medication, and remained with him while he ended his life. “It’s an amazing process,” she says, “and it’s the most peaceful, beautiful death that you can imagine.”
With the hopes sharing Ray Walz’s end-of-life experience will help people better understand the prospect of a medically assisted death, here she shares the story of Ray Walz’s final day.
“When Ray got up that morning, he was like mister business. And I knew he would be, ‘cause that’s the kind of guy he is.
“We were up at 6. The thing is, you have to open all these little capsules, there’s a hundred of them. You have to open them, and take a toothpick, and dig out the medication… So he pulled them apart, and I took the medication out of one side and he took it out of the other… It took an hour and a half to get the medicine ready. Luckily it’s kind of like, it gives you something to do, so that your mind isn’t going crazy over all this stuff, like that this is your last morning together…
“They give you three anti-nausea medications to take… and then you have an hour before you take the seconal medication. And the way it turned out was so wonderful, because we had that hour, just the two of us, and it was just a sacred, intimate time between us. Ray was reading emails from his kids… he was reading the passages that meant a lot to him from that meditation center.
“My thing was, and it had been for weeks, that I didn’t ever want to break down in front of him. So that’s what I had to concentrate on, because I knew it would make it so much harder on him if I did.
“He was ready. So we went into the bedroom, and I got him all comfortable on the bed… He said to me, ‘I thought maybe I’d be nervous, earlier in the week when I was thinking about it. But, he said, ‘I’m totally at peace. Everything is done.’”
“I handed him the medication and he took it. I was reading a meditation for the dying, that I used to read for my hospice patients, that talks about saying goodbye to the body, and letting go of your name, letting go of your family, letting go of your life, everything that has been a part of you. In three minutes he was asleep.
“At the meditation center, each of us had a mantra… he was still breathing and peaceful, and very deeply asleep. So I kept reading the meditation to him, and singing his mantra, and in 40 minutes he was gone. His breathing just slowed. No suffering at all. It was perfect. And that’s what I wanted to give to him more than anything else, was a perfect death.”


On the afternoon of October 23rd, in the presence of his family, trailblazing San Diego surfer Bill Andrews ingested medication prescribed to end his life. Within a few minutes the 73-year-old had fallen asleep, and over the next quarter hour his breathing slowed, gradually, until it stopped altogether.

Andrews is often credited as the first to surf the celebrated waves of La Jolla’s Black’s Beach, and a photograph of him doing so appeared on a 1965 cover of Surfer magazine. By all accounts, Bill Andrews enjoyed a vigorous life as an action sports enthusiast, entrepreneur, engineer, photographer, father, and grandfather.
However, in 2016 he was diagnosed with amyotrophic lateral sclerosis, more commonly known as ALS, or Lou Gehrig’s disease. The neurodegenerative disorder destroys nerve cells.

Those afflicted with the disease become progressively paralyzed to the point they can no longer walk, move their fingers, speak, swallow, or, eventually, breathe. While the disease advances at different rates for different people, there is no cure. Despite outlier cases such as Stephen Hawking — who recently passed at 76, after 55 years enduring a variant of ALS — it’s roundly considered a terminal diagnosis, with as little as two year life expectancy.

For Andrews, the symptoms progressed rapidly, his loss of motor function compounded by acute pain due to a lifetime of broken bones and other sporting injuries. Facing paralysis and suffering in the imminent future, Andrews chose instead to schedule the end of his own life, with the assistance of a physician.
After decades of controversy and public debate, the legal ability to do so has been available in California since mid-2016. Advocates have used several names to describe it: physician assisted suicide, medical aid in dying, death with dignity, the right to die.

Whatever the terms used, the California Department of Public Health reports 191 people acquired prescriptions to end their lives in the last seven months of 2016. At least 111 are confirmed to have taken the medication and perished.

But it’s still a new practice, and most of what we know about how the law is being put into practice is anecdotal. Just like the unsettled vocabulary involved in taking a prescription to take one’s life, the ways it’s being applied, both from a business perspective and a cultural standpoint, are starting to come into focus.

The End of Life Option Act became California law in June 2016 when it was passed by the state legislature and signed by Governor Jerry Brown. It states that a patient diagnosed with a terminal illness may request life ending medication from a licensed medical doctor. But due to the controversial nature of the law, it’s loaded with safeguards against patient abuses.

First of all, the patient must be deemed of sound mind, and not expected to survive a specified illness for more than six months. The patient must first make an oral request for life-ending care to his or her attending physician — alone; that is, without any loved ones or caregivers present to exert influence or duress. The physician must make the patient aware of all alternative treatment options, including hospice care. After a mandatory 15-day waiting period, a second oral request must be made under the same conditions, followed by a written request, signed in the presence of two witnesses.

The patient must also consult with a second physician to confirm the terminal diagnosis, and independently corroborate the patient’s mental state. Due to the soundness-of-mind requirement, Alzheimer’s patients or anyone affected by dementia are disqualified.
Once the medication is secured, a patient must ingest it him- or herself. The preferred prescription, used by Bill Andrews, is for a controlled overdose of the barbiturate seconal, a powerful sleeping agent. One hundred capsules are prepared into a liquid solution for the patient to drink.
A doctor cannot pour it down a patient’s throat, nor a family member. In some cases, the end of life option may boil down to whether a person can suck the medication down a straw and swallow it. At any time, even at the last moment, a patient may simply decide not to take the medication, choose to take it later, or simply keep the medication on hand while allowing a disease to take its course.
A few days prior to taking his fatal last drink, Bill Andrews frankly discussed his illness, and his decision to die on a podcast recorded by his doctor. “Just a year and a half ago I was in Peru surfing,” he said from inside his room at a San Marcos assisted living facility. By contrast, he characterized his present-day life as “horrible” and sedentary. “I get fed. I wear diapers. I’m kind of confined to my bed.”
With the support of his family, he planned how his death would go. “The thing that’s the most incredible thing to me,” Andrews said, “is being able to choose when you’re going to die… I’m choosing the time. I’m choosing the place. I’m choosing the environment. I’m choosing the company. And for me…” he added, “I can’t think of anything better.”
The avid surfer, motorcycle racer, and adventure traveler would find a gentle, painless end, surrounded by people he loved, having said his last goodbyes and tied up all his loose ends. “I’ve kind of been a pioneer in a lot of things,” he told his doctor on the podcast, explaining why he decided go public with his story. “I think this can do a lot of good.”
The doctor assisting Bill Andrews with his death was Bob Uslander, known to his patients as Dr. Bob.
Uslander established his practice, Integrated MD Care, in early 2016. Its primary purpose — then and now — is to provide in-home palliative care. Hospice. “The vast majority of what we do is take care of people in their homes,” he says. Some of his patients aren’t dying, rather they’re enduring prolonged recoveries from serious illness or injury. “A lot of our patients are older, they have dementia. Or they’re just frail, and they need someone to be there to take care of them.”
However, by the time Bill Andrews first approached him, Uslander had already been gaining a reputation as San Diego’s go-to primary physician for people seeking medical aid in dying. Uslander has helped dozens of patients gain access to life-ending medication — far more than any other local doctor. He’s traveled to assist patients in Orange County, Los Angeles, Riverside, Palm Springs, and Oakland. In the process, he has become one of the law’s most visible advocates.
He didn’t set out to be. Focused on starting his new practice when Jerry Brown signed the law, Uslander says he took note of it as an advancement of civil rights, but didn’t think of it as something that would impact him so significantly. “I thought it was a good move,” he says. “Progress. And that once the law went into effect, that doctors would be willing to help their patients.”
However, that has not been the case. Most medical professionals in San Diego have shied away from offering aid in dying to their patients, or referring patients to a doctor who will.
“It was really surprising to me when people started calling me,” recalls Uslander, “saying I can’t find anyone to help me. My own doctor won’t do it, my specialist won’t do it. And some of these people had called 10, 25 physicians, or more. And each time, they got denied.”
By law, health care providers are not required to offer medical aid in dying, and organizations such as hospitals or medical practices may prohibit doctors they employ from doing so. While statutes protect physicians from criminal, civil, and professional liability when they operate within the constraints of the law, a presumed risk to reputation proves enough to make many hesitate.
“It has a big impact, and we know it’s controversial,” confirms Uslander “It’s a service that I would be okay not providing if doctors would step up and take care of people adequately, but that’s not happening. I feel like, if I’m not doing it, there’s way too many people who are going to struggle, and have bad deaths.”
In November, Uslander launched the podcast, “A Life & Death Conversation.” It covers topics ranging from dealing with suicidal thoughts to coping with grief, and a lot of its episodes serve to bring the aid in dying topic into the public sphere, explaining the concept of a good death.
The doctor has found families have an easier time addressing end-of -life options when they can hear about how peaceful the process can be. Following Bill Andrews’s appearance, his three sons returned to record a follow up interview, describing the life-affirming experience his family shared on the day of his death, and the days leading up to it. According to one of his sons, Andrews described his last three to five days as “the most peaceful time of his life.”
Subsequent episodes have featured aid in dying advocates, a grief counselor, a hospice worker, and a doctor from the Netherlands speaking by phone to discuss his experience with euthanasia. The practice has been legal there since 2002, and today reportedly accounts for 4.5 percent of that nation’s deaths.
Uslander the podcast host is a stickler for the language we use to describe it. He avoids terms that carry negative connotations. For example, he points out that, in California, physician assisted suicide is not euthanasia. Officially, it’s not even suicide.
“Euthanasia is active,” he says, “It’s a physician actively ending a person’s life, at their request,” while the End of Life Option Act requires life-ending medication to be self-administered. Meanwhile, to ensure life insurance policies cannot deny benefits to patients who use the law, it clearly states that the patient’s death certificate should name the terminal diagnosis as cause of death. It may be cancer, ALS, heart disease, but never suicide.
A doctor is not required to be present, however most of Uslander’s patients have invited him to take part in their final moments, both for emotional support, and to ensure the medicine is administered properly. The moments he’s witnessed have reinforced to him the positive impact of the new law, and the value of a good death.
“Sometimes the last words they utter are directed at me,” he reveals, “It’s usually something like, ‘Thank you. Thank you for being there.’”
The patient’s family members often echo the sentiment. While he finds it gratifying to hear, Uslander tries to keep such praise in perspective. “It’s not fair,” he says, “I’m held in this light, as the person who stepped in to give them this final gift, when no one else would.”
While opponents of aid in dying have long argued that family members and care workers would coerce patients into physician assisted death for their own financial gain, Uslander’s experience has thus far shown otherwise. “There’s never been one incident that has smacked of that,” he says, “It’s kind of been the opposite.” Patients have been the ones convincing families to accept their decision to die.
Uslander tells the story of a woman in her late 90s who had a hard time getting her children and grandchildren to accept her plan. “There was a lot of misinformation and fear about what was going to happen,” he says, “But once they understood what the process is, and how peaceful it usually is, then they came around to supporting her.”
When the time came, the woman gathered her extended family around her for two days of remembrances and farewells. Then, with children, grandchildren, nieces, and nephews there to support her, she drank the medication, and fell asleep. “As soon as she stopped breathing and died,” Uslander recalls, “everybody stood up and gave her a standing ovation.”
In the August 2016 Voice of San Diego story “What I Learned Helping My Sister Use California’s New Law to End Her Life,” Kelly Davis documented the death of her sister, Betsy, who was in the advanced stages of ALS when, that July, she chose to be among the first in the state to legally ingest life-ending medication prescribed by her doctor.
The story, which received national attention, depicted an emotionally charged end-of-life celebration, wherein Betsy Davis invited friends and family to join her for a two-day gathering of drinks, music, and fashion that culminated with her falling asleep for the last time during an Ojai sunset.
Kelly ultimately helped Betsy realize her end of life vision, though she shares via email that her first instinct was to try to keep her sister alive. “Of course I didn’t want her to die, ever,” she writes. “I was constantly looking for some miracle cure, pestering her ALS doctor about clinical trials.”
However, during a visit several weeks prior to Betsy’s death, an ordinary moment brought a shift in Kelly’s perspective. “She wanted to take a nap, so I left the room,” Davis remembers. “A few minutes later, she called for me to come back to her room. She couldn’t sleep because she had an itch above her eyebrow that was driving her crazy and couldn’t reach it, so I scratched it for her. I left her room thinking about how, if I hadn’t been there, she would have been lying there, just in agony. Even though I’d seen how much she’d suffered in the three years since her diagnosis, there was something about that moment that really struck me and made me realize how much her quality of life had diminished and it was selfish of me to not be OK with her decision.”
Betsy Davis was not alone in wanting to be present for an end-of-life celebration to help herself and her loved ones to let go. On Uslander’s podcast, Bill Andrews’ sons tell how the surfer’s 95-year-old mother performed a hula song she had written for him, as the family gathered around him for the last time. Uslander tells of another patient who gathered friends so he could break out a bottle of scotch he’d been saving for a special occasion, to share one last drink before taking his medication.
Uslander says most of his patients don’t try to turn the moment into an event. Many are already suffering, and simply wish to get it over with. A number of his patients haven’t survived the 15-day waiting period required by the law.
However, others have created personal rituals, ranging from the reading of Bible verses, to the ringing of Buddhist bells. For the most part, they’ve been ad hoc rituals. While we have established norms for funerals, we don’t have practiced customs for commemorating a person’s death while it’s happening. In some cases, people embrace the opportunity to effectively be present at their own funerals.
Melissa Rainey operates a business called Eternally Loved, which offers memorial event planning. She started the work after a close friend died, and she saw the value it provided the family when she stepped in to make funeral arrangements as they grieved.
Recently, Rainey’s begun planning what she’s calling living memorials: arranging events for terminally ill patients. She tells that one of these clients had scheduled her fete ahead of her own physician-assisted death, opting for an elaborate send off.
The woman had a great sense of humor, and had Rainey book a stand-up comedian to emcee the party, introducing loved ones to deliver eulogies. “It broke the ice, and it also created an atmosphere of joy,” recalls Rainey, who also brought in therapy dogs, for people to pet in case someone was having a hard time.” And she had the party catered with the woman’s favorite foods, including Chinese food, donuts, Jewish deli, and In-N-Out Burger.
Historically, the Hemlock Society of San Diego has been the leading local advocate for this cause. The 31-year-old organization has advocated for terminal patients’ right to die, led by Harvard trained forensic psychologist, Faye Girsch, who founded the local chapter in 1987, and eventually served as president of its national, parent organization. After that group merged with another to form a new entity, Compassion & Choices, Girsch split off Hemlock Society of San Diego as an independent organization.
Girsch became involved in the right-to-die movement while working with the American Civil Liberties Union in 1983, on the nationally publicized case of onetime San Diego State student Elizabeth Bouvia, a quadriplegic who filed an injunction against a hospital for keeping her alive against her wishes.
“She wanted to die by refusing food and hydration, which you could not do at the time,” recalls Girsch, “So she admitted herself to Riverside Hospital, and they were force feeding her.” Girsch was tasked with evaluating Bouvia’s state of mind, and found her to be competent. Bouvia lost the case.
However, the circumstances inspired Girsch to lobby for changes to health policy, including working to help put Proposition 161, the “Aid in dying act” on the California ballot in 1992.
While the nonprofit Hemlock Society celebrated the passage of the End of Life Options Act, it continues to advocate expanding the law to include a wider range of patients. For example, while Girsch actually opposes capital punishment, she supports lethal injection being added to the end-of-life option, as Canada’s national health care policy allows. This would extend the right to die to someone unable to swallow medication.
Uslander tells of such a patient at his practice, who opted to have an endogastric tube inserted so he could push the lethal prescription into his stomach with a large syringe. With a progressive disease such as ALS, had that patient lost use of his hands before having a chance to take the medication, he would not be able to access the California law.
It’s one reason the Hemlock Society also finds the 15-day waiting period problematic. It’s included to give patients a chance to change their minds, and Uslander reports that a significant number of his patients do so — either during the waiting period, or after they’ve received the medication.
However, he’s also seen patients perish while waiting for a prescription. Some of these patients experienced what he calls “a bad death,” knowing how close they’d come to the peaceful one they’d been seeking. Some may have received the medication in time, if they’d found a doctor sooner.
So, the Hemlock Society has been working to compile a list of local doctors willing to support medical aid in dying. Thus far, it’s a short list, with Dr. Bob at the top of it. “We’ve being doing this now for a year,” says Girsch, “calling doctors and hospices, seeing whether they will participate or not. And generally, it’s not.”
“Nobody wants to be Dr. Kevorkian,” suggests Charese Brooker, the Hemlock Society’s executive director.
She’s referring to the controversial physician-assisted-suicide activist who made headlines in the 1990s for helping 130 terminal patients end their lives, then wound up in prison for eight years on a second degree murder conviction. While the California laws offers copious legal protections for practitioners, Kevorkian’s legacy includes the fear of reprisal for doctors helping patients die.
Brooker is a registered nurse who’s spent most of her nine year career working in hospice, and has seen the challenges terminal patients face in finding willing physicians. “Even though we now have the act in place,” Brooker says, “we’re seeing a lot of people having trouble accessing it… It’s hard to find a doctor. And then it’s hard to find a second one.” For a patient with terminal illness, she adds, “It’s very cumbersome and very draining.”
Compassionate Choices has been keeping track of whether local hospitals and hospices allow their doctors to serve as attending or consulting physicians, and post the information to a searchable web page. Organizations affiliated with the Catholic church and other religious organizations don’t allow doctors to participate. Neither does VA health care, which is subject to federal law. Even organizations that do offer aid in dying as a policy — such as Sharp HealthCare and Kaiser Permanente —don’t widely advertise the service. There’s little or no acknowledgement of the End of Life Option Act on their web sites, and phone inquiries receive limited or no response.
“What you’ll end up finding is people won’t talk to you,” Brooker says, “They’ll send you on this wild goose chase.”
Even when organization hierarchies aren’t an issue, individual doctors are free to opt out, and often do. Aid in dying advocates contend many, if not most, doctors do not bring up the medical aid in dying option with their terminal patients: particularly oncologists, neurologists, and other specialists who treat most of the patients who qualify. Even if they’re willing to assume the responsibility, they don’t advertise the fact.
“Unless they already have a relationship with the patient, they’re not going out and making it known that they’re doing this,” says Uslander. Publicly, he says, “I’m the only one who’s willing to take on patients.”
Uslander reports patients come to him saying their doctor refused to discuss it, or their hospice disallowed it. Others say their doctors agreed to do it, and even initiated the process, then changed their minds during the mandated 15-day waiting period, forcing the patient to start over. In some instances, the doctor agreed to serve as the consulting physician required by the EOLOA, but not as the attending.
“People are more willing to be the consulting physician, in my experience, than the primary physician,” says Brooker. “A lot of times, what we’re finding is they refer to Dr. Bob.”
According to California’s statistics, 84 percent of those seeking physician assisted death are enrolled in hospice care, which is no coincidence. The six-month terminal diagnosis required by the law is the same term established to receive hospice benefits.
Brooker proposes that hospices are unwilling to administer the option because some people still find a stigma attached to hospice itself. “People think, I’m going to go to hospice and you’re going to kill me.” In response, she says, “hospice has for a long time pushed that idea away.” Like hospitals, they’re reticent to market or discuss their aid in dying policies.
Hospices have at times been accused of rushing patients to death, and other times accused of keeping them alive longer to increase profits. Instances of fraud, such as the highly publicized case of San Diego Hospice allegedly misreporting patient information in 2012, have kept such suspicions alive. As a result, hospices have reaffirmed the credo that they “neither hasten nor postpone death,” which they can’t be seen to do if they publicly offer aid in dying.
However, a relatively noncontroversial practice that routinely takes place in hospices, and hospitals, is palliative sedation. Also known as terminal sedation, it’s what happens once a patient effectively experiences too much pain to remain awake. When the dose of morphine required to make them comfortable, also renders them unconscious.
Palliative sedation is often simply the inevitable end of palliative care; sometimes it’s a conscious decision, oftentimes it’s a circumstance that commences gradually, to the point that reviving a patient to the pain of consciousness would be objectively cruel. In these cases, a terminal patient may linger in this terminal morphine state for days or weeks.
But in Brooker’s experience working in hospices in the Midwest, where aid in dying is not legally available, patients would commonly ask for an end to life by this means, sometimes directly.
“I would have people all the time ask me,” she reports, “Would you kill me? Or, Would you give me that magic dose?”
To Brooker, medical aid in dying offers a more humane alternative. “Terminal sedation has always hit me the wrong way,” she says. “If we’re going to palliate someone so much that they’re in a coma… then what’s the point?”
There’s one point for patients of limited financial means: hospice is affordable. It’s been covered by Medicare since 1982. The end of life option is not.
Bob Uslander reports his aid in dying patients have ranged in age from early 40s to 106 years old, but are usually between 70 and 90. They tend to be college educated, with a high number of them professionals: doctors, lawyers, college professors. More than half have been men, though not by much. The overwhelming majority have been white.
While the sample sizes are too small to draw any concrete conclusions, these demographics roughly match the first set of data reported by the Department of Public Health.
In a nutshell, those who can access medical aid in dying must also be able to afford it. A prescription for seconal costs about $3500. An alternative mix of medications has shown to be effective for about $800 — Betsy Davis used it — but Uslander says it can take longer to work, hours potentially, and patients may gasp or twitch, which can be distressing to families.
Meanwhile, Integrated MD Care is a boutique palliative care provider employing specialists who provide treatments such as physical therapy, massage therapy, acupuncture, music therapy, and cannabis treatment, in addition to traditional nursing care. Uslander’s time does not come cheap.
“I’m not working with insurance, so [patients are] paying me a fee,” he says. He doesn’t share exact numbers — “My fee ranges from zero to something,” he says — but he has worked pro bono. “I have the ability to take care of people without charging them, which I do on occasion.”
However, free care is not sustainable for his business, so Uslander has taken steps to launch the Integrated Lifecare Foundation, a 501(c)(3) nonprofit that will raise funds to support providing patients with lower economic means access to the palliative services Integrated MD Care offers, including medical aid in dying.
“The one aspect that is uncomfortable for all of us at IMDC is that people without some financial means will not benefit from what we can offer,” explains Uslander.
In addition, he has been asked to offer training sessions to local hospices wishing to learn more about the aid in dying process, offering some hope more doctors will commit to participating.
In addition to the $3500 for seconal, Ray Walz paid Integrated MD Care out of pocket for his physician assisted death, which took place on February 4th of this year.
“Dr. Bob charged him $3000 for all of his care, which Ray didn’t think was expensive at all,” says Joy Jeffrey, Ray’s girlfriend of the past three years, who was with him when he died.
After Joy Jeffrey lost her husband of 40 years, she met Walz in a weekly grief therapy group — he’d lost his wife around the same time. The two grew close and began a relationship soon after.
“Ray was a horseman, a cowboy,” Joy remembers fondly, “We fell in love on horseback, actually.”
They enjoyed spending time with their dogs, and camping together on Mount Laguna, in the Sierras, and in the Anza Borrego desert. “There’s not a lot of people who love the desert,” Jeffrey says, “and can just sit there in a chair and watch the light change on the hills, and have it be a soul experience for them. But we found that intimacy with each other, and it was a miracle.”
When the End of Life Option Act became law, the couple read about it, and discussed it. It wasn’t long after that Walz was diagnosed with lymphoma.
It remained in remission for a while, and when tumors appeared around his throat, he received radiation treatment, which worked for a time. But after 12 weeks they returned, more aggressive, more painful. Left to run its course, the tumors would have eventually constricted Walz’s airways, choking him to death.
Mobile until the end, Walz remained active and strong for his 75 years, but in the last two weeks of his life he struggled to eat, and lost 20 pounds. He decided it was time. He reached out to family and friends, and invited them to come see him before he died. On Friday, his friends dropped by. On Saturday, his family, some visiting from the east coast.
“Then I came that Saturday at four,” recalls Jeffrey. “and we spent the night together.”
The following morning, Jeffrey, who had been a hospice volunteer for 20 years, helped Walz prepare his medication, and remained with him while he ended his life. “It’s an amazing process,” she says, “and it’s the most peaceful, beautiful death that you can imagine.”
With the hopes sharing Ray Walz’s end-of-life experience will help people better understand the prospect of a medically assisted death, here she shares the story of Ray Walz’s final day.
“When Ray got up that morning, he was like mister business. And I knew he would be, ‘cause that’s the kind of guy he is.
“We were up at 6. The thing is, you have to open all these little capsules, there’s a hundred of them. You have to open them, and take a toothpick, and dig out the medication… So he pulled them apart, and I took the medication out of one side and he took it out of the other… It took an hour and a half to get the medicine ready. Luckily it’s kind of like, it gives you something to do, so that your mind isn’t going crazy over all this stuff, like that this is your last morning together…
“They give you three anti-nausea medications to take… and then you have an hour before you take the seconal medication. And the way it turned out was so wonderful, because we had that hour, just the two of us, and it was just a sacred, intimate time between us. Ray was reading emails from his kids… he was reading the passages that meant a lot to him from that meditation center.
“My thing was, and it had been for weeks, that I didn’t ever want to break down in front of him. So that’s what I had to concentrate on, because I knew it would make it so much harder on him if I did.
“He was ready. So we went into the bedroom, and I got him all comfortable on the bed… He said to me, ‘I thought maybe I’d be nervous, earlier in the week when I was thinking about it. But, he said, ‘I’m totally at peace. Everything is done.’”
“I handed him the medication and he took it. I was reading a meditation for the dying, that I used to read for my hospice patients, that talks about saying goodbye to the body, and letting go of your name, letting go of your family, letting go of your life, everything that has been a part of you. In three minutes he was asleep.
“At the meditation center, each of us had a mantra… he was still breathing and peaceful, and very deeply asleep. So I kept reading the meditation to him, and singing his mantra, and in 40 minutes he was gone. His breathing just slowed. No suffering at all. It was perfect. And that’s what I wanted to give to him more than anything else, was a perfect death.”
Comments