 Facebook
Facebook
 X
X
 Instagram
Instagram
 TikTok
TikTok
 Youtube
Youtube
When the first hard contraction hit my wife Deirdre, buckling her at her middle and squeezing from her lungs a shocked cry, her first thought was, “I don’t know if I can do this without drugs.” Her second thought was, “I don’t know if I ever want to do this again. She did it—gave birth—without drugs, and she does want to do it again—without drugs.
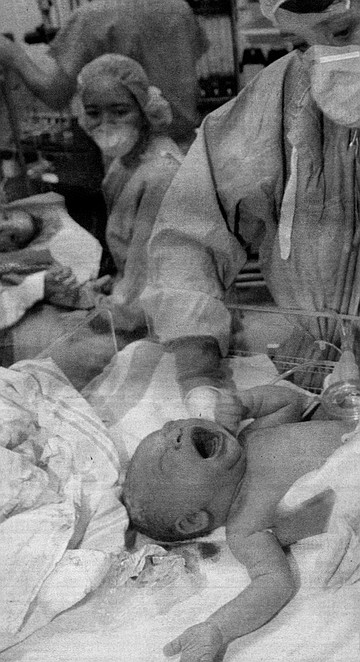
Looking back on our decision to deliver naturally— letting nature take its course as much as possible, without intervention — I can recall only a vague certainty that it was the right way to go. The vagueness didn’t make my certainty any less certain — I had a strong gut feeling, a conviction — but I couldn’t give much of an accounting for it. My sister-in-law had delivered naturally and was a strong advocate. But I wasn’t exactly sure of her reasons.
Deirdre had a clearer idea. “It seemed right, first of all, that you don’t take drugs, so the baby doesn’t get the drugs. The baby is much smaller. And I had heard there were side effects — sometimes the baby has trouble nursing, sometimes the mothers have headaches.
“And I wanted to experience childbirth. I really did want to feel the baby being born, even if it hurt. I wanted it to be a good experience too. Also, I was afraid of drugs; some other women I knew had bad experiences. They were going to have children again, but they were afraid.”
“I felt like I had been hit by a Mack truck,” said a friend who had received pitocin, a drug that stimulates contractions. “It was the most horrible experience of my entire life.” Her second child was born at home, naturally, and Deirdre characterized it as a serene, relaxed, wonderful thing — “like night and day.” She knows other women who recalled positive experiences with drugs, but she still wanted to go natural.
Several months into Deirdre’s pregnancy, we started attending a Bradley Method birthing class, led by Nancy Flint. The method is named after Dr. Robert Bradley, author of the seminal work, Husband-Coached Childbirth, but it is not so much an esoteric method developed by a doctor as a policy of cooperating with nature.
Because such a policy often conflicts with the standard practice of most hospitals, Bradley people have something of a reputation as fanatics. Flint, on the other hand, is just the sort of person you would want to introduce it to someone. She is unthreatening, unmilitant. She has given birth both naturally and with drugs — concern for the baby’s health after a car accident led her to accept a pitocin-induced labor, but she declined painkillers. She has worked with an obstetrician and as a doula, or labor assistant.
Her North Park home, where she teaches her class, is cozy and bright, stenciled and knickknacked. Her features are soft and friendly; her manner, nice with a hint of businesslike efficiency. She is not above making a strong statement — “My very blunt view of women taking medication despite the fact that it can harm the baby is that it’s very selfish,” she says — but in general, she is looking to avoid a fight. This is not always easy; Bradley students are often thought of as people who are suspicious of doctors and who try to buck the system.
“In the last couple of years or so,” admits Flint, “I have started telling my students not to really advertise themselves as Bradley students; rather, as natural child-birth students. Something other than the Bradley name, just because of the negative connotations that go with it. When I was in labor and they knew I was a Bradley teacher, that’s what they put under ‘Problems with patient.’ That was my one problem. They sort of assume that the person is going to give them a hassle.”
Hassles do happen. Flint remembers a man who pushed a doctor away from his wife because he didn’t want her to stay in bed and be monitored. The man was restrained and removed from the room. “It’s only been one person in a hundred, but that’s the one person that doctor will remember forever, that this Bradley stuff is horrible.
“Trust is the big issue. They feel like they’re not being trusted if everything they do is questioned.” So, Flint counsels her students to try to establish trust within the context of the birth plan, the list of things the couple does and does not want during the birth. This is the plan we submitted to Kaiser, signed by ourselves and our certified nurse-midwife:
Birth Plan
We, Deirdre and Matthew Lickona, would like to cooperate as much as possible with the professionals who will be aiding Deirdre during her labor and delivery. We would also like Deirdre to deliver as naturally as possible. To minimize tension between these two desires, and to indicate our wish to be both flexible and responsible in working with Kaiser Permanente, we have prepared this Birth Plan. We would like Deirdre to deliver under the following conditions:
Mobility — we would like Deirdre to be able to walk freely during labor. This includes use of the shower.
Minimal electronic fetal monitoring [EFM] — to enhance mobility, we would like to limit use of the EFM to no more than ten minutes per hour.
No routine IV — we would prefer that Deirdre not receive an IV and that she be allowed to eat and drink during labor instead.
No medication — we would prefer that medication not be offered except in an emergency.
No frequent exams — we would prefer that Deirdre not be examined unless necessary.
No episiotomy — we would prefer that Deirdre receive no episiotomy and that massage and/or warm compress be used instead. If it comes to a choice between cutting and tearing, we would prefer to let Deirdre tear.
Upright position — we would prefer that Deirdre not be flat on her back during delivery. Rather, we would like her to be sitting up.
No separation — we would prefer that Deirdre be given her baby immediately after delivery for breast-feeding and bonding and that she not be separated from her baby at any time.
Because we want our baby to be as healthy as possible, we will of course be flexible on these conditions should complications in birth make it necessary. We have faith in the competency and professionalism of the Kaiser staff, and should complications arise, we would like to be informed so that we may discuss the choices to be made and determine a new plan of action.
Thank you for your understanding and cooperation.
Our requests reflected the basic tenets of the Bradley Method. I asked Flint to comment on each. Other people I spoke with for this story treated some of the things she talks about in greater depth and detail. But what she said, I think, serves as an adequate introduction to some of the issues associated with the method.
Movement: “It speeds labor. It makes it progress at a regular pace. If you stay in bed, labor tends to go very slowly; it does not progress. Therefore, if there’s failure to progress, they have to start using pitocin. But movement is a natural way to keep labor going at a normal pace, to keep the cervix open, to keep the uterus contracting. Gravity is the number-one factor, and it keeps all the muscles working rather than just being latent in bed. It just makes sense — feels better too.”
Limited electronic fetal monitoring: When you’re on the monitor, which measures the baby’s heart rate, you have to be lying down. Limited monitoring allows for movement. Further, research has shown that “electronic fetal monitoring leads to more C-sections than are necessary, and it doesn’t necessarily lead to a healthier outcome — it’s the same with or without it.” No routine IV: Though movement is possible with an IV, it’s cumbersome. “Just being stuck with an IV can be painful and uncomfortable, intrusive to your sense of peace and calm. Instead, let’s drink fluids and we still get the same benefit.”
No medication: When I asked Flint what natural childbirth is, her definition was negative, defined against what she sees as the current conception of normal birth practices — “No intervention. No drugs, no medications. Nothing other than your own power.” Everything on the birth plan falls under the category of “No intervention,” but what comes first to Flint’s mind, what is most important, is drugs.
The two kinds of drugs Flint mentions are pitocin, which augments contractions, and narcotics, which kill pain. The narcotics are often administered through an epidural in the mother’s back. “According to the AMA,” says Flint, “there is no known drug safe for the fetus. So why would you use them? Opponents say, ‘Well, the odds are so long that something could go wrong.’ But that’s still a risk I just find it odd that women are so careful during pregnancy to not take anything, but suddenly it’s okay when you’re in labor.
“There’s evidence to show that some birth drugs remain in the baby’s system for up to seven days. They cause bonding difficulties, the babies are not able to focus as well, so the mother-infant bond is delayed. They are very lethargic. The sucking mechanism is very frequently interfered with, and therefore breast-feeding becomes very difficult.
“There’s always the risk to the mother too. We don’t know if she’ll have some kind of allergic reaction to these drugs. Some women have been known to have heart problems. She’s in trouble, they have to have a C-section, it gets complicated. Yes, it’s all rare; yes, it’s probably a minor effect on the baby, but we’re not sure. There’s some evidence stating that learning disabilities may be caused by birth drugs. There’s not a lot of financial backing of research to prove these facts, because everybody says, ‘I was born with drugs, and look at me, I’m just fine.’ But why are we doing this? Why are we taking these risks?
“In other countries, they do not use birth drugs. They have midwife delivery, and physicians are there for emergencies only, which is always the way it was supposed to be. They have much lower infant mortality rates. There’s a very large study that’s come out of Dublin that compares midwifery to American obstetrics. Their first-time mothers give birth in 5 to 6 hours, our first-time mothers in, like, 12 to 18 hours. They attribute that to the one-on-one, woman-to-woman care, and plus, they are not offering all the drugs.”
No frequent exams: Flint didn’t comment much on this one, but from my conversations with people associated with the Bradley movement, I got the impression that exams were seen as a doctor’s starting point for intervention. If a doctor checked a cervix and found it the same size over a three-hour period, he or she might conclude “failure to progress” and recommend pitocin to get things going. Or an exam might lead a doctor to think that the head was too big to fit through the pelvis, necessitating a C-section.
Their response to these sorts of conclusions was that one labor is not like another. One woman’s cervix might open steadily, another’s might stall at five centimeters for several hours, then open to eight or nine centimeters in a very short time. If she had waited that extra hour, pitocin might not have been necessary. In the case of the big-headed baby, “hormones and enzymes are released constantly in our body that are allowing the pelvis to move out easier. It may appear [that the head is too big for the pelvis] because they don’t allow time for the pelvis to open up.” There is a general faith that nature will take its course in most situations, but not according to any particular schedule.
No episiotomy: “That’s a very controversial issue. You’ll read all kinds of things on both sides. But in our experience, what we have seen is, number one, a surgical cut leads to weakened skin tissue. Therefore, the cut often leads to a bigger tear, so you’re going to be opened more than you would have been on your own. Two, it heals much slower than a tear. It’s a very painful healing process.
“The controversial part is that doctors are taught to believe a cut will be easier to repair in sewing up than a tear, and other people believe that a tear is easier to repair than a cut. I always use the analogy of a puzzle piece. Puzzle pieces lock together perfectly, whereas, if you put two straight lines [flat surfaces] together, there’s nothing to link back together again. So in my mind, a tear would heal — and be able to be repaired — better, easier, faster.
“I’m blessed enough to have had both experiences. The first one, I had a huge episiotomy. They said the baby was in trouble and they needed to get her out. I don’t think they even asked me, they just did it. It was enormously painful afterwards. I couldn’t sit down without pain for six weeks. Sex was incredibly painful for a year. I think they cut way too far, and the repair and the healing took way too long. The second time, without an episiotomy, I had almost no pain afterwards, could sit down normally, and felt perfect after three weeks.”
However, as with other interventions, her opposition is not absolute. “If somebody were to say to me, ‘Okay, your baby’s in trouble, do you want to be cut or do you want to wait and see what happens?’ I’d say, ‘Yeah, cut me.’ On the other hand, if they’re just routinely cutting every single woman, which is the case 98 percent of the time, for no medical reason other than to just speed things up for the doctor’s sake... It’s been deemed the second most unnecessary surgery in the United States, circumcision being the first.”
Some time ago, while channel grazing, I ran across an episode of Chicago Hope and heard a similar argument being made. The skeptical doctor retorted that tears, since they were not controlled like cuts, could extend all the way down into the rectum, a stomach-gripping thought. Flint’s advice for avoiding such extensive tearing:
“Number one — good nutrition. A good, balanced diet and lots of fluids keeps the skin soft and elastic. Number two, a few weeks before the due date, do the perineal massage exercise. Take your thumb and forefinger, lubricate them with oil, olive oil would be fine. Put the thumb inside the perineum, about an inch down, and your forefinger outside. Pull out enough that you feel it tug, and make the shape of the letter U, going up and down both sides of the vaginal wall. The whole time, you’re pulling out, away from your body, enough so that it feels like, ‘Owie,’ a kind of tingly sensation. You can do it in the tub — it makes it a little more comfortable. Just a few minutes every day, that’s been shown to help prepare the tissue.”
During labor, when the baby’s head is ready to exert pressure on the perineum, a warm compress maybe placed against the skin to act as a buffer. And if the mother is only semireclined, instead of flat on her back, the back of the baby’s head comes out first, as opposed to the face, which is larger.
Another argument for the controlled cut is that it is insurance against the danger of tearing upwards, into the clitoris. Janet Cunningham, a certified nurse-midwife I interviewed for this story, had this response:
“If the head just comes flying out, it can get really horrendous — it would be better to start an opening at the bottom. Then you would just get a tear to the bottom, which is much better. But if the mother’s comfortable, and everybody’s relaxed and patient, and you keep the head flexed, you can protect the upper structures. Just by gentle pressure down as the head crowns. You don’t have to press very hard—just enough to guide it.”
Upright position: “In America, most women are not allowed to be vertical during labor. Being able to walk helps the pelvis move out easier.” When I spoke with a licensed midwife, Michelle Freund, she showed me a series of slides of woodcuts and illustrations, dating from medieval to colonial times, which depicted women giving birth in upright to near up right positions. She contended that this has been the practice throughout history because this is what works.
No separation: Though this request applies to the time after birth, Flint sees it as crucial. Her first examples of the dangers of drugs had to do with postpartum effects — trouble focusing, leading to trouble seeing Mom, leading to trouble bonding and trouble breastfeeding. “I find it very interesting that babies are born with the ability to see just 12 inches, which is exactly the distance from the breast to the mom’s face. Holding your baby skin to skin, the baby will imprint on mother and bond with her, become close with her, much faster than if it weren’t breastfeeding.
“Not only will the baby learn to know the mother faster, but the mother will learn to know the baby faster. She will learn the baby’s different cues— the different cries. She will be able to respond to her baby much quicker, know what her baby wants. And by nursing, you tend to hold your baby more, so the baby will become more alert and responsive and smile a lot and make cooing noises and that sort of thing. It happens much earlier and more frequently because the two have connected so strongly.” She also points to the physical benefit of antibodies in breast milk and claims that it has been proven that babies who are breast-fed have slightly higher IQs than babies who are bottle-fed.
This is not a story about breast-feeding, but Flint sees contact and breast-feeding as an extension of the mentality that supports natural childbirth —the baby’s welfare above all else, even the extreme pain of labor. “The toughest part [about drugs] is that it can hurt the baby, and how could you possibly take that risk? I really have trouble dismissing that part. It’s only one day of your life. I don’t get why people are unwilling to do the best for their child. If somebody were to tell them, ‘Don’t worry about it, drugs aren’t going to affect your baby,’ I would say, ‘Are you absolutely sure?’ They can’t answer, ‘Yes,’ they just can’t.” Nevertheless, the pain is the reason why a lot of women receive drugs, and so the pain must be addressed. Part of our Bradley class involved training in pain management. “You squeeze your wife’s arm or her leg or something, hard enough that it hurts a little bit. You pretend that you’re in labor and having a contraction, usually about 90 seconds to 2 minutes. She needs to be able to breathe deeply, slowly, and relax all the muscles that are in her body, including the muscles that are in pain. Just become completely loose, and let her mind be free and use whatever mental and emotional ways of relaxation she can for those two minutes.”
Flint is a Christian; so is her class. “We do a great deal with prayer and Scripture reading. Most couples have particular prayers and particular Scriptures that mean a great deal to them. Often, it is the husband that is speaking these prayers to God for her, or speaking the Scripture to her, so she can be at peace.
“I don’t think labor is easy — I don’t think God intended it to be easy.” (Echoes of the curse put upon Eve when she left the garden — “In pain shall you bring forth children.”) “I think He wants us to look to Him for help. I don’t know if we would if we weren’t in pain. Christ went through a great deal of pain for us. He can bear our pain, if we just lean on Him.”
Besides the explicitly religious practices, Flint propounds a sort of meditation. “Imagery, of something beautiful in God’s world, like an ocean scene with waves coming in and out, which” is how the contractions are flowing in the body. Deep breathing is essential, it helps the muscles relax. And our muscles can work more efficiently when they’re well-oxygenated. It gives you more strength, more stamina, makes you feel more loosey-goosey.”

Though she knows “it’s a little out there for some people,” she advocates aromatherapy. “Lavender is very inductive of relaxation. Peppermint is good for revival, for stimulation. When she’s feeling too tired, like she can’t go on, let’s whip out the peppermint and give her some more oomph. It’s not magic, but I think it does help.”
Finally, she speaks of the emotional benefit of this particular physical pain. “I hate for it to sound kind of hokey or New Agey, but I think it’s very empowering for a woman to give birth on her own. I really believe it gives her a sense of ability in the rest of her life. When I have a difficult situation, like going to the dentist, or anything, I know that I have given birth, and I can do anything. I think it makes you a stronger person...you have this great ability to conquer your fears and your pains.”
We forgot the lavender and peppermint when we went to the Kaiser labor-delivery ward on May 6 of 1997. We didn’t do as much pain-management training as we should have. Deirdre vomited everything she ate or drank during labor, so the IV was necessary to prevent exhaustion and dehydration. But the nurses were good about letting her walk, keeping her on the monitor for about ten minutes an hour. As she lumbered around the halls in the labor-delivery ward, I wheeled the IV beside her, dropping to my knees when her contractions hit so that she could bend over and lean on me.
Deirdre was already at four centimeters when we arrived at around 3:00 a.m.; a few hours later, she was at six. Flint, whom we hired to serve as labor support, guessed that she still had a long way to go. But Deirdre’s curiosity got the better of her, and she opted for another exam around 9:30 a.m. To everyone’s surprise, and Deirdre’s surpassing relief, she was over nine centimeters; the certified nurse-midwife gave her the okay to push.
The bed was inclined into a semi-upright position and an overhead bar affixed to the sides. When she was pushing, Deirdre gripped the bar and squatted, shortening the birth canal and letting gravity lend a hand. Her voice went higher than I have ever heard it, a quavering roller coaster between moaning and screaming. Between contractions, she reclined on the angled bed. She came close to breaking once, and I had to play something of the heavy, holding to what we had decided, pushing her through her suffering. But she never asked for painkillers.
Part of what helped her was Paul’s line from Scripture about making up in our own bodies what is lacking in the suffering of Christ. She believed that her suffering could be efficacious, that it could be used to benefit others, in this case, her mother and her baby. She offered it up, a slightly different approach from Flint’s “leaning on God.”
When our son Finian crowned — when the top of his head began to press on the perineum — the midwife applied a warm compress and massaged the skin down around his head. Deirdre suffered a tiny tear, requiring one stitch. After the birth, Fin was placed on Deirdre’s stomach for a minute before being taken to a nearby table for weighing and examination. He never left the room, except when I took him to be circumcised the next day. Almost everything transpired as we had hoped it would, and the Kaiser staff were cheerfully accommodating.
Apart from the excruciating pain that Deirdre endured, we had a very pleasant birth experience, and Deirdre looks forward to giving birth at Kaiser again. But it doesn’t always work that way — hassles do happen. Though Flint can point to major improvements in doc-tor-Bradley patient relations — fathers in the delivery room, intermittent EFM, optional IV, optional episiotomy— she still sees a contrast in the way doctors and Bradley patients view birth.
“The doctor is there in case of emergencies; that is his forte. When the emergency comes, thank God he’s there.” The doctor, she says, drawing from her nine years as a medical assistant working with an OB, may be thinking more about preventing a lawsuit.
“Malpractice has really been the downfall of childbirth in this society. If the doctor feels he’s not able to do the things he wants to do for what he believes will be a more controlled, and in his opinion, safer birth—by constant fetal monitoring, by IV usage, and perhaps even C-section... [ If he does these things], he knows he did all the steps he could, by the book. If there is a bad out-come and the woman sues, then he can look back on medical records and say, ‘Well, I did everything I was supposed to do.’ ”
Increased worry over malpractice suits is not the only change doctors have had to endure. “In the ’50s and ’60s, nobody asked anything. You just were stuck. Then in the ’70s, women started to want their rights and wanted to know what was going on. Most women who are interested in natural childbirth are highly educated. It can be a little threatening to a physician — ‘Okay, what’s this woman going to want from me; what’s she going to do?’ ”
Flint tries to get her students to ease this anxiety. Besides employing the reassuring language of the birth plan, “I tell students to say, ‘This is what we believe in. We’re not going to ask you to do anything to endanger our child, we’re not that kind of people. We’re very reasonable. We’re going to do the best for — what we believe is the best for our child.’”
It’s a conciliatory statement, but there is still the tension in her self-correction: “what we believe is best for our child.” What happens when “what we believe” and what the doctor believes are at odds? “The doctor cannot force you to do any kind of procedure. They will just chart in your chart ‘Against medical advice’ to cover themselves.” I push, knowing that it is not always best to go to the hard case first, but curious where it will lead. What if the doctor believes the life of the baby is at stake, and the parents want him to stay out?
“I think it would be exceedingly rare,” opines Flint, “if it happened at all, that somebody went so far that they would not listen to what the doctor so strongly suggests. You’ll come to a point where you just have to believe that they know what they’re doing — more than you think. That is part of what I tell my students: you have to trust your doctor.”
Not everyone in the Bradley movement would agree. When my wife was pregnant and visiting her parents in Kansas City, she attended a Bradley class given by one of her parents’ neighbors. The last time she was there, she mentioned that I was writing this story and that I had interviewed Jay and Marjie Hathaway, executive directors of the American Academy of Husband-Coached Childbirth (AAHCC). The woman who taught the class then confided to Deirdre that Jay Hathaway was something of a crackpot.
Talking with Hathaway in his Sherman Oaks home, I could see how she came by this opinion. Hathaway is a layman who reads the medical journals — he calls it a hobby — an activity that arouses suspicion, like the man who spends all his time in the law library and tries to represent himself in court. “What is a nonprofessional doing snooping about in the professional literature?” the skeptic might ask. “How can he hope to understand what he finds, to draw the proper conclusions?”
Hathaway is given to incendiary statements, like “I used to believe that doctors didn’t know, that they needed to be told [about the risks of birth drugs]. But I’ve since changed my mind. I think they do know. I think they don’t care.” He is a man with an unpopular opinion — that the status quo about the tremendously important and intimate experience of giving birth is warped and dangerous — and years of combating the opposition of the medical establishment have taken their toll. He sometimes speaks with a peremptorily defensive manner, offering sharp comebacks to unspoken arguments that buzz invisibly about him.
But for all his vehemence and distress over the state of childbirth today, Hathaway is not a bitter man, not an angry man. He is a good-natured, comfortable father of six (three born with medication, three without), a friendly host, and a gifted storyteller. He seems to relish his role as medical maverick, taking comfort from history:
“I don’t know if you’ve read The Cry and the Covenant or know the name Ignaz Semmelweis,” he begins. “Semmelweis was an Austrian physician who discovered in approximately 1850 that childbed fever was caused by doctors’ hands. They went from an autopsy room, after examining a woman who had died of childbed fever, and they went down the hall, without washing their hands, and delivered a baby from some woman. This perfectly healthy woman was at enormous risk. Maternal death rates at all these big hospitals in Europe in the middle 1800s were between 10 and 30 percent. Today, women still die in childbirth, but it’s 1 in 10,000. They were enormous rates of death, and it was all from physicians. It was all because doctors weren’t washing their hands.
“Perhaps the most dangerous time in the history of the whole world to have a baby was 1850, especially if you were in one of the European capitals and went to a hospital. People at home weren’t having those kinds of death rates. People going to midwives weren’t having those kinds of death rates. Even the midwives within the hospital didn’t have those kinds of death rates.
“Semmelweis observed that doctors’ death rates were higher than midwives’, and one of the reasons he theorized for that was that doctors did autopsies and midwives didn’t. Now, this was an era when microbiology was not only unknown, it was disbelieved in. Pasteur and Semmelweis and all these pioneers, they were all in the middle 1800s. The whole knowledge of the human race about infection was turned upside down. Semmelweis tried to tell the doctors to wash their hands — if they would wash their hands, a lot of their patients wouldn’t die. And it was abhorrent to the doctors. They actually committed him to a psychiatric facility.
“He was just this crusading kind of physician. First, he started washing his hands. His patients didn’t catch this disease, which the teaching of the time said came from miasmas — clouds of death. Semmelweis said, ‘It isn’t a cloud of death, there’s something on your hands.’ He didn’t know exactly what it was.” He washed his hands in chloride of lime, and “he had, in his own practice, over 1000 consecutive cases without a single death at a time when other people were losing 10 or 20 out of 100.
“But the obstetricians of the time, and I have books even clear up into the 1920s, doctors were still arguing that Semmelweis couldn’t actually be right. Doctors couldn’t be the cause of the death of their patients, because they’re doctors. That mindset persists today.” By Hathaway’s own admission the maternal death rate today is minuscule compared o the 1850s, and most of the problems he sees with standard birth practices today do not have lethal consequences, but to him, the principle remains the same: Doctors refuse to change their behavior because they believe they are the ones who know what is best, regardless of what another doctor — in this case, Dr. Bradley—may say.
“Dr. Bradley’s basic premise back in 1947 was, ‘Nothing happens in nature without a reason. If something happens in a natural birth, there’s probably a reason for it, even if we don’t know what that reason is.’ That was profound. We have a lot of evidence today that we didn’t have then. Dr. Bradley wasn’t sitting there in 1947 saying, ‘In another 20 years, they’re going to start La Leche League — I better include breast-feeding. In another 30 years, they’re going to invent bonding, so I better do something about bonding.’
“His model was perspiring mammals. He grew up on a dairy farm. When perspiring mammals have a baby, they don’t have drugs, they don’t lie on their back, they aren’t restrained. The baby comes out, and the first thing every newborn mammal wants to do is breast-feed. Therefore, he theorized that it’s good for the baby to be held by the mother and to breast-feed.
“There was no proof then. There were no studies. Now, I can show you dozens, hundreds of articles on various aspects of the first few minutes after the baby is born and how important it is. He just said that if that’s what is natural, there must be a reason. I suggest that same philosophy should be applied to a lot of the things that are going on today.
“It isn’t as though the Bradley Method is a new thing that has to be judged by the current practitioners. It’s the standard against which you have to judge the interventions. An intervention, to be valid, has to have better rates of success than what would have happened with no intervention. There’s no sense in doing anything that isn’t going to make things better.” And as far as Hathaway can tell, the interventions, essential as they are in emergencies, rarely make things better.
Like anyone who spends time poring over reports and journals, Hathaway is a man full of numbers. “We’re 23rd in the world in infant survival. We’re doing more interventions, we’re using more drugs, we’re doing more cesareans. Our C-section rate nationally is around 20 to 25 percent. Just about a million cesareans will be done this year. You can’t do a million of any kind of major surgery without [risks]. In 1970, our C-section rate was 5 percent. We’re getting worse.”
More history and statistics, culled from a three-hour chat during which Hathaway slid easily from one topic to another, free-associating with the skill of a man intimately familiar with his subject: “Doctors love to point to the improvement in outcomes that has happened in this century, and it’s true. Early in this century was a dangerous, demographically speaking, time to have a baby. They claim they have been responsible for all of the improvement, and they claim that for all time up until then, it was always that way. True, there are many things today which are minor inconveniences, which a thousand years ago would have been fatal complications.” But it wasn’t “always that way.”
“In colonial New England in the 1600s, the average family had 7.1 children. Where did they get those children? The cesarean rate was zero, there were no epidurals, there was no stethoscope. Nothing your doctor has in his office had been invented in 1600, yet people had 7.1 children and lived to be roughly 70 years old.” Even for this century, Hathaway contests the notion that things have gotten dramatically better because of doctors’ interventions. “Doctors will point to graphs and say, ‘Look at the drop in infant mortality since the ’60s — we’ve dropped from 15 to 8.’ Yeah, but it’s 15 per 1000 to 8 per 1000. The overall infant mortality rate has fallen less than 1 percent, while the cesarean rate has gone from 2 percent to 23 percent. They point to this 1 percent drop and say, ‘This justifies doing a million cesareans a year.’ I don’t think it does any such thing.
“An awful lot of other things have happened in that era. When we had our first babies, in the ’60s, more than half the babies born vaginally in the U.S. were by general anesthesia. They don’t do that anymore. A lot of babies died from that, so when that went away, that was a big change.
“Plus, we have a weird new way of defining death. If you’re eight months pregnant and they do an ultrasound and they find out that your baby has no brain — if they do an elective abortion, that’s called a good outcome. It’s not an infant mortality. If you give birth to the same baby and then it dies, which it’s going to, that will be a bad outcome.
“In the first half of this century, more than half the babies born in the U.S. were born at home. It wasn’t until the 1940s that the number of hospital births exceeded the number of home births. The whole baby boomer generation was basically a hospital-born generation, for the first time in the history of the world. For right or wrong, the tail is wagging the dog right now; that’s the way everybody thinks is normal. Natural childbirth is thought of as an aberration, something weird.”
The Hathaways’ own involvement with the Bradley Method began in 1965. Marjie was pregnant with her fourth child. She tells the story: “I had already had three medicated births — knock-down, drag-’em-out obstetric routines. I kept thinking, ‘There’s got to be a better way.’
“Dr. Bradley came to Southern California, and we went to hear him speak. He said some interesting things. He said that women don’t need drugs to give birth to babies. I thought, ‘That’s insane.’ It hurt so bad with the drugs; how could he possibly say that women should give birth without drugs? Then he said that you should breast-feed the baby on the delivery table, and I said, ‘You can’t do that.’ I was always so groggy after giving birth, I thought the baby would fall on the floor.
“And then he says that you can walk out of the delivery room afterwards, and I was like, ‘Walk? Nonono.’ Because I’ve had births where I couldn’t walk for weeks afterwards. I can remember having to crawl on my hands and knees to get to the bathroom. He said, ‘You can get up and walk out of the delivery room, and then you go home two hours after the baby is born.’ This was totally unheard of.
“Jay and I talked about it, and we decided it couldn’t be any worse than what we’d already done. I went back to my doctor in the San Fernando Valley, and I told him all the things I wanted to do, and he looked at me and he said, ‘You’re crazy. No woman should give birth without drugs. No man should be in the delivery room.’ He didn’t agree with me about anything I wanted to do.” One Friday, her doctor examined her, told her she was at four centimeters, and said she’d have a baby that weekend. Tuesday morning, still pregnant, she boarded a plane for Denver, where Dr. Bradley practices medicine. The next day, she gave birth. “I didn’t require any drugs, Jay was with me the whole time, I breast-fed my baby on the delivery table, and I walked out of the delivery room.
“Dr. Bradley said, ‘Don’t come back to Denver every time you want to have a baby. Go to California and get something started.’ ” Using connections she had with La Leche, she began teaching interested people.
Jay Hathaway and the academy are the source for much of the information Nancy Flint offered, and I asked him about some of the claims she made, particularly with regard to birth drugs. The drugs and their effects —- stronger contractions, less pain — seemed to me the intervention most attractive to a woman in labor, and they are the intervention most strenuously opposed by Bradley supporters.
“Today’s drugs are still reaching the babies, and they’re still harming the babies,” begins Jay. “Even when they’re needed, you always have the potential for harm. There is a pamphlet that came out in 1974, and this is where a lot of people get the misunderstanding. They Said that regional anesthetics do not ordinarily enter the bloodstream and cannot reach the baby’s system. That’s a true falsity; it doesn’t enter the bloodstream, and it does reach the baby. In three to five minutes, it will transfer across the placenta into the fetus. That’s from the Physicians' Desk Reference.
“If you have any doubt about it, when you’re at a birth, watching them give an epidural, watch the fetal monitor. It’s immediate. The baby’s heart rate drops by about ten points almost immediately.”
When I ask about documentable problems that drugs cause for babies, Jay first cites the trouble breast-feeding that Flint talked about. The drug dries out the baby’s mouth, making it difficult for the baby to taste or smell Mom’s milk. “Oftentimes, these babies don’t want to nurse for at least three days,” says Marjie. This can interfere with bonding, as can the lethargy that comes with narcotics.
“Another problem,” says Jay, “is that the baby’s blood-brain barrier is immature. The blood-brain barrier is a kind of selective filter that your body has which allows nutrients and certain other molecules to get into your brain through the circulation to your brain more readily. It also prevents certain other things. If you give a woman in labor drugs, they may be getting to the baby’s brain more freely than to the mother’s brain.”
So what’s the danger? Jay Hathaway settles into another story. “Many years ago, there was a researcher named Yvonne Brackbill. One of the pieces of data that came out of her studies was that if the mother has drugs in labor, the baby’s IQ is three points lower. This maybe isn’t a huge amount; three points isn’t going to turn a genius into a moron. But I’d like my three points back.”
Brackbill’s results, which she called “conservative,” also stated the following: At 4 months, infants in the inhalant group [born to mothers under general anesthesia] “tended to laugh and coo less, had inappropriate placing and stepping responses, were less able to sit with help and hold their heads erect, and showed abnormalities in such physiological measures as heart rate, length, respiratory rate, blood pressure, and liver size.”
At 8 months, inhibited skills included “ability to respond to social play, sit alone, manipulate a bell, pick up a cube, and pull a string to obtain an object.” Tests at 12 months “revealed abnormalities in sweating patterns, locomotor and postural development, gait and overall neurological scores.” And in the case of Demerol, older children “are stunted in language and cognitive development.” (Quotes taken from an October 1978 article in Human Behavior.)
In 1979, Dr. Brackbill testified before a Senate subcommittee as to her findings. Hathaway, who attended the hearings, recalls that “the FDA’s first representatives were a pair of professional government research people. They had gone through the studies [that Brack-bill used as collaborative evidence] and found fault with every single one of these papers. ‘This study was not large enough; the control group wasn’t adequately controlled for this factor,’ etc. These were the only papers ever published in scientific literature on the safety of obstetric drugs.
“Yvonne Brackbill got up and basically, her testimony was, ‘Yes, each of these studies is in some way flawed.’ Her challenge was, ‘The overwhelming evidence suggests risk.’ Not one of these studies ever found a benefit of drugs to the baby. In every single case, they had found a deficit.” Brackbill’s study involved inhalant drugs used to put women to sleep during labor, as well as painkillers such as Seconal and Demerol. Epidurals generally employ bupivacaine or some other “-caine,” which carry their own risks. From a 1994 Chicago Tribune column by Doris Haire, president of the American Foundation for Maternal and Child Health: “A six-week follow-up evaluation by Deborah Rosenblatt in the United Kingdom of infants exposed to bupivacaine epidurals during labor demonstrated significant and consistent effects of the drug throughout the six-week assessment period. The initial effects were cyanosis (decreased oxygenation of the infant) and unresponsiveness. The infant’s visual skills, alertness, motor organization, ability to control states of consciousness and physiological response to stress were adversely affected.”
Further, a 1992 article in Developmental Medicine and Child Neurology summarized a study that examined the effects of bupivacaine epidural on infants’ performance on the Neonatal Behavioral Assessment Scale. “The epidural group showed poorer performance on the orientation and motor clusters during the first month of life.” Also, “Epidural mothers reported spending less time with their infants while in the hospital; post hoc analysis showed that they had longer labor, more forceps deliveries, and a greater amount of oxytocin [pitocin].... The results are discussed in terms of possible effects of the infant’s early disorganization on the mother-infant interaction.”
Finally, according to an article by Doris Haire in the spring 1987 issue of Childbirth Educator, “Epidural causes the pelvic musculature to become flaccid or limp, leading to dysfunction of the trough of pelvic muscles that normally rotate the baby into the proper position.” This may necessitate a C-section. Two studies conducted by Dr. James Thorp, associate director of maternal-fetal medicine at St. Luke’s Hospital in Kansas City, Missouri, concluded that women who receive epidurals are more likely to require C-sections for dystocia — the clinical name for bad positioning or a bad fit between the baby’s head and the mother’s pelvis. C-sections require general anesthetic, which brings us back to Dr. Brackbill’s findings.
Jay Hathaway admits the risks are small, that “bad outcomes” are relatively rare. But “even something that goes wrong one in a million times is going to happen two or three times a year. When you use any intervention which isn’t needed, there’s no benefit, so any risk at all to me is unacceptable.” Of course, Hathaway here and elsewhere raises the question of what “needed” means. Some women might argue that they need the drugs to kill the pain or help the labor; Hathaway is focusing primarily on the baby. Still, this doesn’t mean that he is ignoring the mother; he claims she faces risks as well.
“Everyone you talk to can give you a bad epidural story.” The sister of a friend of the Hathaways had a baby with an epidural. “It was one of the perfect ones. It worked great. There were no problems, no complications. The baby was fine. The mother was kind of shaky afterwards, which is not unusual. She didn’t have a headache; she was just shaking. They said, ‘Oh, that’s normal. Don’t worry about it. It’ll go away.’ Six weeks later, she’s still shaking, and her eyes are rolling back into her head. They sent her to a neurologist; he takes away her driver’s license and says, ‘These are seizures.’ She says, ‘Why am I having seizures?’ He says, ‘You had an epidural, didn’t you? I see it all the time.’ ”
Epidurals also increase the risk of postpartum fever. “If you’ve just had a baby, one of the things they do in hospitals is check your vital signs. If your temperature goes up, they assume you have an infection, and often, they separate you from the baby. It’s not particularly harmful, except that it interferes with the relationship with the baby. If the baby is withheld from the mother because of the fever, then it’s a bad thing.”
Besides epidurals, another possible cause Hathaway cites for the rise in C-section rates is the electronic fetal monitor. Here he supports the claim Flint made earlier. “When the EFM was introduced, the C-section rate was vastly lower. The first randomized controlled clinical trials ever done of fetal monitoring, done by a doctor in Denver named Al Haverkamp, showed a tripling of the cesarean-section rate. He had two groups: one monitored electronically and one not monitored electronically. The monitored group and the unmonitored group had the same rate of intrapartum and fetal deaths and damage. There was no improvement in outcome, but there were three times the rate of cesareans.” At least eight further studies have also concluded that EFM makes no difference in outcome.
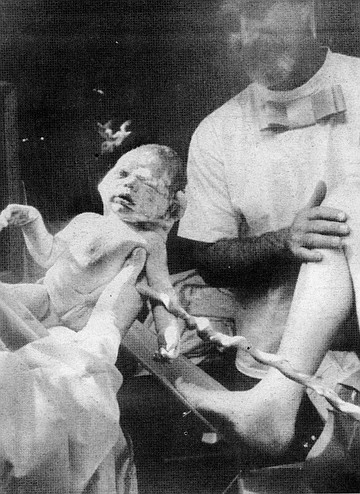
Hathaway is a man conscious of the effect he is likely to have on the listener, and so he is careful to make certain admissions and concessions. First, he grants that “No way am I an objective observer. I am a biased person, and I am putting my bias out front. But my evidence is not fraudulent. I did not sit at my computer and fake an article from some medical journal. They really came from their journals, but I’ve selected them with my bias. There are doctors who will come up with opposing articles, but they’re biased too.” (All articles quoted in this story are included in the The Bradley Method Teacher's Manual)
While admitting his bias, he tries to avoid being seen as extremist. “You can’t just automatically say, ‘Drugs are evil and bad.’ Some babies, if you let nature take its course, aren’t going to survive, or they’re going to get damaged. [Some of these cases] can be effectively and fairly reliably treated with drugs or surgery or intervention. There are babies who are fine, normal, healthy babies, who would have otherwise been dead or damaged kids.
“But we’re saying that the natural way of having a baby is the safest possible way for 97 percent of the people. If you take that diagnostic and treatment modality [that you apply to emergency cases] and you apply it to a hundred out of a hundred people instead of just one person out of a hundred, somewhere in that group is going to be some other baby that’s going to be harmed. A phrase Dr. Bradley often uses is ‘irreducible minimum.’ There’s an irreducible minimum number of complications for any procedure you want to mention.”
As Flint pointed out, the Bradley movement has achieved certain victories — fathers in the delivery room being an important one. Says Hathaway, “Dr. Marshall Klaus, years ago, did a study where he took a bunch of women who were in labor and assigned them someone to remain with them. The people were not medical people, many of them were not even mothers, but they were female. The results were dramatically better. The statistics were phenomenal in decrease in the use of drugs, decrease in cesareans, increase in the satisfaction of the mothers.
“Bradley observed the same thing. In 1947, he was assigned a population of women in his residency in obstetrics, and he was doing an experiment with these women, a pronatural childbirth approach. These people volunteered to be in this thing. He was, in effect, their coach. He would spend their whole labor with them, and they did much better.” At first, Bradley thought he was a great coach, but then it dawned on him that someone else could do what he was doing, someone like the father.
“The most stressful thing you could possibly do to a woman in labor is put her in a hospital room, connect her to a bunch of machines, give her drugs or whatever you’re going to do, and leave her all alone.” Hathaway sees this as the cause of “enormous increase in drug use and interventions, and pitocin, and cesareans, because the woman is frightened and abandoned at that moment in her life when she needs support more than at maybe any other time in her life.” And in the years since the Bradley movement began, fathers in the delivery room have gone from being a rarity to being the norm.
Of course, if your baby is born at home, the presence of the father is a nonissue, as are most interventions. Michelle Freund is a licensed midwife living in Oceanside who provides pre- and postpartum care for women who want to give birth at home, as well as supervising labor and delivery. She is not a Bradley instructor, but she does preach natural child-birth. She is a friend of Flint’s and she shares her Christian friendliness, but there is something a touch more bristly about her.
Her home testifies to her beliefs and interests. Amid the pleasant decor, I notice small statues of pregnant women; framed drawings of pregnant women, discreetly nude; a U-shaped birthing chair. Fertility — fecundity — in all its earthy, swollen fleshiness, is held in high esteem.
Like the Hathaways, Freund’s involvement with natural childbirth started with personal experience. As a result of preparation for her own labor, she decided that “it seemed the normal thing to have a natural childbirth.... I just felt like every woman that I asked that had given birth either had negative things to say or didn’t want to talk about their birth. So, I thought, ‘There’s something wrong here.’ ”
Though she had planned on having a home birth, circumstances necessitated her going to a hospital. “It really reinforced to me how important it was that women were supported, that they have advocates in the hospital, that they learned and educated themselves. So, that’s how I started.” In 1987, she began working as a childbirth assistant, “being a bridge between hospital staff and the client, so that they could work towards a natural birth.” But the work proved frustrating.
“I’ll tell you frankly, when I was starting out [between ’87 and ’90], if it wasn’t for those home births I would attend periodically, I would not have been able to keep going into the hospitals with these couples. I would feel as though I actually saw physical and emotional abuse occurring, and there was nothing I could do.
“I’ve seen some awful things happen. One doctor in this county — this was probably seven or eight years ago... There was this new amni hook, which is what you use to break the bag of waters. This woman had a birth plan, and she was doing great. She was probably seven centimeters, and we had just walked into the hospital, because we did labor support at home.
“This new amni hook, it looked like a finger condom, and on the end of it was a sharp point. They’re obsolete now; there was a problem with the little tips coming unglued. He comes in, already gloved up, which was really unprofessional to begin with — you don’t walk in from the nurses’ station with gloves on when you check a woman, you put clean gloves on right there in front of her. He had his fingers tucked in the palm of his hand, and he went in and broke her water and acted like he never did anything.
“He didn’t say he had it on, and then he carefully turned toward the trash can, rolled his glove off, and discarded it so we didn’t see it. But I did see it, and I went in and found it in the trash. It was really underhanded, and it had complete disregard for the woman’s choice and her written preference, which he had. They were his standing orders from her — completely disregarded.
“I don’t know his intentions, but the audacity to play God like that... It saddens me. I hope there are very few doctors like that. At seven centimeters, it may not be troublesome to break the bag of waters, but there’s no guarantee it’s going to help the labor progress. It’s a sterile environment, so it protects the baby from any bacteria we introduce via internal exams. It also acts as a cushion for the baby’s head and helps dilate the cervix. And with the bag intact, there’s less chance of cord compression— the cord can float around. The bag is there for a good reason, and there should be a good reason to break it.”
Besides that, “I’ve seen women yelled at. I’ve seen women given episiotomies when they said ‘Don’t cut me’ and the baby was not in distress. I’ve seen women be told not to push because the doctor wasn’t there yet, and she’s in pain and she wants to push — and sometimes when you don’t push and you’re holding that baby back, it will cause distress for the baby. I’ve seen women nurses come in and keep offering medication, when they’ve been asked not to offer medication, and say things like, ‘Don’t be a martyr, you don’t have to do this this way, what’s wrong with an epidural?’ I’ve seen nurses come in and never even look at the mother or touch her, just push the button to get blood pressure, chart notes, and walk back out.
“I’ve seen babies whisked away unnecessarily. I’ve heard doctors railroad women into cesareans when they’re not necessary, making them feel hopeless, saying things like, ‘What do you want? Do you want a healthy baby?’ You know, Let s just get this over with’ instead of ‘These are the things we can do, and this is what I recommend.’
“Most women giving birth do whatever they’re told to have a healthy baby. But intervention doesn’t guarantee a healthy baby. There’s no guaranteeing with a cesarean that you’re going to get a healthy baby. I’ve taken moms in for cesarean, baby and mom were in great shape. By the time the doctor got there to do the cesarean — she just kept waiting and waiting—and the baby crashed during the cesarean. They drew it out and it took about see minutes to revive it.”
In spite of her experiences, she insists that she is “not antihospital or anti-doctor. I am against misusing technology.” For example, Freund once provided care to a woman whose pregnancy had gone to 43 weeks. She and the doctor she used as consultant were both concerned, and the doctor recommended a nonstress test to see if the baby was still healthy. The woman, opposed to intervention of any kind, refused. “I wish she would have done the nonstress test,” says Freund, looking back. I think it was harmless, but she was adamantly against it. I thought it was a good piece of technology to use at the appropriate time to assess the wellbeing of the baby.” As it turned out, the baby was fine.
But what if the baby hadn’t been fine? Mothers have been prosecuted for abusing babies in utero by drinking too much; could she have been prosecuted for some kind of neglect? Flint, Jay Hathaway, and Freund all admit that interventions are sometimes necessary for the health of the baby. But what happens when Mom refuses?
Freund supposes that “someone could try to bring up charges against her, because my doctor knew full well, and I knew full well, that she didn’t have the nonstress test. We had documentation.” But, she says, “at this day and age, if you can kill a baby in utero because of Roe v. Wade, then why should she be prosecuted for not choosing a piece of technology?”
Legal issues aside, Freund does not assume absolute neutrality. She told the mother, “ ‘Please think about how you might feel if your baby died in utero and could have been saved had you had the nonstress test.’ I have to feel like I’ve told [a woman] all the risks, and given her all the facts, and also will encourage someone to call and discuss it with the consulting doctor. I’ll say, ‘I think you need it.’ I’ll say that.”
Still, she says, “My perception of a good provider is, less is more. You want to inform them and give them all the standards of care and help them make educated choices, but we have to remember that we’re in bigger trouble if we make the choices for them. They’ve got to make the choices. Probably, if we’d stayed along those lines all along, there wouldn’t be the malpractice fears that there are today. I think that’s probably why midwives get sued a lot less, because they’ve got a great rapport with their clients, and they have their clients assume responsibility for making choices by giving them full informed consent and full disclosure and letting the couple determine what they want.
“I’m against coercing people to do things that might not be in their best interest but in the best interest of malpractice insurance or someone else’s agenda. I believe we need our hospitals, because we need comprehensive care should it be necessary. But the majority of women don’t need that kind of care. However, the majority of women choose that kind of care.
“It’s not the doctor’s fault. The feminist movement in the early 1900s said, ‘We can have painless childbirth, so we demand our Twilight Sleep [a general anesthetic].’ The women’s movement was the beginning of the end for natural childbirth.” Women who could afford painless childbirth went to the hospital and got it, while those who could not gave birth at home.
“Hospital birth gave you status, because rich people were having babies in the hospital.
“Then, it was the passive woman who said, ‘Well, here I am, doctor; do something for me. I’m paying you, so do something.’ ” But some people, “educated middle-class people,” still sought out midwives. “Midwives were underground for a long time. It wasn’t until, I think, 1955 that they started certifying nurse-midwives.”
Now, “there’s several routes you can go,” explains Freund. “The most traditional is apprenticeship, and that’s how midwives learned throughout the centuries. They would go with their mother or their auntie or whoever was the midwife, and they would go to the births and just learn. When that woman was too old, she passed the obligation to the younger person. There was always a village midwife somewhere.
“In today’s world, when you say ‘traditionally trained,’ you’re thinking the most mainstream training: becoming a registered nurse, taking a three-year midwifery program, and getting your certification as a certified nurse-midwife. Currently, the majority of certified midwives in California are certified nurse-midwives. However, the majority of those nurse-midwives work in an institution, be it a hospital or birth center.
“My personal opinion was that birth wasn’t an illness,” says Freund, “so it really shouldn’t take place in a hospital. I’m not learning about how to take care of somebody that’s sick. This is a normal physiological process; I’m learning how to take care of a natural process.”
So, after attending 38 hospital births as a childbirth assistant, she took what she considers the traditional route of apprenticeship. “I worked for three years from 1990 to ’93.” During that time, she assisted at “close to 200 deliveries. My third year, I did an internship with my midwife.” As an intern, Freund began taking on clients under the midwife’s supervision. “She is now licensed but was not at that time. She had 18 years of experience when I started working with her.”
In October of 1993, the California legislature passed the Midwifery Licensing Act, whereby midwives who are not nurses can become licensed if they take a three-year accreditation program and sit the state exam. The program involves “three mechanisms. Your clinical numbers — how many prenatal visits, newborn exams, deliveries, and labor managements you’ve done. Those charts need to be evaluated by an ob-gyn and a certified nurse-midwife and signed off.”
The charts are then submitted to the school (in Freund’s case, the Seattle Midwifery School). The school calls the patients to verify the data. The second mechanism is the school’s exam; the third is a clinical evaluation. “You have a doctor or a midwife sit in your clinic, making sure you do correct history intake, you inform the patient about nutrition, support, emotional support, and whatnot. You do an initial history intake, a First-trimester mom, a second-trimester mom, a third-trimester mom, a newborn baby, and a postpartum. Then you are evaluated on a simulated delivery of a baby and a placenta, a baby with a cord around its neck, and a simulation of an emergency pitocin injection and sterile technique and suture.”
For the simulated birth, “Most midwives have [artificial] babies that have the bones and stuff on the head.” Freund, who has served as a supervisor since becoming licensed in 1996, owns “an anatomically correct pelvis, and I also have membranes and a placenta, just made of fabric and cord. But for most people, you could do it as rough as pushing a baby through a piece of foam with a slit in it,” and pinning a piece of cord to the baby and a sponge-placenta.
The pitocin injection “is usually done on an orange, and the suturing is done on foam. I use markers and color the tissue” to indicate which layers are being sutured. It’s funny to think of a state license being given based partly on work with foam and oranges, but it seems to support her claim that managing birth does not require the depth of knowledge associated with most medical procedures.
After the clinical evaluation, “you can sit for the state exam” and become a licensed midwife. The obvious question is, how do you get the clinical numbers for the first mechanism if you’re not licensed? “If you’re not licensed, the only way you can get those numbers is to do it as an unlicensed practitioner. You can do it under the supervision of a certified nurse-midwife or doctor. A lot of midwives did work with licensed doctors years ago in this community. Today it’s a different story.
“We were all practicing without a license, and some have done it for 20 years. We did births because we believed in it, and women were going to give birth at home with or without a doctor’s permission. Eventually, they got off their butts and worked toward getting us a route by which we could be licensed, but we still had to be the guardians of home birthers, who were not going into an institution to give birth.”
Today, “there are still lay midwives practicing that don’t want to get licensed. We’re hoping that more will come forward and get licensed so that there is some type of regulating body for us. There wasn’t a regulating body, but I think that a lot of us, including myself, felt that this is what we were called to do. We had the skills, the training — the state needed to provide that [body]. So while I was waiting for them to provide that, I was practicing.
“I feel like it’s a calling for me. That’s one of the reasons I moved forward in midwifery without my license. I’m doing it in a very responsible way, whether or not I have that license. I had all the knowledge I needed to practice safely, to give good care, and my outcomes were fabulous. Today, I have very good outcomes. I have a very low transport [to hospital] rate; it’s less than 5 percent.”
Wasn’t unlicensed practice illegal? “It’s illegal to practice medicine without a license. However, the practice of medicine and the practice of midwifery can go side by side without crossing over.”
What if a medical emergency occurs? “You’re damned if you do and damned if you don’t. If I said, ‘I’m doing midwifery, but I’m not going to practice medicine,’ that means I shouldn’t use needles or tell somebody what to do for their kid. I can only give the things that I would do. But if you were doing midwifery without a license, and there was an emergency and you didn’t act appropriately, then you would be held more accountable than if you did the appropriate thing and practiced medicine and got the best outcome. That’s your responsibility. You take on the yoke of working with [moms in labor], then you darn well better be doing everything you can.”
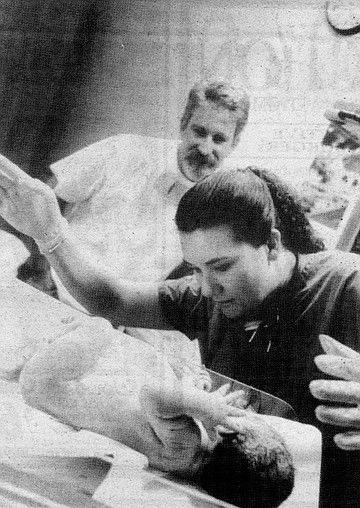
Unless she transports a patient to the hospital, she is that patient’s primary care provider from pregnancy to postpartum and newborn care. But it’s labor that attracts the attention — it’s not hard to imagine other kinds of care occurring outside the hospital setting. I ask her to describe a sample labor.
“After all the prenatal care, and after doing a home visit where we check for supplies, test our pagers, check our maps to the house, and meet everyone who’s going to be at the birth, the client calls, says she is in labor. My fully trained assistant and I arrive. Mom might be in the tub or lying on the bed or up walking. [Besides the advantages Flint attributed to movement, Freund says that changing movement frequently “gives the baby an opportunity to move and mold and adjust to the pelvis and make its way through.”]
“Meanwhile, I would immediately listen to the baby with a Doppler or a fetuscope and check Mom’s vitals. My assistant would start setting up for the birth. Eventually, I would do an initial internal assessment to see what kind of dilation is happening. Often the woman is well progressed. Mom’s either up walking, alternating with lying down on her side resting; she might be in the shower. One woman would go from sitting to hands and knees, then to her Jacuzzi, then squatting. Then, settling down into my birth chair to push the baby out.”
Not that everyone has to use the birth chair. “If you leave her alone, a mother will more than likely automatically choose the best physical position for her.” Some give birth in the tub, some on their hands and knees, some squatting.
“Usually, there’s nice music. There’s usually a mother or two, or family members or a couple of friends. Some women will have a masseuse or an acupuncturist there to help them along with labor. There’s always a lot of women. Women like to invite other women to their births, just for the nurturing.
“Either Dad catches the baby or I catch the baby. We put the baby on the mother’s chest. There’s a lot of tears and joy and laughter. My assistant is there watching the baby, making sure the baby has good heart rate and respirations, good color. I’m watching the mother, checking her fundus because we still have to deliver the placenta. Hopefully, we get the baby on the breast to cause uterine contractions, and that causes the placenta to detach and deliver.
“Either Mom wants to get up and shower, if she’s strong and stable, or we clean her up and tuck her into bed and monitor her throughout the time the assistant is cleaning up and they’re bonding.” The baby gets an exam, everyone gets something to eat, and then everyone goes to bed.
So goes the sample, what about the 5 percent that need to go to the hospital? When does that happen? “If I thought that Mom was getting exhausted and progress is slow.” Exhaustion can bring on “lack of mobility, dehydration, they start to burn their fat stores. If the mom gets exhausted, sometimes the baby gets exhausted. If the mom gets dehydrated, the baby can spike a fever. If a woman’s vomiting and she can’t keep any fluids down, and she’s got this long, laborious labor, she’s not going to be in good shape.
“If I listen to contractions, and after contractions, to see how the baby’s heart rate is, how the baby’s heart rate responds to contractions — and mostly it’s always beautiful — if there’s something there that I don’t like, if there’s deceleration, then I’m going to listen more carefully and make my assessment. I might change the mother’s position. I might give the mother oxygen. I might push the baby against the pelvis. Different things to see how the baby responds. If there’s fetal distress, then I’m going to call the hospital and explain to the parents and move into that setting. I’m not hesitant to transfer when it’s needed.”
I can’t help it; I keep thinking about the pain. I keep thinking that the pain is the sticking point, the obstacle that would keep a woman from considering natural childbirth. What do you say to that? “This is a natural physiological function,” responds Freund. “Your body was designed to give birth. It doesn’t have to be painful. The more educated you become, the more you trust and understand the process, the less painful it should be. So if you exercise, you educate, you eat well, you look forward to the birth, you should have a nice, natural birth.”
It doesn’t have to be painful? “The pain is a process that reminds you of what you’re doing. It helps you grow. I’ve been to support groups for women who have had cesarean sections, and they have a huge loss, because they didn’t experience the birth of their baby. And most American women don’t, because they’re on an epidural. I think that we’re all into this fast-food, express this, express that, let’s just schedule my baby and get this over with kind of thing, because we don’t have time for unplanned, spontaneous things.
“It brings us to our natural limits. Women will say, I’ve never done anything as hard.’ Well, what’s wrong with that? Empowerment is what you get when you birth your baby naturally, and you lose your power when you give up that right to a natural birth.”
Like Flint, Freund is a Christian, and when dealing with Christian patients, she invokes their common faith. “You talk about trusting God, knowing that He won’t give you any more than you can handle, surrendering, being the empty vessel, bringing forth His blessings, all those things. You talk about Philippians 4:13: ‘I can do all things in Christ Jesus who strengthens me.’ Visualization, seeing Him, seeing yourself in the palm of His hand, or cuddled up in the arms of Jesus, things like that, where they can have that kind of thing to grasp on.
“The majority of those certified nurse-midwives work in an institution, be it a hospital or birth center.” Freund may be right in saying this, but that is not to say that a hospital and a birth center are the same. During our interview, Freund pointed out that some hospitals are dressing up their labor-delivery wards to look like bedrooms, to make the mother more comfortable. But, she said, if the doctor is still an interventionist at heart, the dressings are superficial.
The dressings are there at Best Start Birth Center on Fourth Avenue in Hillcrest, but the homey atmosphere does not mislead. Janet Cunningham and Roberta Frank, both certified nurse-midwives, believe wholeheartedly in natural childbirth; their professional liability insurance requires that they work here in the center. They also like that they are hospital-close in case transport is necessary— Mercy is just down the street.
Freund showed me some pictures of labors when we spoke. One stuck in my mind: a photo of a woman, naked from the waist down, seated on the concrete of her patio, back against the wall of her house. Her knees were drawn up and spread apart. Her head was tilted back, eyes closed. A long, liquid trail flowed from her vagina across the concrete patio; her water had just broken. The photo was arresting; my wife gave birth naturally, but not this close to nature. Not all of Freund’s moms deliver this way, but I wondered if maybe the institutional setting of the Birth Center might be a sort of middle ground between the hospital and the home, appealing to a greater range of people. Freund might argue that I was institutionally tainted — that I viewed it as a more secure, safe place than home, when home is the real paragon of security and safety—and maybe she would be right. But I’m also right about the broad appeal of the Birth Center.
“We have moms who home-school their children,” says Cunningham. “We have moms who go right back to work. We’ve got women who drive trucks, who are attorneys, who work in medical offices. We have women of all races; we have women who are Muslim and real fundamental Christian religions. It’s just so fascinating. They’re here because they believe they’ll have a better experience. I think they just trust nature.”
Cunningham and Frank share Freund’s view of intervention: “I think that doctors interject a lot more than they should into the birth,” says Cunningham. “It’s a natural process. That’s kind of the culture of medicine. We’re actually seeing a little bit of theoretical work done, research. It’s like a cascade. You do one procedure, whether it’s EFM, and then you don’t know if you might need a C-section, so we’re not going to let the mother eat anything. So we have to give them an IV.
“While the nurse is with another client, or if she just doesn’t want to labor sit — you can’t always expect the dads to be there — maybe she chooses an epidural when all she needed was to be able to walk around and have somebody rub her back and tell her that she’s doing a beautiful job. Then with the epidural, maybe the blood pressure goes down even though they gave her fluids, and so you can end up with the C-section. All the things they do can sort of cascade and you end up with an outcome you never would have expected, and then the attitude is, ‘Oh, isn’t it wonderful that we have our suites right here and anesthesia right here.’ Maybe if they weren’t right there, things would have been different.”
As evidence, Frank tells this story: “I’ve had two people come to me and tell me about their past birth experience where the doctor has said that the baby’s probably too big and won’t be able to fit through. I think they ended up getting induced or having a cesarean section, and the babies weighed less than my son — he was eight pounds, nine ounces — and they had bigger hips than I do. I just feel like, a lot of times, it’s scheduled because it’s more convenient for the doctors. I don’t know if that’s true, but... ”
Cunningham concurs. “We see that in our practice all the time — a woman wants a vaginal birth after a previous section. A catchall reason for doing a cesarean is ‘failure to progress’ or cephalopelvic disproportion. Then, lo and behold, she has a successful vaginal birth after cesarean, and the second baby is bigger than the first. A lot of it has to do with geometry. A large baby that’s lined up well will usually fit through. We encourage moms to be up and moving. Elastic binders can sometimes help, especially if it’s baby three or four and the mom’s just kind of pendulous, and the baby’s just hanging out there. Cinching the baby up gives you a good drive angle—it’s so old-fashioned, so low-tech.”
“There’s a lot of old tricks that have been forgotten,” adds Frank. “When birth became technical — when women were confined to bed and wearing monitors and the C-section rate went up — physicians became really good surgeons, and their expertise wasn’t as good at supporting normal birth. My mother was an OB nurse in the ’40s, and I have her old textbook. There’s a chapter on position changes the mother can do to turn the baby.
“Sometimes, they’ll schedule a C-section if the baby’s head is overriding the pubic bone. They’ll say the pelvis is too small. But in my mother’s book, there’s a picture, it shows specifically a position the mother can assume to rock the head below the pubic bone and into the pelvis. We did it, and it worked.”
More low-tech intervention: when Cunningham gave birth to her own son here, “I was pushing, and in the last stage of pushing, we were getting some moderate decelerations of his heartbeat. At one point, the concern was, ‘Are we going to transfer to the hospital?’ I was in a full squat — really using gravity to bring him down — but in between [pushes], Roberta pushed his little head back up to get some of the pressure off
“I really believe that if I were in a hospital, I probably would at least have had a vacuum extraction, and I would have had a cut from here to there, maybe. If we needed to transfer, we would have, but if it had been in a hospital, I really don’t think an OB would have thought to push his head back up. I remember thinking, ‘Oh, he’s going the wrong way,’ but it worked. It relieved the pressure on his head, and he was born just fine.”
Transfers are sometimes necessary—they estimate about 12 percent — especially for first time moms exhausted from long labors. “That’s when the hospital really helps,” says Frank. “That’s when an epidural really helps. Mom goes in and she can sleep for a couple of hours, not have any pain for a couple of hours. After a good sleep, labor usually rallies, and she’ll go on to have a vaginal birth. That’s a good use of the system. Let everybody try normal, and if normal isn’t working for them, then rely on medicine.”
The problem, as Hathaway pointed out, is that “normal” no longer means “natural.” Cunningham used to work as a labor-and-delivery nurse at Ohio State. “I got subsumed into the culture. I heard OBs in labor and delivery say, ‘Birth can only be normal retrospectively.’ ” Columbus, Ohio, was a town in which it was easy to get sued _ “they have the second highest per capita population of lawyers in the country” — so doctors had to be careful, and that meant intervention. “Everybody had monitoring, and there was a high C-section rate. One thing that really disturbed me was a woman, uncomplicated, normal healthy labor, had an elective epidural for pain management. We did everything right, but her blood pressure bottomed out, and the baby’s heart rate bottomed out. The anesthesiologist gave her fluid and some medication. Her blood pressure came up, but the baby’s stayed down.
“There was a mad dash to the OR. We had to do a crash section, and of course you had to have general anesthesia. I’m with her in the recovery room and she’s asking how her baby’s doing, and her baby was fine. She’s thanking the OB and the anesthesiologist for saving her baby’s life, and everybody’s eating it up, saying, ‘We’re glad to be here. This is why hospital birth [is good].’ Nobody told her that it totally happened because of the epidural.” Drug dosages have since been decreased, but the story stands as an example of both the “cascade effect” of interventions and the interventionist mentality the women oppose.
Frank “tried to work in a hospital, but I just couldn’t do it. I couldn’t support the system at the expense of the client. You’ve got so much work that needs to be done, you have to document.. .you find yourself doing things for no other reason than it comes from the administration that you have to do it. It doesn’t matter that it doesn’t fit any of the people that are there having babies.” She did have a hospital practice as a certified nurse-midwife, along with three others, “for about sue months, back in 1979. The administration at UCSD Medical Center thought we were a great idea and gave us all privileges right out of school. But the OB department and the anesthesia department had different ideas. We found out we couldn’t practice midwifery there. I think they were afraid we were just too controversial. Things were going well; they liked things just the way they were.”
When hospital transfers do occur, Cunningham and Frank call on Dr. Dale Lapp. Though he looks like any other doctor (I was expecting maybe a wild-haired madman?), he does not fit the intervention-minded doctor image I had been given. Rather, he is what proponents of natural childbirth wish for, a man willing to intervene if necessary but who says, “We have all the high-tech hospital things available if they’re needed, but the fact is, a lot of the time they’re not. It seems like women who do natural childbirth — without anesthesia — have just a little bit better experience, a little bit easier recovery.”
When I ask Dr. Lapp for his take on the pain question, he responds, “There was a study done on women who wanted to deliver without anesthesia. They did psychological testing to just evaluate how sure they were they could do that. The women who were very sure they could do it, that had the right attitude, almost all of them did it. The ones that asked for anesthesia were the ones that weren’t really sure they could do it.” While he lacks Hathaway’s outrage regarding drugs, he does say that “anesthesia drops blood pressure, and that can reflect in fetal heart tones,” indicating fetal distress. “It takes away the urge to push, so sometimes the second stage of labor can be prolonged, and that can really tire the mother out. My sense and my experience is that, if you meddle too much, that’s where your complications come from.” What he says is not new to my ears, what is new is that I am hearing it from a doctor.
This story by no means provides a complete account of the natural childbirth issue. Nor does it address all the issues doctors face — insurance and malpractice issues, issues of time and space in hospitals, and the like — in any great detail. It is also admittedly one sided — no pro-intervention doctors were interviewed. But, as Jay Hathaway said, “The current power structure is so large, it’s like some enormous ocean liner. I’m some guy in an itty-bitty rowboat saying, ‘Turn the Titanic around, and keep away from that iceberg.’” Intervention is the standard; this story is intended to give voice to those who propose an alternative.

When the first hard contraction hit my wife Deirdre, buckling her at her middle and squeezing from her lungs a shocked cry, her first thought was, “I don’t know if I can do this without drugs.” Her second thought was, “I don’t know if I ever want to do this again. She did it—gave birth—without drugs, and she does want to do it again—without drugs.

Looking back on our decision to deliver naturally— letting nature take its course as much as possible, without intervention — I can recall only a vague certainty that it was the right way to go. The vagueness didn’t make my certainty any less certain — I had a strong gut feeling, a conviction — but I couldn’t give much of an accounting for it. My sister-in-law had delivered naturally and was a strong advocate. But I wasn’t exactly sure of her reasons.
Deirdre had a clearer idea. “It seemed right, first of all, that you don’t take drugs, so the baby doesn’t get the drugs. The baby is much smaller. And I had heard there were side effects — sometimes the baby has trouble nursing, sometimes the mothers have headaches.
“And I wanted to experience childbirth. I really did want to feel the baby being born, even if it hurt. I wanted it to be a good experience too. Also, I was afraid of drugs; some other women I knew had bad experiences. They were going to have children again, but they were afraid.”
“I felt like I had been hit by a Mack truck,” said a friend who had received pitocin, a drug that stimulates contractions. “It was the most horrible experience of my entire life.” Her second child was born at home, naturally, and Deirdre characterized it as a serene, relaxed, wonderful thing — “like night and day.” She knows other women who recalled positive experiences with drugs, but she still wanted to go natural.
Several months into Deirdre’s pregnancy, we started attending a Bradley Method birthing class, led by Nancy Flint. The method is named after Dr. Robert Bradley, author of the seminal work, Husband-Coached Childbirth, but it is not so much an esoteric method developed by a doctor as a policy of cooperating with nature.
Because such a policy often conflicts with the standard practice of most hospitals, Bradley people have something of a reputation as fanatics. Flint, on the other hand, is just the sort of person you would want to introduce it to someone. She is unthreatening, unmilitant. She has given birth both naturally and with drugs — concern for the baby’s health after a car accident led her to accept a pitocin-induced labor, but she declined painkillers. She has worked with an obstetrician and as a doula, or labor assistant.
Her North Park home, where she teaches her class, is cozy and bright, stenciled and knickknacked. Her features are soft and friendly; her manner, nice with a hint of businesslike efficiency. She is not above making a strong statement — “My very blunt view of women taking medication despite the fact that it can harm the baby is that it’s very selfish,” she says — but in general, she is looking to avoid a fight. This is not always easy; Bradley students are often thought of as people who are suspicious of doctors and who try to buck the system.
“In the last couple of years or so,” admits Flint, “I have started telling my students not to really advertise themselves as Bradley students; rather, as natural child-birth students. Something other than the Bradley name, just because of the negative connotations that go with it. When I was in labor and they knew I was a Bradley teacher, that’s what they put under ‘Problems with patient.’ That was my one problem. They sort of assume that the person is going to give them a hassle.”
Hassles do happen. Flint remembers a man who pushed a doctor away from his wife because he didn’t want her to stay in bed and be monitored. The man was restrained and removed from the room. “It’s only been one person in a hundred, but that’s the one person that doctor will remember forever, that this Bradley stuff is horrible.
“Trust is the big issue. They feel like they’re not being trusted if everything they do is questioned.” So, Flint counsels her students to try to establish trust within the context of the birth plan, the list of things the couple does and does not want during the birth. This is the plan we submitted to Kaiser, signed by ourselves and our certified nurse-midwife:
Birth Plan
We, Deirdre and Matthew Lickona, would like to cooperate as much as possible with the professionals who will be aiding Deirdre during her labor and delivery. We would also like Deirdre to deliver as naturally as possible. To minimize tension between these two desires, and to indicate our wish to be both flexible and responsible in working with Kaiser Permanente, we have prepared this Birth Plan. We would like Deirdre to deliver under the following conditions:
Mobility — we would like Deirdre to be able to walk freely during labor. This includes use of the shower.
Minimal electronic fetal monitoring [EFM] — to enhance mobility, we would like to limit use of the EFM to no more than ten minutes per hour.
No routine IV — we would prefer that Deirdre not receive an IV and that she be allowed to eat and drink during labor instead.
No medication — we would prefer that medication not be offered except in an emergency.
No frequent exams — we would prefer that Deirdre not be examined unless necessary.
No episiotomy — we would prefer that Deirdre receive no episiotomy and that massage and/or warm compress be used instead. If it comes to a choice between cutting and tearing, we would prefer to let Deirdre tear.
Upright position — we would prefer that Deirdre not be flat on her back during delivery. Rather, we would like her to be sitting up.
No separation — we would prefer that Deirdre be given her baby immediately after delivery for breast-feeding and bonding and that she not be separated from her baby at any time.
Because we want our baby to be as healthy as possible, we will of course be flexible on these conditions should complications in birth make it necessary. We have faith in the competency and professionalism of the Kaiser staff, and should complications arise, we would like to be informed so that we may discuss the choices to be made and determine a new plan of action.
Thank you for your understanding and cooperation.
Our requests reflected the basic tenets of the Bradley Method. I asked Flint to comment on each. Other people I spoke with for this story treated some of the things she talks about in greater depth and detail. But what she said, I think, serves as an adequate introduction to some of the issues associated with the method.
Movement: “It speeds labor. It makes it progress at a regular pace. If you stay in bed, labor tends to go very slowly; it does not progress. Therefore, if there’s failure to progress, they have to start using pitocin. But movement is a natural way to keep labor going at a normal pace, to keep the cervix open, to keep the uterus contracting. Gravity is the number-one factor, and it keeps all the muscles working rather than just being latent in bed. It just makes sense — feels better too.”
Limited electronic fetal monitoring: When you’re on the monitor, which measures the baby’s heart rate, you have to be lying down. Limited monitoring allows for movement. Further, research has shown that “electronic fetal monitoring leads to more C-sections than are necessary, and it doesn’t necessarily lead to a healthier outcome — it’s the same with or without it.” No routine IV: Though movement is possible with an IV, it’s cumbersome. “Just being stuck with an IV can be painful and uncomfortable, intrusive to your sense of peace and calm. Instead, let’s drink fluids and we still get the same benefit.”
No medication: When I asked Flint what natural childbirth is, her definition was negative, defined against what she sees as the current conception of normal birth practices — “No intervention. No drugs, no medications. Nothing other than your own power.” Everything on the birth plan falls under the category of “No intervention,” but what comes first to Flint’s mind, what is most important, is drugs.
The two kinds of drugs Flint mentions are pitocin, which augments contractions, and narcotics, which kill pain. The narcotics are often administered through an epidural in the mother’s back. “According to the AMA,” says Flint, “there is no known drug safe for the fetus. So why would you use them? Opponents say, ‘Well, the odds are so long that something could go wrong.’ But that’s still a risk I just find it odd that women are so careful during pregnancy to not take anything, but suddenly it’s okay when you’re in labor.
“There’s evidence to show that some birth drugs remain in the baby’s system for up to seven days. They cause bonding difficulties, the babies are not able to focus as well, so the mother-infant bond is delayed. They are very lethargic. The sucking mechanism is very frequently interfered with, and therefore breast-feeding becomes very difficult.
“There’s always the risk to the mother too. We don’t know if she’ll have some kind of allergic reaction to these drugs. Some women have been known to have heart problems. She’s in trouble, they have to have a C-section, it gets complicated. Yes, it’s all rare; yes, it’s probably a minor effect on the baby, but we’re not sure. There’s some evidence stating that learning disabilities may be caused by birth drugs. There’s not a lot of financial backing of research to prove these facts, because everybody says, ‘I was born with drugs, and look at me, I’m just fine.’ But why are we doing this? Why are we taking these risks?
“In other countries, they do not use birth drugs. They have midwife delivery, and physicians are there for emergencies only, which is always the way it was supposed to be. They have much lower infant mortality rates. There’s a very large study that’s come out of Dublin that compares midwifery to American obstetrics. Their first-time mothers give birth in 5 to 6 hours, our first-time mothers in, like, 12 to 18 hours. They attribute that to the one-on-one, woman-to-woman care, and plus, they are not offering all the drugs.”
No frequent exams: Flint didn’t comment much on this one, but from my conversations with people associated with the Bradley movement, I got the impression that exams were seen as a doctor’s starting point for intervention. If a doctor checked a cervix and found it the same size over a three-hour period, he or she might conclude “failure to progress” and recommend pitocin to get things going. Or an exam might lead a doctor to think that the head was too big to fit through the pelvis, necessitating a C-section.
Their response to these sorts of conclusions was that one labor is not like another. One woman’s cervix might open steadily, another’s might stall at five centimeters for several hours, then open to eight or nine centimeters in a very short time. If she had waited that extra hour, pitocin might not have been necessary. In the case of the big-headed baby, “hormones and enzymes are released constantly in our body that are allowing the pelvis to move out easier. It may appear [that the head is too big for the pelvis] because they don’t allow time for the pelvis to open up.” There is a general faith that nature will take its course in most situations, but not according to any particular schedule.
No episiotomy: “That’s a very controversial issue. You’ll read all kinds of things on both sides. But in our experience, what we have seen is, number one, a surgical cut leads to weakened skin tissue. Therefore, the cut often leads to a bigger tear, so you’re going to be opened more than you would have been on your own. Two, it heals much slower than a tear. It’s a very painful healing process.
“The controversial part is that doctors are taught to believe a cut will be easier to repair in sewing up than a tear, and other people believe that a tear is easier to repair than a cut. I always use the analogy of a puzzle piece. Puzzle pieces lock together perfectly, whereas, if you put two straight lines [flat surfaces] together, there’s nothing to link back together again. So in my mind, a tear would heal — and be able to be repaired — better, easier, faster.
“I’m blessed enough to have had both experiences. The first one, I had a huge episiotomy. They said the baby was in trouble and they needed to get her out. I don’t think they even asked me, they just did it. It was enormously painful afterwards. I couldn’t sit down without pain for six weeks. Sex was incredibly painful for a year. I think they cut way too far, and the repair and the healing took way too long. The second time, without an episiotomy, I had almost no pain afterwards, could sit down normally, and felt perfect after three weeks.”
However, as with other interventions, her opposition is not absolute. “If somebody were to say to me, ‘Okay, your baby’s in trouble, do you want to be cut or do you want to wait and see what happens?’ I’d say, ‘Yeah, cut me.’ On the other hand, if they’re just routinely cutting every single woman, which is the case 98 percent of the time, for no medical reason other than to just speed things up for the doctor’s sake... It’s been deemed the second most unnecessary surgery in the United States, circumcision being the first.”
Some time ago, while channel grazing, I ran across an episode of Chicago Hope and heard a similar argument being made. The skeptical doctor retorted that tears, since they were not controlled like cuts, could extend all the way down into the rectum, a stomach-gripping thought. Flint’s advice for avoiding such extensive tearing:
“Number one — good nutrition. A good, balanced diet and lots of fluids keeps the skin soft and elastic. Number two, a few weeks before the due date, do the perineal massage exercise. Take your thumb and forefinger, lubricate them with oil, olive oil would be fine. Put the thumb inside the perineum, about an inch down, and your forefinger outside. Pull out enough that you feel it tug, and make the shape of the letter U, going up and down both sides of the vaginal wall. The whole time, you’re pulling out, away from your body, enough so that it feels like, ‘Owie,’ a kind of tingly sensation. You can do it in the tub — it makes it a little more comfortable. Just a few minutes every day, that’s been shown to help prepare the tissue.”
During labor, when the baby’s head is ready to exert pressure on the perineum, a warm compress maybe placed against the skin to act as a buffer. And if the mother is only semireclined, instead of flat on her back, the back of the baby’s head comes out first, as opposed to the face, which is larger.
Another argument for the controlled cut is that it is insurance against the danger of tearing upwards, into the clitoris. Janet Cunningham, a certified nurse-midwife I interviewed for this story, had this response:
“If the head just comes flying out, it can get really horrendous — it would be better to start an opening at the bottom. Then you would just get a tear to the bottom, which is much better. But if the mother’s comfortable, and everybody’s relaxed and patient, and you keep the head flexed, you can protect the upper structures. Just by gentle pressure down as the head crowns. You don’t have to press very hard—just enough to guide it.”
Upright position: “In America, most women are not allowed to be vertical during labor. Being able to walk helps the pelvis move out easier.” When I spoke with a licensed midwife, Michelle Freund, she showed me a series of slides of woodcuts and illustrations, dating from medieval to colonial times, which depicted women giving birth in upright to near up right positions. She contended that this has been the practice throughout history because this is what works.
No separation: Though this request applies to the time after birth, Flint sees it as crucial. Her first examples of the dangers of drugs had to do with postpartum effects — trouble focusing, leading to trouble seeing Mom, leading to trouble bonding and trouble breastfeeding. “I find it very interesting that babies are born with the ability to see just 12 inches, which is exactly the distance from the breast to the mom’s face. Holding your baby skin to skin, the baby will imprint on mother and bond with her, become close with her, much faster than if it weren’t breastfeeding.
“Not only will the baby learn to know the mother faster, but the mother will learn to know the baby faster. She will learn the baby’s different cues— the different cries. She will be able to respond to her baby much quicker, know what her baby wants. And by nursing, you tend to hold your baby more, so the baby will become more alert and responsive and smile a lot and make cooing noises and that sort of thing. It happens much earlier and more frequently because the two have connected so strongly.” She also points to the physical benefit of antibodies in breast milk and claims that it has been proven that babies who are breast-fed have slightly higher IQs than babies who are bottle-fed.
This is not a story about breast-feeding, but Flint sees contact and breast-feeding as an extension of the mentality that supports natural childbirth —the baby’s welfare above all else, even the extreme pain of labor. “The toughest part [about drugs] is that it can hurt the baby, and how could you possibly take that risk? I really have trouble dismissing that part. It’s only one day of your life. I don’t get why people are unwilling to do the best for their child. If somebody were to tell them, ‘Don’t worry about it, drugs aren’t going to affect your baby,’ I would say, ‘Are you absolutely sure?’ They can’t answer, ‘Yes,’ they just can’t.” Nevertheless, the pain is the reason why a lot of women receive drugs, and so the pain must be addressed. Part of our Bradley class involved training in pain management. “You squeeze your wife’s arm or her leg or something, hard enough that it hurts a little bit. You pretend that you’re in labor and having a contraction, usually about 90 seconds to 2 minutes. She needs to be able to breathe deeply, slowly, and relax all the muscles that are in her body, including the muscles that are in pain. Just become completely loose, and let her mind be free and use whatever mental and emotional ways of relaxation she can for those two minutes.”
Flint is a Christian; so is her class. “We do a great deal with prayer and Scripture reading. Most couples have particular prayers and particular Scriptures that mean a great deal to them. Often, it is the husband that is speaking these prayers to God for her, or speaking the Scripture to her, so she can be at peace.
“I don’t think labor is easy — I don’t think God intended it to be easy.” (Echoes of the curse put upon Eve when she left the garden — “In pain shall you bring forth children.”) “I think He wants us to look to Him for help. I don’t know if we would if we weren’t in pain. Christ went through a great deal of pain for us. He can bear our pain, if we just lean on Him.”
Besides the explicitly religious practices, Flint propounds a sort of meditation. “Imagery, of something beautiful in God’s world, like an ocean scene with waves coming in and out, which” is how the contractions are flowing in the body. Deep breathing is essential, it helps the muscles relax. And our muscles can work more efficiently when they’re well-oxygenated. It gives you more strength, more stamina, makes you feel more loosey-goosey.”

Though she knows “it’s a little out there for some people,” she advocates aromatherapy. “Lavender is very inductive of relaxation. Peppermint is good for revival, for stimulation. When she’s feeling too tired, like she can’t go on, let’s whip out the peppermint and give her some more oomph. It’s not magic, but I think it does help.”
Finally, she speaks of the emotional benefit of this particular physical pain. “I hate for it to sound kind of hokey or New Agey, but I think it’s very empowering for a woman to give birth on her own. I really believe it gives her a sense of ability in the rest of her life. When I have a difficult situation, like going to the dentist, or anything, I know that I have given birth, and I can do anything. I think it makes you a stronger person...you have this great ability to conquer your fears and your pains.”
We forgot the lavender and peppermint when we went to the Kaiser labor-delivery ward on May 6 of 1997. We didn’t do as much pain-management training as we should have. Deirdre vomited everything she ate or drank during labor, so the IV was necessary to prevent exhaustion and dehydration. But the nurses were good about letting her walk, keeping her on the monitor for about ten minutes an hour. As she lumbered around the halls in the labor-delivery ward, I wheeled the IV beside her, dropping to my knees when her contractions hit so that she could bend over and lean on me.
Deirdre was already at four centimeters when we arrived at around 3:00 a.m.; a few hours later, she was at six. Flint, whom we hired to serve as labor support, guessed that she still had a long way to go. But Deirdre’s curiosity got the better of her, and she opted for another exam around 9:30 a.m. To everyone’s surprise, and Deirdre’s surpassing relief, she was over nine centimeters; the certified nurse-midwife gave her the okay to push.
The bed was inclined into a semi-upright position and an overhead bar affixed to the sides. When she was pushing, Deirdre gripped the bar and squatted, shortening the birth canal and letting gravity lend a hand. Her voice went higher than I have ever heard it, a quavering roller coaster between moaning and screaming. Between contractions, she reclined on the angled bed. She came close to breaking once, and I had to play something of the heavy, holding to what we had decided, pushing her through her suffering. But she never asked for painkillers.
Part of what helped her was Paul’s line from Scripture about making up in our own bodies what is lacking in the suffering of Christ. She believed that her suffering could be efficacious, that it could be used to benefit others, in this case, her mother and her baby. She offered it up, a slightly different approach from Flint’s “leaning on God.”
When our son Finian crowned — when the top of his head began to press on the perineum — the midwife applied a warm compress and massaged the skin down around his head. Deirdre suffered a tiny tear, requiring one stitch. After the birth, Fin was placed on Deirdre’s stomach for a minute before being taken to a nearby table for weighing and examination. He never left the room, except when I took him to be circumcised the next day. Almost everything transpired as we had hoped it would, and the Kaiser staff were cheerfully accommodating.
Apart from the excruciating pain that Deirdre endured, we had a very pleasant birth experience, and Deirdre looks forward to giving birth at Kaiser again. But it doesn’t always work that way — hassles do happen. Though Flint can point to major improvements in doc-tor-Bradley patient relations — fathers in the delivery room, intermittent EFM, optional IV, optional episiotomy— she still sees a contrast in the way doctors and Bradley patients view birth.
“The doctor is there in case of emergencies; that is his forte. When the emergency comes, thank God he’s there.” The doctor, she says, drawing from her nine years as a medical assistant working with an OB, may be thinking more about preventing a lawsuit.
“Malpractice has really been the downfall of childbirth in this society. If the doctor feels he’s not able to do the things he wants to do for what he believes will be a more controlled, and in his opinion, safer birth—by constant fetal monitoring, by IV usage, and perhaps even C-section... [ If he does these things], he knows he did all the steps he could, by the book. If there is a bad out-come and the woman sues, then he can look back on medical records and say, ‘Well, I did everything I was supposed to do.’ ”
Increased worry over malpractice suits is not the only change doctors have had to endure. “In the ’50s and ’60s, nobody asked anything. You just were stuck. Then in the ’70s, women started to want their rights and wanted to know what was going on. Most women who are interested in natural childbirth are highly educated. It can be a little threatening to a physician — ‘Okay, what’s this woman going to want from me; what’s she going to do?’ ”
Flint tries to get her students to ease this anxiety. Besides employing the reassuring language of the birth plan, “I tell students to say, ‘This is what we believe in. We’re not going to ask you to do anything to endanger our child, we’re not that kind of people. We’re very reasonable. We’re going to do the best for — what we believe is the best for our child.’”
It’s a conciliatory statement, but there is still the tension in her self-correction: “what we believe is best for our child.” What happens when “what we believe” and what the doctor believes are at odds? “The doctor cannot force you to do any kind of procedure. They will just chart in your chart ‘Against medical advice’ to cover themselves.” I push, knowing that it is not always best to go to the hard case first, but curious where it will lead. What if the doctor believes the life of the baby is at stake, and the parents want him to stay out?
“I think it would be exceedingly rare,” opines Flint, “if it happened at all, that somebody went so far that they would not listen to what the doctor so strongly suggests. You’ll come to a point where you just have to believe that they know what they’re doing — more than you think. That is part of what I tell my students: you have to trust your doctor.”
Not everyone in the Bradley movement would agree. When my wife was pregnant and visiting her parents in Kansas City, she attended a Bradley class given by one of her parents’ neighbors. The last time she was there, she mentioned that I was writing this story and that I had interviewed Jay and Marjie Hathaway, executive directors of the American Academy of Husband-Coached Childbirth (AAHCC). The woman who taught the class then confided to Deirdre that Jay Hathaway was something of a crackpot.
Talking with Hathaway in his Sherman Oaks home, I could see how she came by this opinion. Hathaway is a layman who reads the medical journals — he calls it a hobby — an activity that arouses suspicion, like the man who spends all his time in the law library and tries to represent himself in court. “What is a nonprofessional doing snooping about in the professional literature?” the skeptic might ask. “How can he hope to understand what he finds, to draw the proper conclusions?”
Hathaway is given to incendiary statements, like “I used to believe that doctors didn’t know, that they needed to be told [about the risks of birth drugs]. But I’ve since changed my mind. I think they do know. I think they don’t care.” He is a man with an unpopular opinion — that the status quo about the tremendously important and intimate experience of giving birth is warped and dangerous — and years of combating the opposition of the medical establishment have taken their toll. He sometimes speaks with a peremptorily defensive manner, offering sharp comebacks to unspoken arguments that buzz invisibly about him.
But for all his vehemence and distress over the state of childbirth today, Hathaway is not a bitter man, not an angry man. He is a good-natured, comfortable father of six (three born with medication, three without), a friendly host, and a gifted storyteller. He seems to relish his role as medical maverick, taking comfort from history:
“I don’t know if you’ve read The Cry and the Covenant or know the name Ignaz Semmelweis,” he begins. “Semmelweis was an Austrian physician who discovered in approximately 1850 that childbed fever was caused by doctors’ hands. They went from an autopsy room, after examining a woman who had died of childbed fever, and they went down the hall, without washing their hands, and delivered a baby from some woman. This perfectly healthy woman was at enormous risk. Maternal death rates at all these big hospitals in Europe in the middle 1800s were between 10 and 30 percent. Today, women still die in childbirth, but it’s 1 in 10,000. They were enormous rates of death, and it was all from physicians. It was all because doctors weren’t washing their hands.
“Perhaps the most dangerous time in the history of the whole world to have a baby was 1850, especially if you were in one of the European capitals and went to a hospital. People at home weren’t having those kinds of death rates. People going to midwives weren’t having those kinds of death rates. Even the midwives within the hospital didn’t have those kinds of death rates.
“Semmelweis observed that doctors’ death rates were higher than midwives’, and one of the reasons he theorized for that was that doctors did autopsies and midwives didn’t. Now, this was an era when microbiology was not only unknown, it was disbelieved in. Pasteur and Semmelweis and all these pioneers, they were all in the middle 1800s. The whole knowledge of the human race about infection was turned upside down. Semmelweis tried to tell the doctors to wash their hands — if they would wash their hands, a lot of their patients wouldn’t die. And it was abhorrent to the doctors. They actually committed him to a psychiatric facility.
“He was just this crusading kind of physician. First, he started washing his hands. His patients didn’t catch this disease, which the teaching of the time said came from miasmas — clouds of death. Semmelweis said, ‘It isn’t a cloud of death, there’s something on your hands.’ He didn’t know exactly what it was.” He washed his hands in chloride of lime, and “he had, in his own practice, over 1000 consecutive cases without a single death at a time when other people were losing 10 or 20 out of 100.
“But the obstetricians of the time, and I have books even clear up into the 1920s, doctors were still arguing that Semmelweis couldn’t actually be right. Doctors couldn’t be the cause of the death of their patients, because they’re doctors. That mindset persists today.” By Hathaway’s own admission the maternal death rate today is minuscule compared o the 1850s, and most of the problems he sees with standard birth practices today do not have lethal consequences, but to him, the principle remains the same: Doctors refuse to change their behavior because they believe they are the ones who know what is best, regardless of what another doctor — in this case, Dr. Bradley—may say.
“Dr. Bradley’s basic premise back in 1947 was, ‘Nothing happens in nature without a reason. If something happens in a natural birth, there’s probably a reason for it, even if we don’t know what that reason is.’ That was profound. We have a lot of evidence today that we didn’t have then. Dr. Bradley wasn’t sitting there in 1947 saying, ‘In another 20 years, they’re going to start La Leche League — I better include breast-feeding. In another 30 years, they’re going to invent bonding, so I better do something about bonding.’
“His model was perspiring mammals. He grew up on a dairy farm. When perspiring mammals have a baby, they don’t have drugs, they don’t lie on their back, they aren’t restrained. The baby comes out, and the first thing every newborn mammal wants to do is breast-feed. Therefore, he theorized that it’s good for the baby to be held by the mother and to breast-feed.
“There was no proof then. There were no studies. Now, I can show you dozens, hundreds of articles on various aspects of the first few minutes after the baby is born and how important it is. He just said that if that’s what is natural, there must be a reason. I suggest that same philosophy should be applied to a lot of the things that are going on today.
“It isn’t as though the Bradley Method is a new thing that has to be judged by the current practitioners. It’s the standard against which you have to judge the interventions. An intervention, to be valid, has to have better rates of success than what would have happened with no intervention. There’s no sense in doing anything that isn’t going to make things better.” And as far as Hathaway can tell, the interventions, essential as they are in emergencies, rarely make things better.
Like anyone who spends time poring over reports and journals, Hathaway is a man full of numbers. “We’re 23rd in the world in infant survival. We’re doing more interventions, we’re using more drugs, we’re doing more cesareans. Our C-section rate nationally is around 20 to 25 percent. Just about a million cesareans will be done this year. You can’t do a million of any kind of major surgery without [risks]. In 1970, our C-section rate was 5 percent. We’re getting worse.”
More history and statistics, culled from a three-hour chat during which Hathaway slid easily from one topic to another, free-associating with the skill of a man intimately familiar with his subject: “Doctors love to point to the improvement in outcomes that has happened in this century, and it’s true. Early in this century was a dangerous, demographically speaking, time to have a baby. They claim they have been responsible for all of the improvement, and they claim that for all time up until then, it was always that way. True, there are many things today which are minor inconveniences, which a thousand years ago would have been fatal complications.” But it wasn’t “always that way.”
“In colonial New England in the 1600s, the average family had 7.1 children. Where did they get those children? The cesarean rate was zero, there were no epidurals, there was no stethoscope. Nothing your doctor has in his office had been invented in 1600, yet people had 7.1 children and lived to be roughly 70 years old.” Even for this century, Hathaway contests the notion that things have gotten dramatically better because of doctors’ interventions. “Doctors will point to graphs and say, ‘Look at the drop in infant mortality since the ’60s — we’ve dropped from 15 to 8.’ Yeah, but it’s 15 per 1000 to 8 per 1000. The overall infant mortality rate has fallen less than 1 percent, while the cesarean rate has gone from 2 percent to 23 percent. They point to this 1 percent drop and say, ‘This justifies doing a million cesareans a year.’ I don’t think it does any such thing.
“An awful lot of other things have happened in that era. When we had our first babies, in the ’60s, more than half the babies born vaginally in the U.S. were by general anesthesia. They don’t do that anymore. A lot of babies died from that, so when that went away, that was a big change.
“Plus, we have a weird new way of defining death. If you’re eight months pregnant and they do an ultrasound and they find out that your baby has no brain — if they do an elective abortion, that’s called a good outcome. It’s not an infant mortality. If you give birth to the same baby and then it dies, which it’s going to, that will be a bad outcome.
“In the first half of this century, more than half the babies born in the U.S. were born at home. It wasn’t until the 1940s that the number of hospital births exceeded the number of home births. The whole baby boomer generation was basically a hospital-born generation, for the first time in the history of the world. For right or wrong, the tail is wagging the dog right now; that’s the way everybody thinks is normal. Natural childbirth is thought of as an aberration, something weird.”
The Hathaways’ own involvement with the Bradley Method began in 1965. Marjie was pregnant with her fourth child. She tells the story: “I had already had three medicated births — knock-down, drag-’em-out obstetric routines. I kept thinking, ‘There’s got to be a better way.’
“Dr. Bradley came to Southern California, and we went to hear him speak. He said some interesting things. He said that women don’t need drugs to give birth to babies. I thought, ‘That’s insane.’ It hurt so bad with the drugs; how could he possibly say that women should give birth without drugs? Then he said that you should breast-feed the baby on the delivery table, and I said, ‘You can’t do that.’ I was always so groggy after giving birth, I thought the baby would fall on the floor.
“And then he says that you can walk out of the delivery room afterwards, and I was like, ‘Walk? Nonono.’ Because I’ve had births where I couldn’t walk for weeks afterwards. I can remember having to crawl on my hands and knees to get to the bathroom. He said, ‘You can get up and walk out of the delivery room, and then you go home two hours after the baby is born.’ This was totally unheard of.
“Jay and I talked about it, and we decided it couldn’t be any worse than what we’d already done. I went back to my doctor in the San Fernando Valley, and I told him all the things I wanted to do, and he looked at me and he said, ‘You’re crazy. No woman should give birth without drugs. No man should be in the delivery room.’ He didn’t agree with me about anything I wanted to do.” One Friday, her doctor examined her, told her she was at four centimeters, and said she’d have a baby that weekend. Tuesday morning, still pregnant, she boarded a plane for Denver, where Dr. Bradley practices medicine. The next day, she gave birth. “I didn’t require any drugs, Jay was with me the whole time, I breast-fed my baby on the delivery table, and I walked out of the delivery room.
“Dr. Bradley said, ‘Don’t come back to Denver every time you want to have a baby. Go to California and get something started.’ ” Using connections she had with La Leche, she began teaching interested people.
Jay Hathaway and the academy are the source for much of the information Nancy Flint offered, and I asked him about some of the claims she made, particularly with regard to birth drugs. The drugs and their effects —- stronger contractions, less pain — seemed to me the intervention most attractive to a woman in labor, and they are the intervention most strenuously opposed by Bradley supporters.
“Today’s drugs are still reaching the babies, and they’re still harming the babies,” begins Jay. “Even when they’re needed, you always have the potential for harm. There is a pamphlet that came out in 1974, and this is where a lot of people get the misunderstanding. They Said that regional anesthetics do not ordinarily enter the bloodstream and cannot reach the baby’s system. That’s a true falsity; it doesn’t enter the bloodstream, and it does reach the baby. In three to five minutes, it will transfer across the placenta into the fetus. That’s from the Physicians' Desk Reference.
“If you have any doubt about it, when you’re at a birth, watching them give an epidural, watch the fetal monitor. It’s immediate. The baby’s heart rate drops by about ten points almost immediately.”
When I ask about documentable problems that drugs cause for babies, Jay first cites the trouble breast-feeding that Flint talked about. The drug dries out the baby’s mouth, making it difficult for the baby to taste or smell Mom’s milk. “Oftentimes, these babies don’t want to nurse for at least three days,” says Marjie. This can interfere with bonding, as can the lethargy that comes with narcotics.
“Another problem,” says Jay, “is that the baby’s blood-brain barrier is immature. The blood-brain barrier is a kind of selective filter that your body has which allows nutrients and certain other molecules to get into your brain through the circulation to your brain more readily. It also prevents certain other things. If you give a woman in labor drugs, they may be getting to the baby’s brain more freely than to the mother’s brain.”
So what’s the danger? Jay Hathaway settles into another story. “Many years ago, there was a researcher named Yvonne Brackbill. One of the pieces of data that came out of her studies was that if the mother has drugs in labor, the baby’s IQ is three points lower. This maybe isn’t a huge amount; three points isn’t going to turn a genius into a moron. But I’d like my three points back.”
Brackbill’s results, which she called “conservative,” also stated the following: At 4 months, infants in the inhalant group [born to mothers under general anesthesia] “tended to laugh and coo less, had inappropriate placing and stepping responses, were less able to sit with help and hold their heads erect, and showed abnormalities in such physiological measures as heart rate, length, respiratory rate, blood pressure, and liver size.”
At 8 months, inhibited skills included “ability to respond to social play, sit alone, manipulate a bell, pick up a cube, and pull a string to obtain an object.” Tests at 12 months “revealed abnormalities in sweating patterns, locomotor and postural development, gait and overall neurological scores.” And in the case of Demerol, older children “are stunted in language and cognitive development.” (Quotes taken from an October 1978 article in Human Behavior.)
In 1979, Dr. Brackbill testified before a Senate subcommittee as to her findings. Hathaway, who attended the hearings, recalls that “the FDA’s first representatives were a pair of professional government research people. They had gone through the studies [that Brack-bill used as collaborative evidence] and found fault with every single one of these papers. ‘This study was not large enough; the control group wasn’t adequately controlled for this factor,’ etc. These were the only papers ever published in scientific literature on the safety of obstetric drugs.
“Yvonne Brackbill got up and basically, her testimony was, ‘Yes, each of these studies is in some way flawed.’ Her challenge was, ‘The overwhelming evidence suggests risk.’ Not one of these studies ever found a benefit of drugs to the baby. In every single case, they had found a deficit.” Brackbill’s study involved inhalant drugs used to put women to sleep during labor, as well as painkillers such as Seconal and Demerol. Epidurals generally employ bupivacaine or some other “-caine,” which carry their own risks. From a 1994 Chicago Tribune column by Doris Haire, president of the American Foundation for Maternal and Child Health: “A six-week follow-up evaluation by Deborah Rosenblatt in the United Kingdom of infants exposed to bupivacaine epidurals during labor demonstrated significant and consistent effects of the drug throughout the six-week assessment period. The initial effects were cyanosis (decreased oxygenation of the infant) and unresponsiveness. The infant’s visual skills, alertness, motor organization, ability to control states of consciousness and physiological response to stress were adversely affected.”
Further, a 1992 article in Developmental Medicine and Child Neurology summarized a study that examined the effects of bupivacaine epidural on infants’ performance on the Neonatal Behavioral Assessment Scale. “The epidural group showed poorer performance on the orientation and motor clusters during the first month of life.” Also, “Epidural mothers reported spending less time with their infants while in the hospital; post hoc analysis showed that they had longer labor, more forceps deliveries, and a greater amount of oxytocin [pitocin].... The results are discussed in terms of possible effects of the infant’s early disorganization on the mother-infant interaction.”
Finally, according to an article by Doris Haire in the spring 1987 issue of Childbirth Educator, “Epidural causes the pelvic musculature to become flaccid or limp, leading to dysfunction of the trough of pelvic muscles that normally rotate the baby into the proper position.” This may necessitate a C-section. Two studies conducted by Dr. James Thorp, associate director of maternal-fetal medicine at St. Luke’s Hospital in Kansas City, Missouri, concluded that women who receive epidurals are more likely to require C-sections for dystocia — the clinical name for bad positioning or a bad fit between the baby’s head and the mother’s pelvis. C-sections require general anesthetic, which brings us back to Dr. Brackbill’s findings.
Jay Hathaway admits the risks are small, that “bad outcomes” are relatively rare. But “even something that goes wrong one in a million times is going to happen two or three times a year. When you use any intervention which isn’t needed, there’s no benefit, so any risk at all to me is unacceptable.” Of course, Hathaway here and elsewhere raises the question of what “needed” means. Some women might argue that they need the drugs to kill the pain or help the labor; Hathaway is focusing primarily on the baby. Still, this doesn’t mean that he is ignoring the mother; he claims she faces risks as well.
“Everyone you talk to can give you a bad epidural story.” The sister of a friend of the Hathaways had a baby with an epidural. “It was one of the perfect ones. It worked great. There were no problems, no complications. The baby was fine. The mother was kind of shaky afterwards, which is not unusual. She didn’t have a headache; she was just shaking. They said, ‘Oh, that’s normal. Don’t worry about it. It’ll go away.’ Six weeks later, she’s still shaking, and her eyes are rolling back into her head. They sent her to a neurologist; he takes away her driver’s license and says, ‘These are seizures.’ She says, ‘Why am I having seizures?’ He says, ‘You had an epidural, didn’t you? I see it all the time.’ ”
Epidurals also increase the risk of postpartum fever. “If you’ve just had a baby, one of the things they do in hospitals is check your vital signs. If your temperature goes up, they assume you have an infection, and often, they separate you from the baby. It’s not particularly harmful, except that it interferes with the relationship with the baby. If the baby is withheld from the mother because of the fever, then it’s a bad thing.”
Besides epidurals, another possible cause Hathaway cites for the rise in C-section rates is the electronic fetal monitor. Here he supports the claim Flint made earlier. “When the EFM was introduced, the C-section rate was vastly lower. The first randomized controlled clinical trials ever done of fetal monitoring, done by a doctor in Denver named Al Haverkamp, showed a tripling of the cesarean-section rate. He had two groups: one monitored electronically and one not monitored electronically. The monitored group and the unmonitored group had the same rate of intrapartum and fetal deaths and damage. There was no improvement in outcome, but there were three times the rate of cesareans.” At least eight further studies have also concluded that EFM makes no difference in outcome.

Hathaway is a man conscious of the effect he is likely to have on the listener, and so he is careful to make certain admissions and concessions. First, he grants that “No way am I an objective observer. I am a biased person, and I am putting my bias out front. But my evidence is not fraudulent. I did not sit at my computer and fake an article from some medical journal. They really came from their journals, but I’ve selected them with my bias. There are doctors who will come up with opposing articles, but they’re biased too.” (All articles quoted in this story are included in the The Bradley Method Teacher's Manual)
While admitting his bias, he tries to avoid being seen as extremist. “You can’t just automatically say, ‘Drugs are evil and bad.’ Some babies, if you let nature take its course, aren’t going to survive, or they’re going to get damaged. [Some of these cases] can be effectively and fairly reliably treated with drugs or surgery or intervention. There are babies who are fine, normal, healthy babies, who would have otherwise been dead or damaged kids.
“But we’re saying that the natural way of having a baby is the safest possible way for 97 percent of the people. If you take that diagnostic and treatment modality [that you apply to emergency cases] and you apply it to a hundred out of a hundred people instead of just one person out of a hundred, somewhere in that group is going to be some other baby that’s going to be harmed. A phrase Dr. Bradley often uses is ‘irreducible minimum.’ There’s an irreducible minimum number of complications for any procedure you want to mention.”
As Flint pointed out, the Bradley movement has achieved certain victories — fathers in the delivery room being an important one. Says Hathaway, “Dr. Marshall Klaus, years ago, did a study where he took a bunch of women who were in labor and assigned them someone to remain with them. The people were not medical people, many of them were not even mothers, but they were female. The results were dramatically better. The statistics were phenomenal in decrease in the use of drugs, decrease in cesareans, increase in the satisfaction of the mothers.
“Bradley observed the same thing. In 1947, he was assigned a population of women in his residency in obstetrics, and he was doing an experiment with these women, a pronatural childbirth approach. These people volunteered to be in this thing. He was, in effect, their coach. He would spend their whole labor with them, and they did much better.” At first, Bradley thought he was a great coach, but then it dawned on him that someone else could do what he was doing, someone like the father.
“The most stressful thing you could possibly do to a woman in labor is put her in a hospital room, connect her to a bunch of machines, give her drugs or whatever you’re going to do, and leave her all alone.” Hathaway sees this as the cause of “enormous increase in drug use and interventions, and pitocin, and cesareans, because the woman is frightened and abandoned at that moment in her life when she needs support more than at maybe any other time in her life.” And in the years since the Bradley movement began, fathers in the delivery room have gone from being a rarity to being the norm.
Of course, if your baby is born at home, the presence of the father is a nonissue, as are most interventions. Michelle Freund is a licensed midwife living in Oceanside who provides pre- and postpartum care for women who want to give birth at home, as well as supervising labor and delivery. She is not a Bradley instructor, but she does preach natural child-birth. She is a friend of Flint’s and she shares her Christian friendliness, but there is something a touch more bristly about her.
Her home testifies to her beliefs and interests. Amid the pleasant decor, I notice small statues of pregnant women; framed drawings of pregnant women, discreetly nude; a U-shaped birthing chair. Fertility — fecundity — in all its earthy, swollen fleshiness, is held in high esteem.
Like the Hathaways, Freund’s involvement with natural childbirth started with personal experience. As a result of preparation for her own labor, she decided that “it seemed the normal thing to have a natural childbirth.... I just felt like every woman that I asked that had given birth either had negative things to say or didn’t want to talk about their birth. So, I thought, ‘There’s something wrong here.’ ”
Though she had planned on having a home birth, circumstances necessitated her going to a hospital. “It really reinforced to me how important it was that women were supported, that they have advocates in the hospital, that they learned and educated themselves. So, that’s how I started.” In 1987, she began working as a childbirth assistant, “being a bridge between hospital staff and the client, so that they could work towards a natural birth.” But the work proved frustrating.
“I’ll tell you frankly, when I was starting out [between ’87 and ’90], if it wasn’t for those home births I would attend periodically, I would not have been able to keep going into the hospitals with these couples. I would feel as though I actually saw physical and emotional abuse occurring, and there was nothing I could do.
“I’ve seen some awful things happen. One doctor in this county — this was probably seven or eight years ago... There was this new amni hook, which is what you use to break the bag of waters. This woman had a birth plan, and she was doing great. She was probably seven centimeters, and we had just walked into the hospital, because we did labor support at home.
“This new amni hook, it looked like a finger condom, and on the end of it was a sharp point. They’re obsolete now; there was a problem with the little tips coming unglued. He comes in, already gloved up, which was really unprofessional to begin with — you don’t walk in from the nurses’ station with gloves on when you check a woman, you put clean gloves on right there in front of her. He had his fingers tucked in the palm of his hand, and he went in and broke her water and acted like he never did anything.
“He didn’t say he had it on, and then he carefully turned toward the trash can, rolled his glove off, and discarded it so we didn’t see it. But I did see it, and I went in and found it in the trash. It was really underhanded, and it had complete disregard for the woman’s choice and her written preference, which he had. They were his standing orders from her — completely disregarded.
“I don’t know his intentions, but the audacity to play God like that... It saddens me. I hope there are very few doctors like that. At seven centimeters, it may not be troublesome to break the bag of waters, but there’s no guarantee it’s going to help the labor progress. It’s a sterile environment, so it protects the baby from any bacteria we introduce via internal exams. It also acts as a cushion for the baby’s head and helps dilate the cervix. And with the bag intact, there’s less chance of cord compression— the cord can float around. The bag is there for a good reason, and there should be a good reason to break it.”
Besides that, “I’ve seen women yelled at. I’ve seen women given episiotomies when they said ‘Don’t cut me’ and the baby was not in distress. I’ve seen women be told not to push because the doctor wasn’t there yet, and she’s in pain and she wants to push — and sometimes when you don’t push and you’re holding that baby back, it will cause distress for the baby. I’ve seen women nurses come in and keep offering medication, when they’ve been asked not to offer medication, and say things like, ‘Don’t be a martyr, you don’t have to do this this way, what’s wrong with an epidural?’ I’ve seen nurses come in and never even look at the mother or touch her, just push the button to get blood pressure, chart notes, and walk back out.
“I’ve seen babies whisked away unnecessarily. I’ve heard doctors railroad women into cesareans when they’re not necessary, making them feel hopeless, saying things like, ‘What do you want? Do you want a healthy baby?’ You know, Let s just get this over with’ instead of ‘These are the things we can do, and this is what I recommend.’
“Most women giving birth do whatever they’re told to have a healthy baby. But intervention doesn’t guarantee a healthy baby. There’s no guaranteeing with a cesarean that you’re going to get a healthy baby. I’ve taken moms in for cesarean, baby and mom were in great shape. By the time the doctor got there to do the cesarean — she just kept waiting and waiting—and the baby crashed during the cesarean. They drew it out and it took about see minutes to revive it.”
In spite of her experiences, she insists that she is “not antihospital or anti-doctor. I am against misusing technology.” For example, Freund once provided care to a woman whose pregnancy had gone to 43 weeks. She and the doctor she used as consultant were both concerned, and the doctor recommended a nonstress test to see if the baby was still healthy. The woman, opposed to intervention of any kind, refused. “I wish she would have done the nonstress test,” says Freund, looking back. I think it was harmless, but she was adamantly against it. I thought it was a good piece of technology to use at the appropriate time to assess the wellbeing of the baby.” As it turned out, the baby was fine.
But what if the baby hadn’t been fine? Mothers have been prosecuted for abusing babies in utero by drinking too much; could she have been prosecuted for some kind of neglect? Flint, Jay Hathaway, and Freund all admit that interventions are sometimes necessary for the health of the baby. But what happens when Mom refuses?
Freund supposes that “someone could try to bring up charges against her, because my doctor knew full well, and I knew full well, that she didn’t have the nonstress test. We had documentation.” But, she says, “at this day and age, if you can kill a baby in utero because of Roe v. Wade, then why should she be prosecuted for not choosing a piece of technology?”
Legal issues aside, Freund does not assume absolute neutrality. She told the mother, “ ‘Please think about how you might feel if your baby died in utero and could have been saved had you had the nonstress test.’ I have to feel like I’ve told [a woman] all the risks, and given her all the facts, and also will encourage someone to call and discuss it with the consulting doctor. I’ll say, ‘I think you need it.’ I’ll say that.”
Still, she says, “My perception of a good provider is, less is more. You want to inform them and give them all the standards of care and help them make educated choices, but we have to remember that we’re in bigger trouble if we make the choices for them. They’ve got to make the choices. Probably, if we’d stayed along those lines all along, there wouldn’t be the malpractice fears that there are today. I think that’s probably why midwives get sued a lot less, because they’ve got a great rapport with their clients, and they have their clients assume responsibility for making choices by giving them full informed consent and full disclosure and letting the couple determine what they want.
“I’m against coercing people to do things that might not be in their best interest but in the best interest of malpractice insurance or someone else’s agenda. I believe we need our hospitals, because we need comprehensive care should it be necessary. But the majority of women don’t need that kind of care. However, the majority of women choose that kind of care.
“It’s not the doctor’s fault. The feminist movement in the early 1900s said, ‘We can have painless childbirth, so we demand our Twilight Sleep [a general anesthetic].’ The women’s movement was the beginning of the end for natural childbirth.” Women who could afford painless childbirth went to the hospital and got it, while those who could not gave birth at home.
“Hospital birth gave you status, because rich people were having babies in the hospital.
“Then, it was the passive woman who said, ‘Well, here I am, doctor; do something for me. I’m paying you, so do something.’ ” But some people, “educated middle-class people,” still sought out midwives. “Midwives were underground for a long time. It wasn’t until, I think, 1955 that they started certifying nurse-midwives.”
Now, “there’s several routes you can go,” explains Freund. “The most traditional is apprenticeship, and that’s how midwives learned throughout the centuries. They would go with their mother or their auntie or whoever was the midwife, and they would go to the births and just learn. When that woman was too old, she passed the obligation to the younger person. There was always a village midwife somewhere.
“In today’s world, when you say ‘traditionally trained,’ you’re thinking the most mainstream training: becoming a registered nurse, taking a three-year midwifery program, and getting your certification as a certified nurse-midwife. Currently, the majority of certified midwives in California are certified nurse-midwives. However, the majority of those nurse-midwives work in an institution, be it a hospital or birth center.
“My personal opinion was that birth wasn’t an illness,” says Freund, “so it really shouldn’t take place in a hospital. I’m not learning about how to take care of somebody that’s sick. This is a normal physiological process; I’m learning how to take care of a natural process.”
So, after attending 38 hospital births as a childbirth assistant, she took what she considers the traditional route of apprenticeship. “I worked for three years from 1990 to ’93.” During that time, she assisted at “close to 200 deliveries. My third year, I did an internship with my midwife.” As an intern, Freund began taking on clients under the midwife’s supervision. “She is now licensed but was not at that time. She had 18 years of experience when I started working with her.”
In October of 1993, the California legislature passed the Midwifery Licensing Act, whereby midwives who are not nurses can become licensed if they take a three-year accreditation program and sit the state exam. The program involves “three mechanisms. Your clinical numbers — how many prenatal visits, newborn exams, deliveries, and labor managements you’ve done. Those charts need to be evaluated by an ob-gyn and a certified nurse-midwife and signed off.”
The charts are then submitted to the school (in Freund’s case, the Seattle Midwifery School). The school calls the patients to verify the data. The second mechanism is the school’s exam; the third is a clinical evaluation. “You have a doctor or a midwife sit in your clinic, making sure you do correct history intake, you inform the patient about nutrition, support, emotional support, and whatnot. You do an initial history intake, a First-trimester mom, a second-trimester mom, a third-trimester mom, a newborn baby, and a postpartum. Then you are evaluated on a simulated delivery of a baby and a placenta, a baby with a cord around its neck, and a simulation of an emergency pitocin injection and sterile technique and suture.”
For the simulated birth, “Most midwives have [artificial] babies that have the bones and stuff on the head.” Freund, who has served as a supervisor since becoming licensed in 1996, owns “an anatomically correct pelvis, and I also have membranes and a placenta, just made of fabric and cord. But for most people, you could do it as rough as pushing a baby through a piece of foam with a slit in it,” and pinning a piece of cord to the baby and a sponge-placenta.
The pitocin injection “is usually done on an orange, and the suturing is done on foam. I use markers and color the tissue” to indicate which layers are being sutured. It’s funny to think of a state license being given based partly on work with foam and oranges, but it seems to support her claim that managing birth does not require the depth of knowledge associated with most medical procedures.
After the clinical evaluation, “you can sit for the state exam” and become a licensed midwife. The obvious question is, how do you get the clinical numbers for the first mechanism if you’re not licensed? “If you’re not licensed, the only way you can get those numbers is to do it as an unlicensed practitioner. You can do it under the supervision of a certified nurse-midwife or doctor. A lot of midwives did work with licensed doctors years ago in this community. Today it’s a different story.
“We were all practicing without a license, and some have done it for 20 years. We did births because we believed in it, and women were going to give birth at home with or without a doctor’s permission. Eventually, they got off their butts and worked toward getting us a route by which we could be licensed, but we still had to be the guardians of home birthers, who were not going into an institution to give birth.”
Today, “there are still lay midwives practicing that don’t want to get licensed. We’re hoping that more will come forward and get licensed so that there is some type of regulating body for us. There wasn’t a regulating body, but I think that a lot of us, including myself, felt that this is what we were called to do. We had the skills, the training — the state needed to provide that [body]. So while I was waiting for them to provide that, I was practicing.
“I feel like it’s a calling for me. That’s one of the reasons I moved forward in midwifery without my license. I’m doing it in a very responsible way, whether or not I have that license. I had all the knowledge I needed to practice safely, to give good care, and my outcomes were fabulous. Today, I have very good outcomes. I have a very low transport [to hospital] rate; it’s less than 5 percent.”
Wasn’t unlicensed practice illegal? “It’s illegal to practice medicine without a license. However, the practice of medicine and the practice of midwifery can go side by side without crossing over.”
What if a medical emergency occurs? “You’re damned if you do and damned if you don’t. If I said, ‘I’m doing midwifery, but I’m not going to practice medicine,’ that means I shouldn’t use needles or tell somebody what to do for their kid. I can only give the things that I would do. But if you were doing midwifery without a license, and there was an emergency and you didn’t act appropriately, then you would be held more accountable than if you did the appropriate thing and practiced medicine and got the best outcome. That’s your responsibility. You take on the yoke of working with [moms in labor], then you darn well better be doing everything you can.”

Unless she transports a patient to the hospital, she is that patient’s primary care provider from pregnancy to postpartum and newborn care. But it’s labor that attracts the attention — it’s not hard to imagine other kinds of care occurring outside the hospital setting. I ask her to describe a sample labor.
“After all the prenatal care, and after doing a home visit where we check for supplies, test our pagers, check our maps to the house, and meet everyone who’s going to be at the birth, the client calls, says she is in labor. My fully trained assistant and I arrive. Mom might be in the tub or lying on the bed or up walking. [Besides the advantages Flint attributed to movement, Freund says that changing movement frequently “gives the baby an opportunity to move and mold and adjust to the pelvis and make its way through.”]
“Meanwhile, I would immediately listen to the baby with a Doppler or a fetuscope and check Mom’s vitals. My assistant would start setting up for the birth. Eventually, I would do an initial internal assessment to see what kind of dilation is happening. Often the woman is well progressed. Mom’s either up walking, alternating with lying down on her side resting; she might be in the shower. One woman would go from sitting to hands and knees, then to her Jacuzzi, then squatting. Then, settling down into my birth chair to push the baby out.”
Not that everyone has to use the birth chair. “If you leave her alone, a mother will more than likely automatically choose the best physical position for her.” Some give birth in the tub, some on their hands and knees, some squatting.
“Usually, there’s nice music. There’s usually a mother or two, or family members or a couple of friends. Some women will have a masseuse or an acupuncturist there to help them along with labor. There’s always a lot of women. Women like to invite other women to their births, just for the nurturing.
“Either Dad catches the baby or I catch the baby. We put the baby on the mother’s chest. There’s a lot of tears and joy and laughter. My assistant is there watching the baby, making sure the baby has good heart rate and respirations, good color. I’m watching the mother, checking her fundus because we still have to deliver the placenta. Hopefully, we get the baby on the breast to cause uterine contractions, and that causes the placenta to detach and deliver.
“Either Mom wants to get up and shower, if she’s strong and stable, or we clean her up and tuck her into bed and monitor her throughout the time the assistant is cleaning up and they’re bonding.” The baby gets an exam, everyone gets something to eat, and then everyone goes to bed.
So goes the sample, what about the 5 percent that need to go to the hospital? When does that happen? “If I thought that Mom was getting exhausted and progress is slow.” Exhaustion can bring on “lack of mobility, dehydration, they start to burn their fat stores. If the mom gets exhausted, sometimes the baby gets exhausted. If the mom gets dehydrated, the baby can spike a fever. If a woman’s vomiting and she can’t keep any fluids down, and she’s got this long, laborious labor, she’s not going to be in good shape.
“If I listen to contractions, and after contractions, to see how the baby’s heart rate is, how the baby’s heart rate responds to contractions — and mostly it’s always beautiful — if there’s something there that I don’t like, if there’s deceleration, then I’m going to listen more carefully and make my assessment. I might change the mother’s position. I might give the mother oxygen. I might push the baby against the pelvis. Different things to see how the baby responds. If there’s fetal distress, then I’m going to call the hospital and explain to the parents and move into that setting. I’m not hesitant to transfer when it’s needed.”
I can’t help it; I keep thinking about the pain. I keep thinking that the pain is the sticking point, the obstacle that would keep a woman from considering natural childbirth. What do you say to that? “This is a natural physiological function,” responds Freund. “Your body was designed to give birth. It doesn’t have to be painful. The more educated you become, the more you trust and understand the process, the less painful it should be. So if you exercise, you educate, you eat well, you look forward to the birth, you should have a nice, natural birth.”
It doesn’t have to be painful? “The pain is a process that reminds you of what you’re doing. It helps you grow. I’ve been to support groups for women who have had cesarean sections, and they have a huge loss, because they didn’t experience the birth of their baby. And most American women don’t, because they’re on an epidural. I think that we’re all into this fast-food, express this, express that, let’s just schedule my baby and get this over with kind of thing, because we don’t have time for unplanned, spontaneous things.
“It brings us to our natural limits. Women will say, I’ve never done anything as hard.’ Well, what’s wrong with that? Empowerment is what you get when you birth your baby naturally, and you lose your power when you give up that right to a natural birth.”
Like Flint, Freund is a Christian, and when dealing with Christian patients, she invokes their common faith. “You talk about trusting God, knowing that He won’t give you any more than you can handle, surrendering, being the empty vessel, bringing forth His blessings, all those things. You talk about Philippians 4:13: ‘I can do all things in Christ Jesus who strengthens me.’ Visualization, seeing Him, seeing yourself in the palm of His hand, or cuddled up in the arms of Jesus, things like that, where they can have that kind of thing to grasp on.
“The majority of those certified nurse-midwives work in an institution, be it a hospital or birth center.” Freund may be right in saying this, but that is not to say that a hospital and a birth center are the same. During our interview, Freund pointed out that some hospitals are dressing up their labor-delivery wards to look like bedrooms, to make the mother more comfortable. But, she said, if the doctor is still an interventionist at heart, the dressings are superficial.
The dressings are there at Best Start Birth Center on Fourth Avenue in Hillcrest, but the homey atmosphere does not mislead. Janet Cunningham and Roberta Frank, both certified nurse-midwives, believe wholeheartedly in natural childbirth; their professional liability insurance requires that they work here in the center. They also like that they are hospital-close in case transport is necessary— Mercy is just down the street.
Freund showed me some pictures of labors when we spoke. One stuck in my mind: a photo of a woman, naked from the waist down, seated on the concrete of her patio, back against the wall of her house. Her knees were drawn up and spread apart. Her head was tilted back, eyes closed. A long, liquid trail flowed from her vagina across the concrete patio; her water had just broken. The photo was arresting; my wife gave birth naturally, but not this close to nature. Not all of Freund’s moms deliver this way, but I wondered if maybe the institutional setting of the Birth Center might be a sort of middle ground between the hospital and the home, appealing to a greater range of people. Freund might argue that I was institutionally tainted — that I viewed it as a more secure, safe place than home, when home is the real paragon of security and safety—and maybe she would be right. But I’m also right about the broad appeal of the Birth Center.
“We have moms who home-school their children,” says Cunningham. “We have moms who go right back to work. We’ve got women who drive trucks, who are attorneys, who work in medical offices. We have women of all races; we have women who are Muslim and real fundamental Christian religions. It’s just so fascinating. They’re here because they believe they’ll have a better experience. I think they just trust nature.”
Cunningham and Frank share Freund’s view of intervention: “I think that doctors interject a lot more than they should into the birth,” says Cunningham. “It’s a natural process. That’s kind of the culture of medicine. We’re actually seeing a little bit of theoretical work done, research. It’s like a cascade. You do one procedure, whether it’s EFM, and then you don’t know if you might need a C-section, so we’re not going to let the mother eat anything. So we have to give them an IV.
“While the nurse is with another client, or if she just doesn’t want to labor sit — you can’t always expect the dads to be there — maybe she chooses an epidural when all she needed was to be able to walk around and have somebody rub her back and tell her that she’s doing a beautiful job. Then with the epidural, maybe the blood pressure goes down even though they gave her fluids, and so you can end up with the C-section. All the things they do can sort of cascade and you end up with an outcome you never would have expected, and then the attitude is, ‘Oh, isn’t it wonderful that we have our suites right here and anesthesia right here.’ Maybe if they weren’t right there, things would have been different.”
As evidence, Frank tells this story: “I’ve had two people come to me and tell me about their past birth experience where the doctor has said that the baby’s probably too big and won’t be able to fit through. I think they ended up getting induced or having a cesarean section, and the babies weighed less than my son — he was eight pounds, nine ounces — and they had bigger hips than I do. I just feel like, a lot of times, it’s scheduled because it’s more convenient for the doctors. I don’t know if that’s true, but... ”
Cunningham concurs. “We see that in our practice all the time — a woman wants a vaginal birth after a previous section. A catchall reason for doing a cesarean is ‘failure to progress’ or cephalopelvic disproportion. Then, lo and behold, she has a successful vaginal birth after cesarean, and the second baby is bigger than the first. A lot of it has to do with geometry. A large baby that’s lined up well will usually fit through. We encourage moms to be up and moving. Elastic binders can sometimes help, especially if it’s baby three or four and the mom’s just kind of pendulous, and the baby’s just hanging out there. Cinching the baby up gives you a good drive angle—it’s so old-fashioned, so low-tech.”
“There’s a lot of old tricks that have been forgotten,” adds Frank. “When birth became technical — when women were confined to bed and wearing monitors and the C-section rate went up — physicians became really good surgeons, and their expertise wasn’t as good at supporting normal birth. My mother was an OB nurse in the ’40s, and I have her old textbook. There’s a chapter on position changes the mother can do to turn the baby.
“Sometimes, they’ll schedule a C-section if the baby’s head is overriding the pubic bone. They’ll say the pelvis is too small. But in my mother’s book, there’s a picture, it shows specifically a position the mother can assume to rock the head below the pubic bone and into the pelvis. We did it, and it worked.”
More low-tech intervention: when Cunningham gave birth to her own son here, “I was pushing, and in the last stage of pushing, we were getting some moderate decelerations of his heartbeat. At one point, the concern was, ‘Are we going to transfer to the hospital?’ I was in a full squat — really using gravity to bring him down — but in between [pushes], Roberta pushed his little head back up to get some of the pressure off
“I really believe that if I were in a hospital, I probably would at least have had a vacuum extraction, and I would have had a cut from here to there, maybe. If we needed to transfer, we would have, but if it had been in a hospital, I really don’t think an OB would have thought to push his head back up. I remember thinking, ‘Oh, he’s going the wrong way,’ but it worked. It relieved the pressure on his head, and he was born just fine.”
Transfers are sometimes necessary—they estimate about 12 percent — especially for first time moms exhausted from long labors. “That’s when the hospital really helps,” says Frank. “That’s when an epidural really helps. Mom goes in and she can sleep for a couple of hours, not have any pain for a couple of hours. After a good sleep, labor usually rallies, and she’ll go on to have a vaginal birth. That’s a good use of the system. Let everybody try normal, and if normal isn’t working for them, then rely on medicine.”
The problem, as Hathaway pointed out, is that “normal” no longer means “natural.” Cunningham used to work as a labor-and-delivery nurse at Ohio State. “I got subsumed into the culture. I heard OBs in labor and delivery say, ‘Birth can only be normal retrospectively.’ ” Columbus, Ohio, was a town in which it was easy to get sued _ “they have the second highest per capita population of lawyers in the country” — so doctors had to be careful, and that meant intervention. “Everybody had monitoring, and there was a high C-section rate. One thing that really disturbed me was a woman, uncomplicated, normal healthy labor, had an elective epidural for pain management. We did everything right, but her blood pressure bottomed out, and the baby’s heart rate bottomed out. The anesthesiologist gave her fluid and some medication. Her blood pressure came up, but the baby’s stayed down.
“There was a mad dash to the OR. We had to do a crash section, and of course you had to have general anesthesia. I’m with her in the recovery room and she’s asking how her baby’s doing, and her baby was fine. She’s thanking the OB and the anesthesiologist for saving her baby’s life, and everybody’s eating it up, saying, ‘We’re glad to be here. This is why hospital birth [is good].’ Nobody told her that it totally happened because of the epidural.” Drug dosages have since been decreased, but the story stands as an example of both the “cascade effect” of interventions and the interventionist mentality the women oppose.
Frank “tried to work in a hospital, but I just couldn’t do it. I couldn’t support the system at the expense of the client. You’ve got so much work that needs to be done, you have to document.. .you find yourself doing things for no other reason than it comes from the administration that you have to do it. It doesn’t matter that it doesn’t fit any of the people that are there having babies.” She did have a hospital practice as a certified nurse-midwife, along with three others, “for about sue months, back in 1979. The administration at UCSD Medical Center thought we were a great idea and gave us all privileges right out of school. But the OB department and the anesthesia department had different ideas. We found out we couldn’t practice midwifery there. I think they were afraid we were just too controversial. Things were going well; they liked things just the way they were.”
When hospital transfers do occur, Cunningham and Frank call on Dr. Dale Lapp. Though he looks like any other doctor (I was expecting maybe a wild-haired madman?), he does not fit the intervention-minded doctor image I had been given. Rather, he is what proponents of natural childbirth wish for, a man willing to intervene if necessary but who says, “We have all the high-tech hospital things available if they’re needed, but the fact is, a lot of the time they’re not. It seems like women who do natural childbirth — without anesthesia — have just a little bit better experience, a little bit easier recovery.”
When I ask Dr. Lapp for his take on the pain question, he responds, “There was a study done on women who wanted to deliver without anesthesia. They did psychological testing to just evaluate how sure they were they could do that. The women who were very sure they could do it, that had the right attitude, almost all of them did it. The ones that asked for anesthesia were the ones that weren’t really sure they could do it.” While he lacks Hathaway’s outrage regarding drugs, he does say that “anesthesia drops blood pressure, and that can reflect in fetal heart tones,” indicating fetal distress. “It takes away the urge to push, so sometimes the second stage of labor can be prolonged, and that can really tire the mother out. My sense and my experience is that, if you meddle too much, that’s where your complications come from.” What he says is not new to my ears, what is new is that I am hearing it from a doctor.
This story by no means provides a complete account of the natural childbirth issue. Nor does it address all the issues doctors face — insurance and malpractice issues, issues of time and space in hospitals, and the like — in any great detail. It is also admittedly one sided — no pro-intervention doctors were interviewed. But, as Jay Hathaway said, “The current power structure is so large, it’s like some enormous ocean liner. I’m some guy in an itty-bitty rowboat saying, ‘Turn the Titanic around, and keep away from that iceberg.’” Intervention is the standard; this story is intended to give voice to those who propose an alternative.
Comments